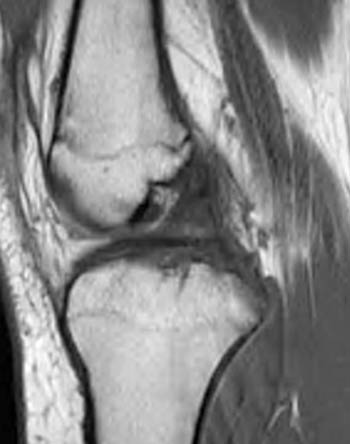
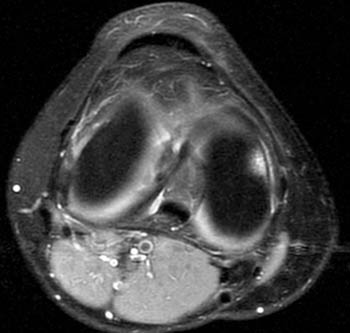
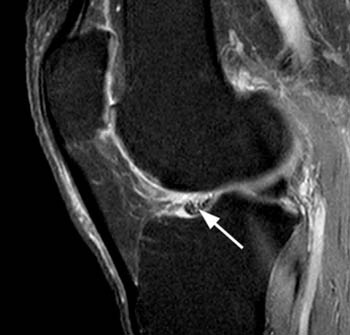
Clinical History: A 14 year-old female presents with medial knee pain after a basketball injury. (1a) T1-weighted sagittal and (1b) fat-suppressed proton density-weighted axial images are provided. What are the findings” What is your diagnosis?
Findings
Diagnosis
Oblique Meniscomeniscal Ligament
Introduction
The C-shaped fibrocartilaginous menisci aid in joint stabilization and load transmission. Meniscal tears are among the most common etiologies of knee pain and suspected meniscal tears are the most common indication for MRI of the knee. Magnetic resonance imaging (MRI) has proven to be an excellent tool in the evaluation of meniscal tears and associated pathology. MRI’s high spatial resolution, excellent soft tissue contrast and multiplanar capabilities make it ideal for evaluating suspected injuries of the menisci, articular cartilage, ligaments, tendons, muscles, and bone marrow.
When interpreting MR images of the knee, it is essential to be aware of the normal anatomic variations and normal anatomic structures that can mimic meniscal tears. The oblique meniscomeniscal ligament is but one of several known structures that can mimic meniscal pathology. Other established anatomical variants include the transverse meniscal ligaments and the meniscofemoral ligaments, which mimic meniscal tears at their meniscal attachment sites. Additional “pitfalls” in the evaluation for meniscal tears include the popliteus tendon, the meniscal ossicle, and the ‘speckled or spotty” anterior horn of the lateral meniscus.
Discussion
The oblique meniscomeniscal ligaments are intermeniscal ligaments with a reported prevalence ranging from 1%-4%.1-3 The oblique meniscomeniscal ligaments are named based on their anterior attachment site. The medial oblique meniscomeniscal ligament (2a, 3a, 4a, 5a) attaches to the anterior horn of the medial meniscus and the posterior horn of the lateral meniscus, while the lateral oblique meniscomeniscal ligament attaches to the anterior horn of the lateral meniscus and the posterior horn of the medial meniscus.
Both the medial and lateral oblique meniscomeniscal ligaments transverse the intercondylar notch, passing between the anterior and posterior cruciate ligaments. The cruciate ligaments are intra-articular but extrasynovial structures. Although an oblique meniscomeniscal ligament can mimic a bucket handle tear, the extrasynovial passage of the ligament between the cruciate ligaments distinguishes it from a flipped bucket handle tear, especially in the presence of an otherwise normal appearing meniscus (Fig. 4). Additionally, knowledge of this variant allows one to identify it by its typical course from the anterior horn of one meniscus to the posterior horn of the other.
