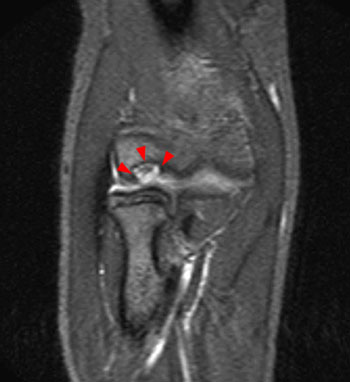
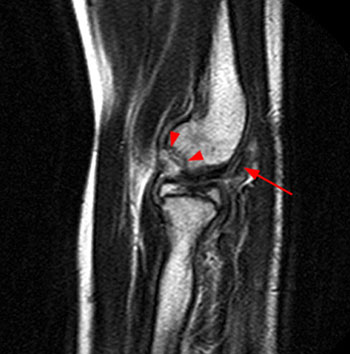
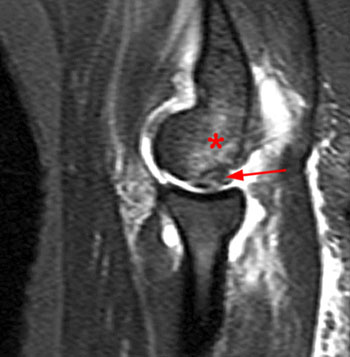
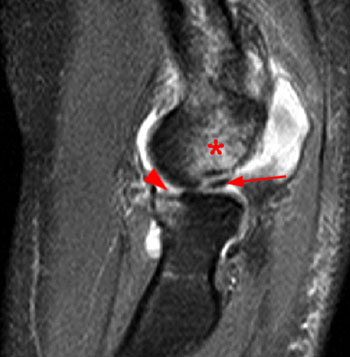
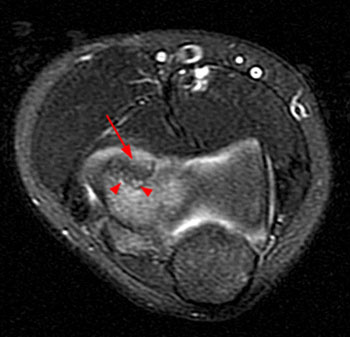
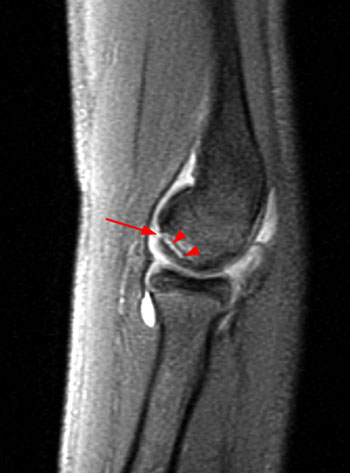
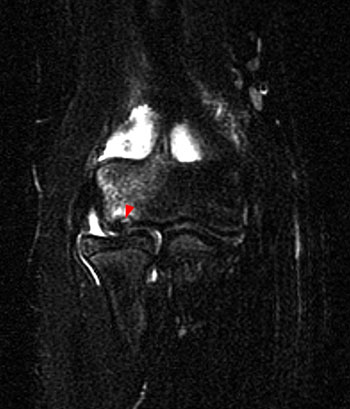
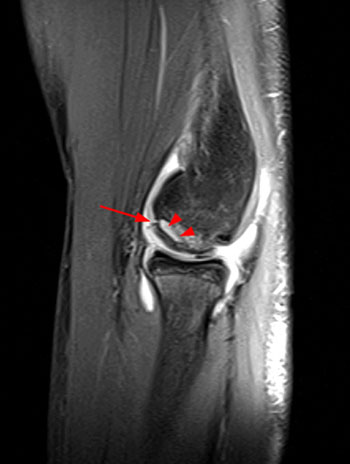
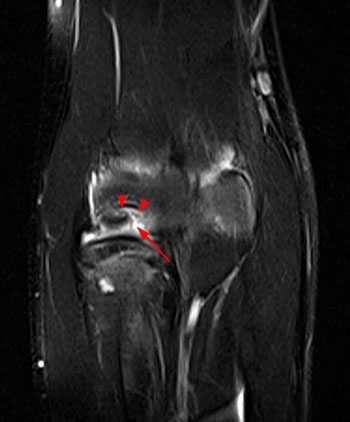
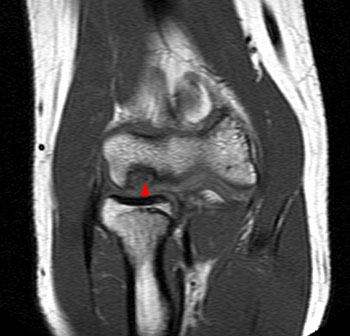
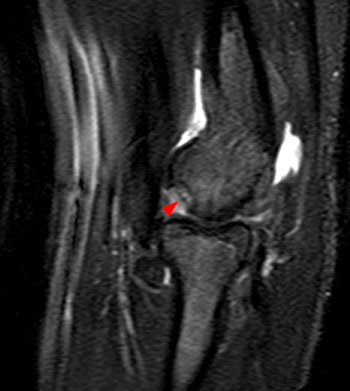
