Clinical History:
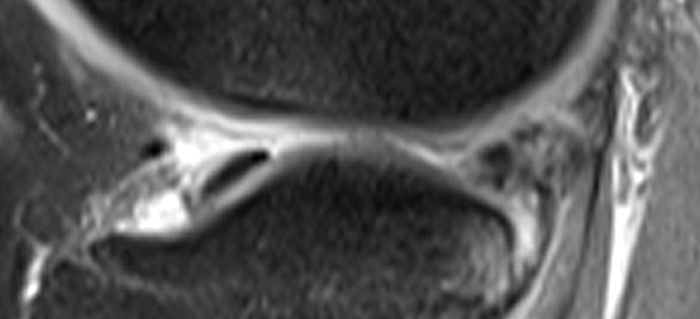
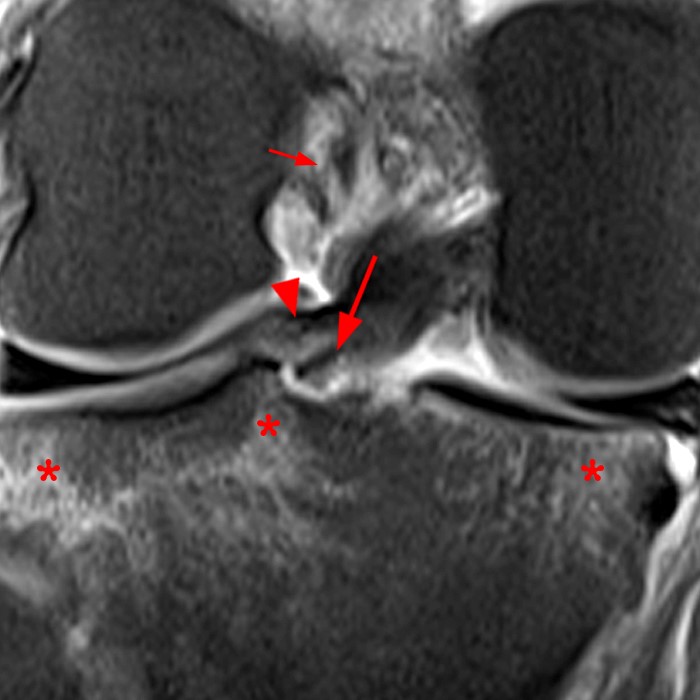
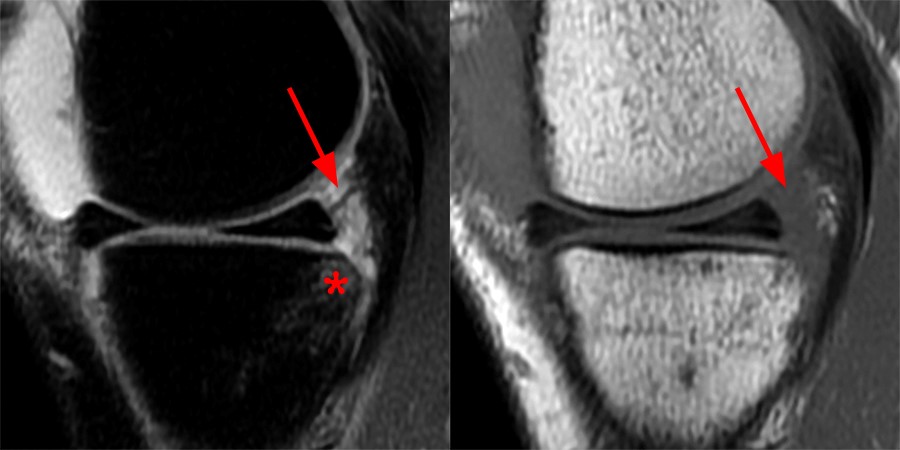
A 16 year-old female presents after twisting her knee while playing basketball 7 days prior. Cropped fat-suppressed proton density-weighted coronal (1A) and sagittal (1B) images are provided. What are the findings? What is the most likely major ligament injury?