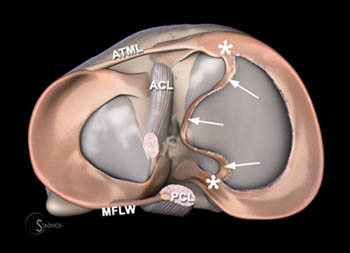
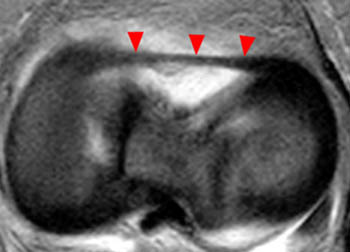
Figure 4:
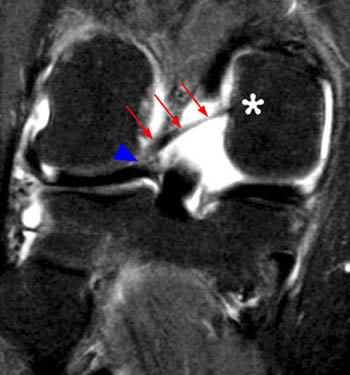
(4a) This graphic representation of the knee from above with the femur removed demonstrates the medial oblique meniscomeniscal ligament (arrows), which attaches at the anterior horn of the medial meniscus (asterisk), passes between the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL), and attaches at the posterior horn of the lateral meniscus (arrowhead). (4b) In contrast to the medial oblique meniscomeniscal ligament, the "bucket handle" fragment (arrows) of a bucket handle tear of the medial meniscus attaches at the anterior and posterior horn of the medial meniscus (asterisks). The anterior transverse meniscal ligament (ATML) and meniscofemoral ligament of Wrisberg (MFLW) are also demonstrated.
Figure 5:
(5a) Sequential coronal fat-suppressed proton density-weighted images from anterior to posterior demonstrate the course of the medial oblique meniscomeniscal ligament (arrows), coursing from the anterior horn of the medial meniscus to the posterior horn of the lateral meniscus. Note the normal size of the medial meniscal body (arrowheads), which would be foreshortened if this were a bucket-handle tear.
The anterior transverse meniscal ligament (Fig. 4, 6a, 7a) attaches to the anterior horns of both menisci, while the much rarer posterior transverse meniscal ligament attaches to the posterior horns of both menisci. The anterior transverse meniscal ligament is present in approximately 60% of knees, and the posterior transverse meniscal ligament is present in 1-4% knees.1-3 These ligaments can also mimic meniscal tears at their meniscal attachment sites.
The meniscofemoral ligaments of Humphrey and Wrisberg extend from the posterior horn of the lateral meniscus to the medial femoral condyle (Fig. 4, Fig. 8a). The ligament of Humphrey extends anterior to the PCL, while the ligament of Wrisberg extends posterior to the PCL. Meniscofemoral ligament incidence is 70-100%, and in about 2-3% of knees the ligaments of Humphrey and Wrisberg are both present.5 On sagittal images of the knee, an intermediate signal intensity interface is often seen at the attachment of a meniscofemoral ligament to the posterior horn of the lateral meniscus (Fig. 9a), and unless one is aware of this variant structure, the appearance can be confused with a meniscal tear.
Figure 9:
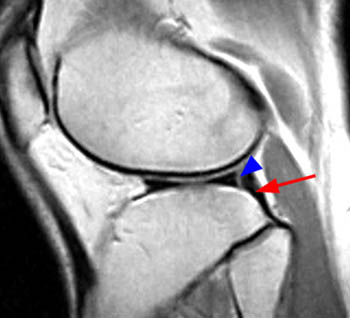
(9a) A proton density-weighted sagittal image near the root of the posterior horn of the lateral meniscus demonstrates the intermediate signal intensity interface (arrow) between the ligament of Wrisberg (blue arrowhead) and the posterior horn of the lateral meniscus (red arrowhead). This normal appearance should not be confused with a meniscal tear.
The popliteus is a flat, triangular, deep posterior compartment muscle, which arises by a strong tendon from the outer side of the lateral femoral condyle and has a broad muscular attachment to the posterior shaft of the tibia. The popliteus tendon and tendon sheath pass posterior to the posterior horn of the lateral meniscus, where one can see the “pseudotear” appearance (10a), a potential pitfall in meniscal evaluation.