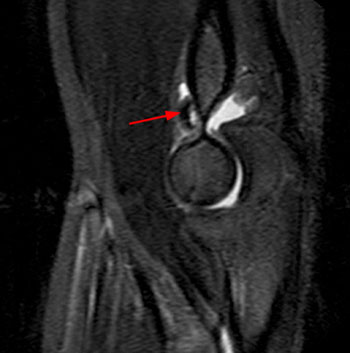
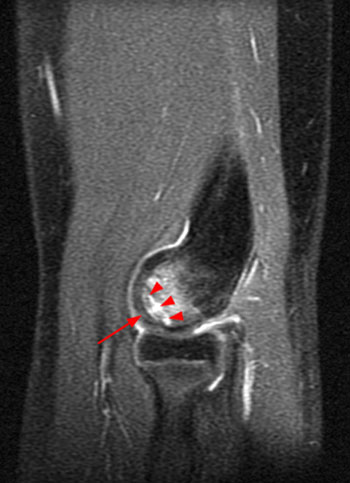
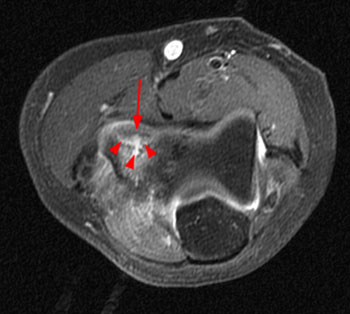
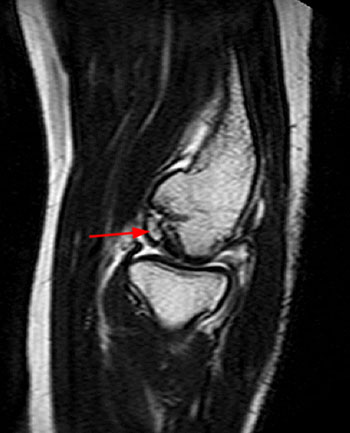
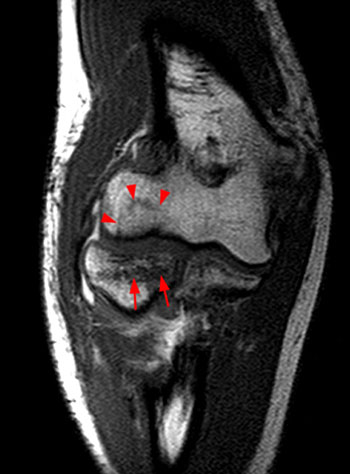
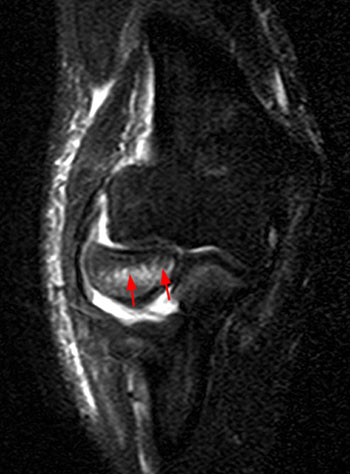
Clinical History: An 11 year-old female gymnast presents with right elbow pain and popping with flexion. Coronal inversion recovery (1A) and sagittal T2-weighted (1B) images are provided. What are the findings? What is your diagnosis?