Findings
Figure 2:
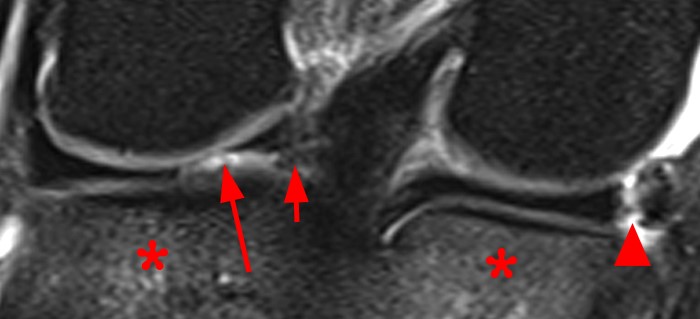
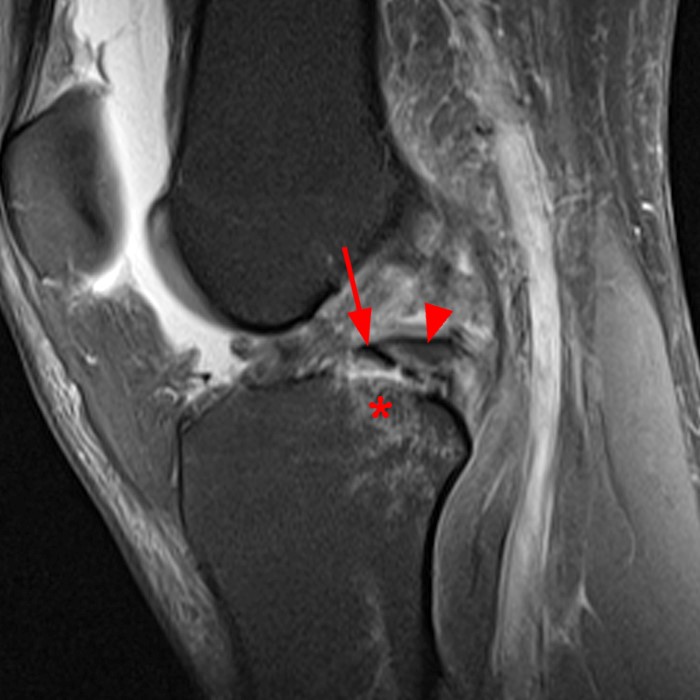
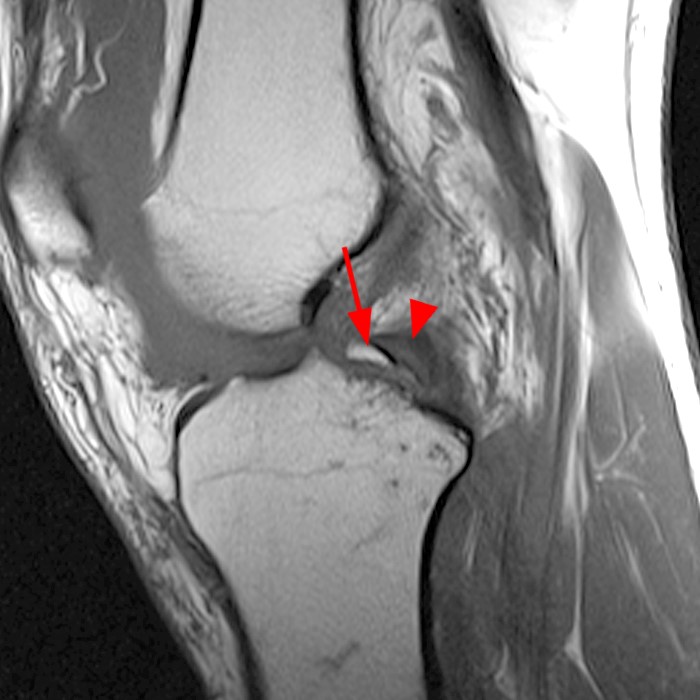
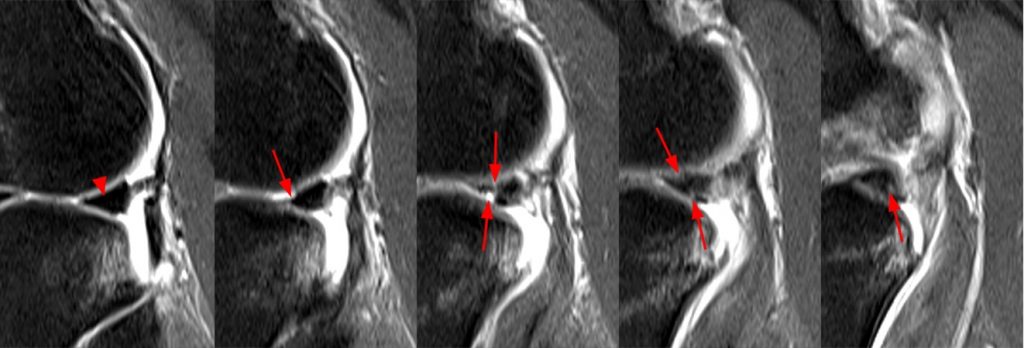
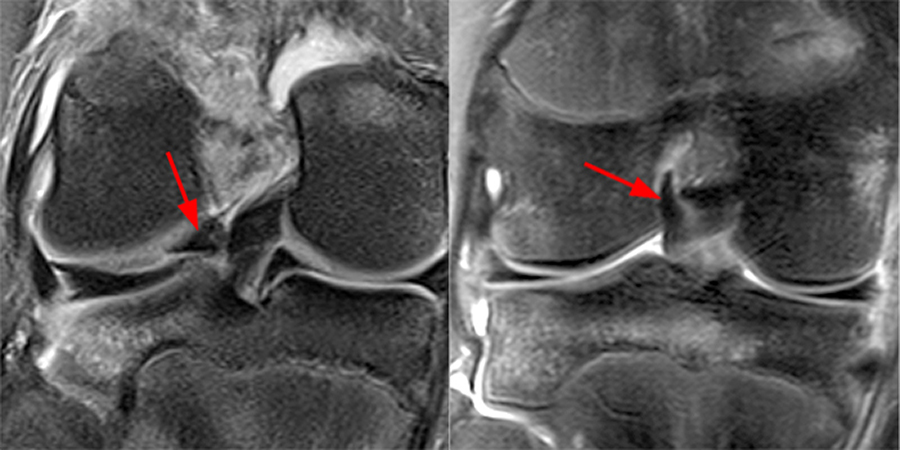
The coronal fat-suppressed proton density-weighted image (2A) demonstrates a focally irregular and truncated contour of the posterior horn of the lateral meniscus near the posterior root (arrow) which is confirmed (arrow) on the sagittal fat-suppressed proton density-weighted image (2B). A small displaced meniscal flap (short arrow) is seen adjacent to the PCL. A longitudinal tear is present at the periphery of the posterior junction of the medial meniscus (arrowhead). Bone bruises (asterisks) are noted at the medial and lateral aspect of the posterior tibia.
Diagnosis
Medial and lateral meniscal tears characteristic of anterior cruciate ligament (ACL) disruption.
Introduction
With the extreme forces and altered biomechanics that result in ACL disruption, it is not surprising that associated meniscal tears are extremely common. Acute ACL tears have a reported incidence of meniscal tear in up to 82% of cases, and chronic ACL tears have a reported incidence of meniscal tear in up to 96% of cases. Failure to recognize and treat meniscal tears at the time of ACL reconstruction can have long-term consequences, including accelerated arthritis and instability that can contribute to ACL graft failure. This Web Clinic discusses several meniscal tear patterns that have a high correlation with ACL tears and may be subtle and easily missed without the appropriate search pattern.
In addition to meniscal tears, ACL tears are associated with multiple additional structural injuries including ligamentous, capsular, osteochondral, and tendinous injuries, which are beyond the scope of this discussion.
Relevant Anatomy
The medial and lateral menisci are C-shaped, semilunar, fibrocartilage structures commonly divided into an anterior horn, body, and posterior horn. When viewed perpendicular to the inner edge, the menisci are triangular or wedge shaped, appearing tapered centrally at the inner free edge with a concave superior surface articulating with the femur and a flat inferior surface articulating with the tibia. Each meniscus has peripheral attachments to the capsule and tibia and firm attachments to the tibia anteriorly and posteriorly via the meniscal roots.