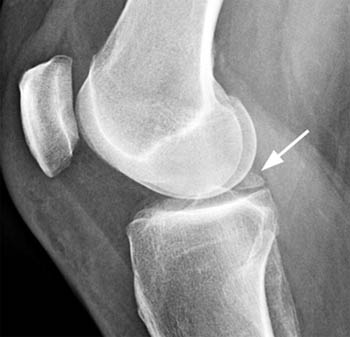
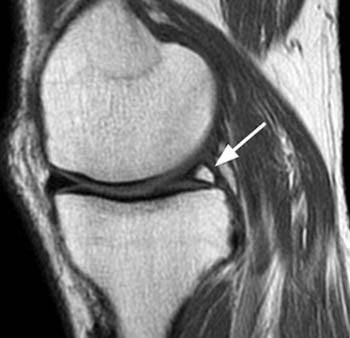
The etiology of the meniscal ossicle is uncertain, but these may be post traumatic or vestigial structures which can be asymptomatic or can be associated with local pain. They occur most commonly in the posterior horn of the medial meniscus, and on plain films (11a), are often mistaken for loose bodies. MRI is able to demonstrate the typical intrameniscal location of a meniscal ossicle (12a), and can be used to identify the occasional associated meniscal tear.
The anterior horn lateral meniscus/ anterior lateral meniscal root can have a ‘speckled or spotty” appearance in up to 60% of patients, which is likely secondary to the adjacent/crossing fibers of the anterior cruciate ligament insertion.6 This ‘speckled” appearance can mimic a tear of the anterior horn lateral meniscus (13a).
Conclusion
High spatial resolution, excellent image contrast and multiplanar capabilities make MRI an excellent tool in the evaluation for meniscal tears. Normal anatomic variations and normal anatomic structures can mimic meniscal tears to the untrained observer. Knowledge and understanding of these “pitfalls” is integral in the accurate interpretation of MRI images of the knee, as false positive MRI interpretations can lead to inappropriate or unnecessary treatment.
References
1 Zivanovic S. Menisco-meniscal ligaments of the human knee joint. Anat Anz 1974;135(suppl 1-2):35-42.
2 Dervin GF, Paterson RS. Oblique meniscomeniscal ligament of the knee. Arthroscopy 1997;12:363-365.
3 Radoievitch S. Les ligaments des menisques interarticulaires du genou. Ann Anat Path Anat Normale Medico-Chirugicales 1931:8:3-11.
4 Heller L, Langman J. The meniscofemoral ligaments of the human knee. J Bone Joint Surg Br 46:307,1964.
5 Hassine D, Feron JM, Henry-Feugeas MC, et al. The meniscofemoral ligaments: Magnetic resonance imaging and anatomic correlations. Surg Radiol Anat 14:57, 1992.
6 Shankman S, Beltran J, Melamed E, Rosenberg Z. Anterior horn of the lateral meniscus ” another potential pitfall in MR imaging of the knee. Radiology 1997; 204:181-184.
7 Resnick D. Diagnosis of Bone and Joint Disorders, 4th Edition. W.B. Saunders Company. Phila., PA; 2002.
8 Sanders TG, Linares RC, Lawhorn KW, Tirman PF, Houser C. Oblique Meniscomeniscal Ligament: Another Potential Pitfall for a Meniscal Tear ” Anatomic Description and Appearance at MR Imaging in Three Cases. Radiology 1999;213:213-216.
9 Sanders TG, Miller MD. A Systematic Approach to Magnetic Resonance Imaging Interpretation of Sports Medicine Injuries of the knee. American Journal of Sports Medicine, 2005;33:131-148.
10 Schnarkowski P, Tirman P, Fuchigami K, Crues J, Butler M, Genant H. Meniscal Ossicle: Radiographic and MR Imaging Findings. 1995;196(1)47-50.
11 Shogry ME, Pope TL. Vacuum phenomenon simulating meniscal or cartilaginous injury of the knee at MR imaging. Radiology 1991; 180: 513.
12 Herman LJ, Beltran J. Pitfalls in MR imaging of the knee. Radiology 1988;167:775-781.
13 Watanabe AT, Carter BC, Teitelbaum GP, Seeger LL, Bradley WG. Normal variations in MR imaging of the knee: appearance and frequency. AJR 1988;153:341-344.
14 Carpenter @A. Meniscofemoral ligament simulating tear of the lateral meniscus: MR features. J Comput Assist Tomogr 1990;12:1033-1034.