Figure 1:
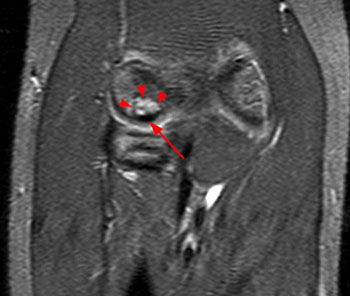
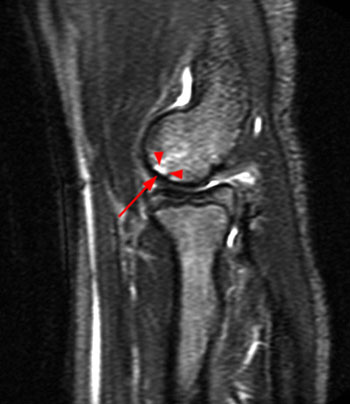
Coronal inversion recovery (1A) and sagittal T2-weighted (1B) images demonstrate an osteochondral defect of the anterior aspect of the capitellum (arrowheads). The margins of both the articular cartilage and subchondral bone are disrupted with fluid-like signal within the defect. The displaced osteochondral fragment (arrow) lies posterior to the capitellum on the sagittal image. Note the open proximal radial physis in this skeletally immature patient.
Diagnosis
Unstable osteochondritis dissecans of the capitellum with a displaced osteochondral fragment.
Introduction/Background
Although confusion remains between the terms osteochondral injury and osteochondritis dissecans, it is really the etiology of the process that is in question. An osteochondral injury involves the separation of a segment of articular cartilage along with its underlying bone. It is a general term used to characterize the pathology encountered at the joint surface with no consideration of etiology. Mechanically, an osteochondral injury is produced by either repetitive and prolonged joint overloading or a sudden impact that results in high compressive stress to the tissue and high shear stress at the subchondral bone junction. This mechanical stress can occur in the setting of normal or abnormal underlying bone. The basic types of osteochondral lesions that occur in the elbow include acute posttraumatic fractures and the osteochondroses, including Panner’s disease and osteochondritis dissecans.
Osteochondral Injury
Panner’s Disease
Panner’s disease is an osteochondrosis of the humeral capitellum. It primarily affects male athletes between 7 and 12 years of age and occurs during the period of active ossification of the capitellar epiphysis. Patients typically present with pain, swelling, and tenderness over the lateral aspect of the elbow. Radiographs show rarefaction and flattening of the capitellar epiphysis with poorly defined cortical margins. Fragmentation, fissuring, and sclerosis of the capitellum can also be observed1. The entire capitellar epiphysis is typically involved. This is one feature that distinguishes Panner’s disease from osteochondritis dissecans, which usually involves only the anterolateral aspect of the capitellum. Panner’s disease is always a benign, self-limited condition. Articular bodies never form, and the capitellar epiphysis eventually assumes a normal appearance as growth progresses. Due to its benign clinical course, MR imaging is rarely used to evaluate patients with Panner’s disease. However, MR may show diffuse bone marrow edema within the capitellar epiphysis in symptomatic individuals2.(Figure 2)
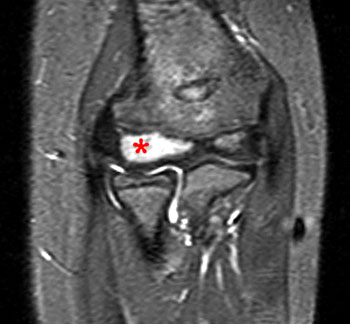
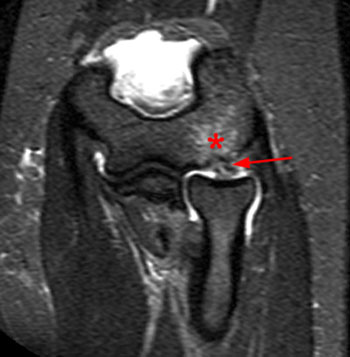
Figure 2:
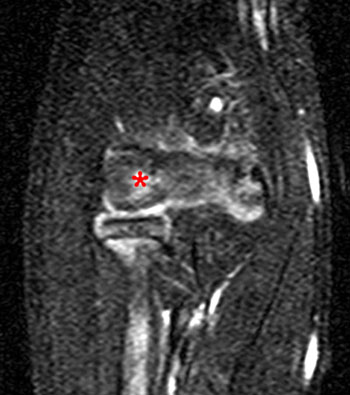
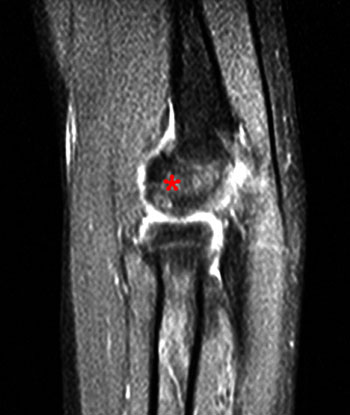