The medial meniscus is larger than the lateral meniscus in the anterior to posterior dimension and increases in width from anterior to posterior resulting in a larger posterior horn compared to the anterior horn. The medial meniscus covers up to 60% of the medial tibial plateau.1 In addition to the anterior and posterior root ligament sites of attachment, the medial meniscus is firmly attached at the meniscal periphery to the deep component of the medial collateral ligament and to the tibia via the meniscotibial (coronary) ligament. The medial meniscus is more tightly anchored than the lateral meniscus and can translate approximately 5 mm in the anterior-posterior plane which allows femoral rollback during flexion.2
Figure 3:
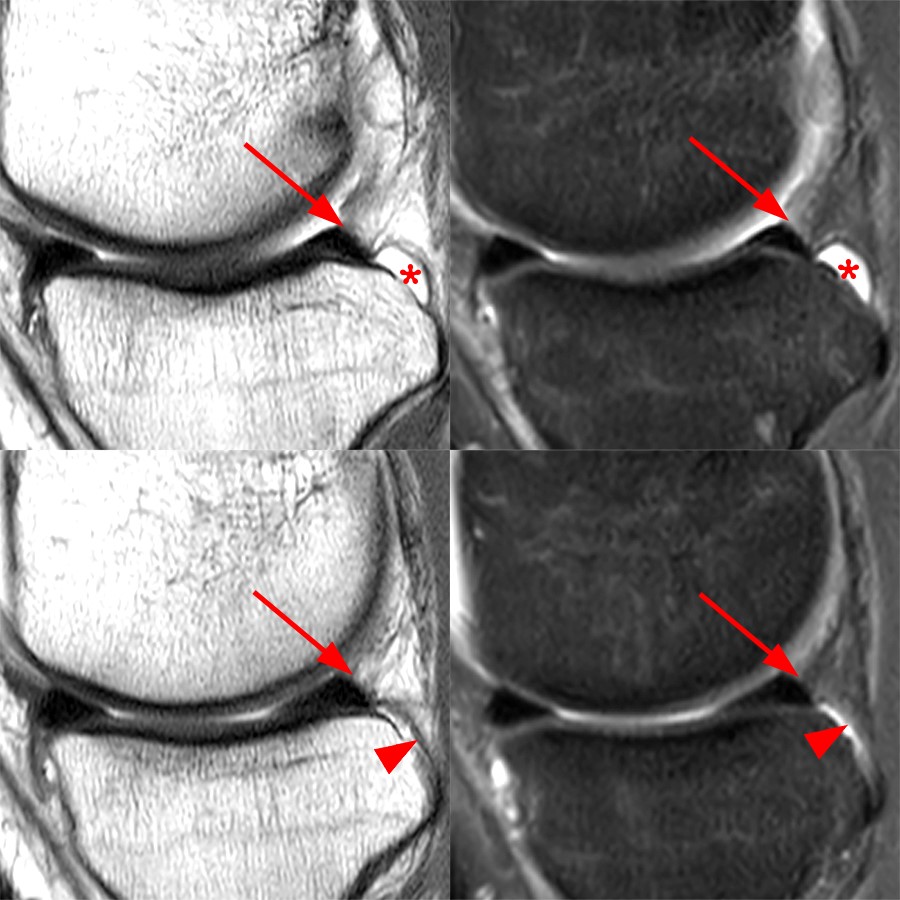
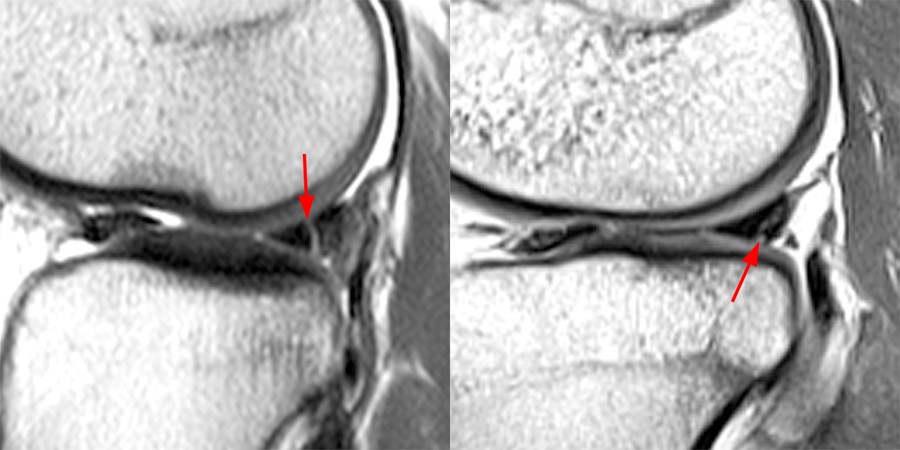
Sagittal proton density-weighted images through the posterior horn of the medial meniscus without (left) and with (right) fat-suppression. Posteriorly the medial meniscus is anchored to the tibia via the posterior root and by the coronary ligament (arrowhead). The posterior horn of the medial meniscus also attaches to the posterior capsule (arrow) via interface with vascularized fibrofatty and synovial soft tissue which typically fat-suppresses as