11 year-old male with elbow pain. Coronal T1 (2A) and coronal fat-suppressed proton density weighted (2B) images of the right elbow demonstrate diffuse low signal intensity on T1-weighted images and diffuse high signal intensity on proton density-weighted images throughout the entire capitellar epiphysis (asterisks). Overlying articular cartilage is intact.
Osteochondritis Dissecans
When occurring in the elbow, osteochondritis dissecans refers primarily to lesions of the anterior aspect of the capitellum, although lesions of the trochlea, radial head, olecranon, and olecranon fossa have been described1. Osteochondritis dissecans of the capitellum primarily affects male athletes between 12 and 15 years of age and occurs at a time when the capitellar epiphysis is almost completely ossified3.
Most authors agree that a combination of injury from repetitive trauma and a tenuous blood supply to the capitellum leads to osteochondritis dissecans. The capitellar epiphysis receives blood from only one or two isolated vessels that enter posteriorly and traverse the capitellum. No metaphyseal collateral flow exists, resulting in a tenuous blood supply4. This limits the ability of the epiphysis to heal between episodes of trauma, rendering it susceptible to osteonecrosis. Genetic factors and biomechanical differences in the articular cartilage of the capitellum and radial head may play a secondary role in the pathogenesis5, 6.
As previously noted, this is an entity most commonly seen in adolescents and young adult males. Usually the dominant arm is affected and in most cases there is a history of overuse of the involved upper extremity. Common sports in which these patients participate are baseball, racquet sports, gymnastics, and weightlifting. Pain is the primary symptom at presentation. The onset of pain is insidious and progressive and tends to be activity related. Palpation of the radiocapitellar joint can elicit tenderness, but often this pain is dull and poorly localized. Another common finding is loss of motion, most often extension. If crepitus to palpation accompanies clicking, popping, or locking, the clinician should be highly suspicious for articular cartilage fragmentation and articular body formation.
Osteochondral Fracture
Shearing and impaction fractures of the capitellum can also occur (Figure 3), but are less common than Panner’s disease and osteochondritis dissecans. In distinction to these anterior capitellar disorders, impaction injuries can involve the posterior capitellum, at the junction of the capitellum and distal radius. These posterior osteochondral fractures are often associated with fractures or contusions of the anterior aspect of the radial head and coronoid process. An association with injuries of the lateral ulnar collateral ligament has been reported in up to 82% of cases7. This suggests the posterior capitellar impaction injuries are associated with elbow instability and may be caused by transient dislocation. These injuries can be distinguished from the pseudodefect of the capitellum by the presence of marrow edema and the presence of articular and subchondral abnormalities of the posterior capitellum.
Figure 3:
Coronal (3A) and sagittal (3B) inversion recovery images of the left elbow in a 45yo female who injured her elbow while lifting. A displaced osteochondral fracture of the posterior capitellum is demonstrated (arrow)with associated hemarthrosis and acute marrow edema (asterisks). Not shown are complete tears of the annular ligament and lateral ulnar collateral ligament and a partial tear of the radial collateral ligament. Transient dislocation was suspected. Sagittal(3C) fat suppressed T2-weighted image of the left elbow in another patient. This is a 46yo female with pain and popping following a fall. Osteochondral fractures of the posterior capitellum and anterior aspect of the radial head are demonstrated. Not shown are high-grade partial tears of the common extensor origin and lateral ulnar collateral ligament. Again, transient dislocation was suspected.
Imaging of Osteochondral Injury
The imaging approach to the osteochondral injury, regardless of etiology, should be the same. The goal of imaging is first to diagnose the abnormality, then characterize it with regard to extent of involvement, stability of the lesion, associated complications, and finally to offer imaging information that may suggest acuity of the injury as well as possible etiology. Although MR imaging has been established as the most sensitive and reliable means for assessment of osteochondritis dissecans8, radiographic evaluation routinely precedes MRI in the evaluation of elbow pain.
The radiographic detection of osteochondral lesions can be challenging. Some authors have suggested that obtaining anterior-posterior radiographs in 45 degrees of flexion can aid in the radiographic detection of subtle lesions4. In general, the characteristic radiographic imaging appearance of an osteochondral lesion includes radiolucency and rarefaction of the osseous articular surface, most commonly involving the capitellum (Figure 4A). Morphologic alterations of the articular surface can be present in the form of flattening and irregularity of the subchondral bone. Additional alterations in the subchondral bone include areas of sclerosis, sclerosis with adjacent lucency, or subchondral cyst formation. Fragmentation at the articular surface and articular bodies suggest unstable lesions.
As previously noted, MRI has emerged as the most sensitive and reliable means for the assessment of osteochondral lesions. The MR diagnosis is made by identifying signal change or morphologic abnormality at the articular surface. In general, signal intensity changes in the subchondral bone that are low on T1-weighted images without fragmentation or lacking high signal intensity at the lesion interface on fluid-sensitive sequences are considered stable in nature. (Figure 4) The MR signs of an unstable lesion include a high signal intensity interface between the lesion and normal bone on fluid sensitive sequences (Figure 5), a high signal intensity defect in the articular cartilage at the lesion margins (Figure 6), and a focal articular surface defect. (Figure 1, Figure 7)
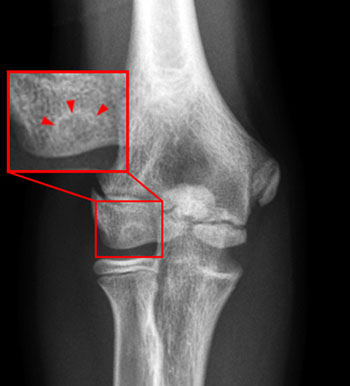
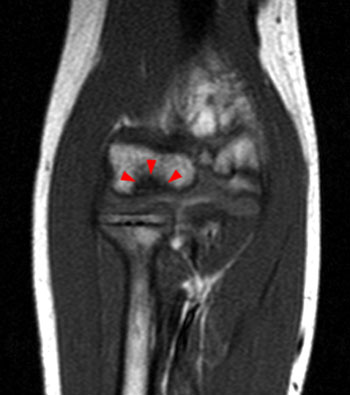
Figure 4:
Frontal radiograph (4A) of the right elbow in a 13yo male who complained of pain when throwing a baseball. A subtle region of trabecular rarefaction within the capitellar epiphysis is surrounded by a thin sclerotic margin (arrowheads). Coronal T1-weighted (4B), coronal T2-weighted (4C), and sagittal fat suppressed proton density-weighted (4D) weighted MR images of the same elbow. A region of marrow edema lies within the capitellum (asterisks) with a thin low signal intensity margin on T1-weighted images (arrowheads). Overlying articular cartilage is intact. This represents a stable osteochondral lesion.
Figure 5:
Coronal T1-weighted (5A) and inversion recovery (5B), sagittal inversion recovery (5C) and axial inversion recovery (5D) images of the right elbow in a 13 year-old male with 2 months of elbow pain while throwing. A curvilinear lesion within the anterior aspect of the capitellar epiphysis (arrows) is surrounded by high signal intensity on fluid sensitive images (arrowheads) and several small adjacent cyst-like lesions are seen. This represents an unstable, non-displaced osteochondral lesion.
Figure 6:
Sagittal proton density-weighted fat suppressed (6A) (6C) and coronal T2-weighted fat suppressed (6B)(6D) images obtained of the right elbow in a 12 year-old male with 6-8 months of elbow pain and popping. The anterior osteochondral fragment is undermined by fluid-like signal (arrowheads). A defect is demonstrated within the articular cartilage at the superior margin of the lesion (arrows). Images (6C) and (6D) were obtained three months after the initial images and demonstrate further lesion detachment with bone resorption beneath the lesion. However, the fragment remains in situ and is not completely detached. This represents an unstable loose-in-situ lesion.
Figure 7:
Same patient as Figure 5, examination obtained 10 months after the study in Figure 5. Coronal T1-weighted (7A) and sagittal inversion recovery (7B)(7C) images of the right elbow. The unstable fragment is now displaced with a fluid-filled defect within the anterior capitellum (arrowheads) (7A,7B). On a more medial sagittal image (7C), the displaced fragment presents as an articular body (arrow)within the coronoid fossa.
Three basic types of lesions have been identified: stable, unstable but attached, and unstable and displaced. Stable lesions by definition are in situ and have intact overlying articular cartilage. Unstable lesions are those in which the articular cartilage is disrupted. The unstable lesion can remain attached and in situ or can detach and become displaced, articular bodies. It is for this reason that MR arthrography has improved staging accuracy for osteochondral lesions4. By placing contrast material into the joint, the extension of contrast material to the interface between the fragment and adjacent normal bone establishes the presence of a defect in the articular cartilage, confirming the presence of an unstable lesion9.
The use of intravenous gadolinium-based contrast has also been described in the evaluation of stability and viability of osteochondral lesions. Fragment enhancement after intravenous contrast administration suggests an intact blood supply and viability of the fragment. Diffuse enhancement at the fragment-subchondral bone interface may indicate an unstable fragment. If enhancing granulation tissue is present, then the fragment is assumed to be separated and unstable by some authors4, 10. (Figure 8)
Figure 8:
Sagittal fat suppressed T1-weighted images obtained before (8A) and after (8B) the administration of intravenous gadolinium contrast material and axial fat suppressed T1-weighted (8C) post-contrast images of the right elbow in a 13 year-old male with an osteochondral lesion(arrows) related to pitching. Diffuse contrast enhancement adjacent to the lesion with marked enhancement at the fragment-subchondral bone interface (arrowheads)suggests granulation tissue and an unstable fragment.
Treatment/Clinical management
Features affecting the success of treatment of osteochondritis dissecans are fragment size, stability, viability, and location. Each of these should be evaluated and reported in the imaging assessment of the elbow. Lesion size has been associated with clinical outcome. Larger defects involving more than 50% of the articular surface or involving the lateral margin of the capitellum may have worse outcomes after debridement and may be better treated with fragment fixation or osteochondral autograft transfer11. Fragment stability, as described above, can be assessed with MR imaging. Information regarding fragment viability can be ascertained with MR imaging following the administration of gadolinium-based contrast material. This information is potentially useful because it could ultimately predict which lesions are likely to heal with nonoperative management. The location of the fragment is typically at the anterior capitellum, but coexisting radial head lesions have been described and could affect both treatment and outcome4.
Nonoperative treatment is reserved for patients with stable and viable lesions without mechanical symptoms and consists of activity modification to avoid the inciting trauma. Approximately 50% of early osteochondral lesions with stable and viable fragments heal with nonoperative therapy12. It has been advised that return to sport is governed by symptoms as imaging studies can remain abnormal for years4. Surgical intervention is indicated for patients who do not respond to initial nonoperative management and for patients with unstable and nonviable lesions at presentation. Surgical intervention consists of internal fixation of the fragment using bioabsorbable screws, debridement of the fragment with drilling or microfracture of the underlying subchondral bone, or the use of an osteochondral graft13. (Figure 9) The predictors of a poor long-term outcome are large fragment size, unstable lesion on presentation, progression of lesion severity over time, and development of secondary osteoarthritis11.
Figure 9:
Contiguous T2-weighted (9A,9B) sagittal images obtained in a 18 year-old male with a sports injury to the right elbow three years ago and failed nonoperative management. A large detached, fragmented osteochondral lesion is seen (arrows). The patient was treated with placement of an osteochondral graft with improvement of symptoms.
The patient fell one year following surgery and was reimaged. Coronal T1-weighted (9C), fat suppressed T2-weighted (9D) and sagittal fat suppressed proton density-weighted (9E) images from the post-operative examination. The faint outline of the healed osteochondral graft is seen on the T1-weighted coronal image (arrowheads). Capitellar marrow signal is normal with intact overlying articular cartilage. A radial head fracture (short arrow) is the result of his fall.
Conclusion
Elbow pain seen in the at-risk athlete, such as a baseball player or gymnast, should raise suspicion for osteochondritis dissecans. It is characterized by localized injury of subchondral bone of the capitellum. To determine the best treatment option, it is important to differentiate between stable and unstable osteochondral lesions. Stable lesions can be treated with rest, whereas unstable lesions, as well as stable lesions that do not respond to nonoperative therapy, may require a surgical approach. Magnetic resonance imaging is the diagnostic study of choice to evaluate capitellar osteochondral lesions and loose bodies and to accurately determine the stability and viability of the fragment so that the appropriate treatment can be initiated.
- Stubbs MJ, Field LD, Savoie FH. Osteochondritis dissecans of the elbow. Clin Sports Med. 2001;20:1-9. ↩
- Stoane JM, Poplausky MR, Haller JO, et al. Panner’s disease: x-ray, MR imaging findings and review of the literature. Comput Med Imaging Grah. 1995;19:473-476. ↩
- Brown R, Blazina ME, Kerlan RK, Carter VS, Jobe FW, Carlson GJ. Osteochondritis dissecans of the capitellum. J Sports Med 1974;2(1):27-46. ↩
- Bradley JP, Petrie RS. Osteochondritis dissecans of the humeral capitellum. Diagnosis and Treatment. Clin Sports Med. 2001;20:565-590. ↩
- Schenk RC Jr, Athanasiou KA, Constantinides G, Gomez E. A biomechanical analysis of articular cartilage of the human elbow and a potential relationship to osteochondritis dissecans. Clin Orthop Relat Res 1994;299:305-312. ↩
- Paes RA. Familial osteochondritis dissecans. Clin Radiol 1989;40(5):501-504. ↩
- Rosenberg ZS, Blutreich SI, Schweitzer ME, Zember JS, Fillmore K. MRI features of posterior capitellar impaction injuries. AJR 2008;190:435-441. ↩
- Takahara M, Ogino T, Takagi M, Tsuchida H, Orui H, Nambu T. Natural progression of osteochondritis dissecans of the humeral capitellum: Initial observations. Radiology 2000;216:207-212. ↩
- Steinbach LS, Palmer WE, Schweitzer ME. Special focus session. MR arthrography. Radiographics. 2002;22:1223-1246. ↩
- Peiss J, Adam G, Casser R, et al. Gadopentetate-dimeglumine-enhanced MR imaging of osteonecrosis and osteochondritis dissecans of the elbow: initial experience. Skeletal Radiol. 1995;24:17-20. ↩
- Takahara M1, Mura N, Sasaki J, Harada M, Ogino T. Classification, treatment, and outcome of osteochondritis dissecans of the humeral capitellum. J Bone Joint Surg Am. 2007 Jun;89(6):1205-14. ↩
- Mihara K, Tsutsui H, Nishinaka N, Yamaguchi K. Non-operative treatment for osteochondritis dissecans of the capitellum. Am J Sports Med 2009’37(2):298-304. ↩
- Smith MV, Bedi A, Chen N. Surgical treatment for osteochondritis dissecans of the capitellum. J Bone Joint Surg Am. 2007 Jun;89(6):1205-14. ↩