in this case. A smooth recess along the tibial surface of the meniscocapsular junction is a normal finding that can be seen near the posterior root, but becomes flattened by the taut coronary ligament (arrowhead) further medially. Note the suppression of fat-signal at the meniscocapsular junction on the right images.
The lateral meniscus is more circular with a shorter radius of curvature and a more uniform size throughout, such that the anterior and posterior horns are similar in size on sagittal images. The lateral meniscus covers approximately 70% of the lateral tibial plateau. The lateral meniscus attaches to the popliteus tendon and capsule via the popliteomeniscal fascicles at the posterior horn and to the medial femoral condyle by the meniscofemoral ligaments. The anterior meniscofemoral ligament (Humphrey) and posterior meniscofemoral ligament (Wrisberg) are commonly present with one or both found with a reported incidence of 93-100%3,4. The lateral meniscus is also attached to the fibula by the meniscofibular ligament and to the tibia by a coronary ligament.5 The lateral meniscus is more loosely attached than the medial meniscus and can translate approximately 11mm with normal knee motion.6
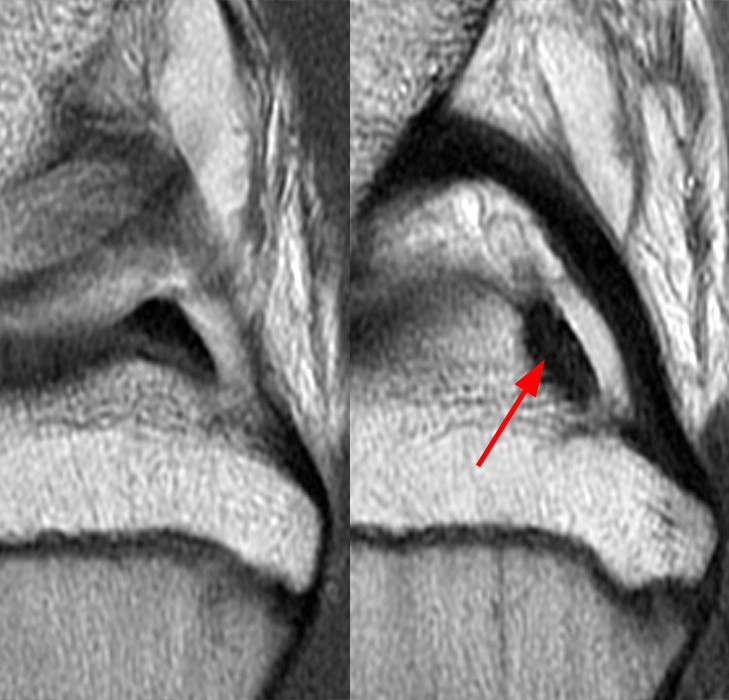
Figure 4:
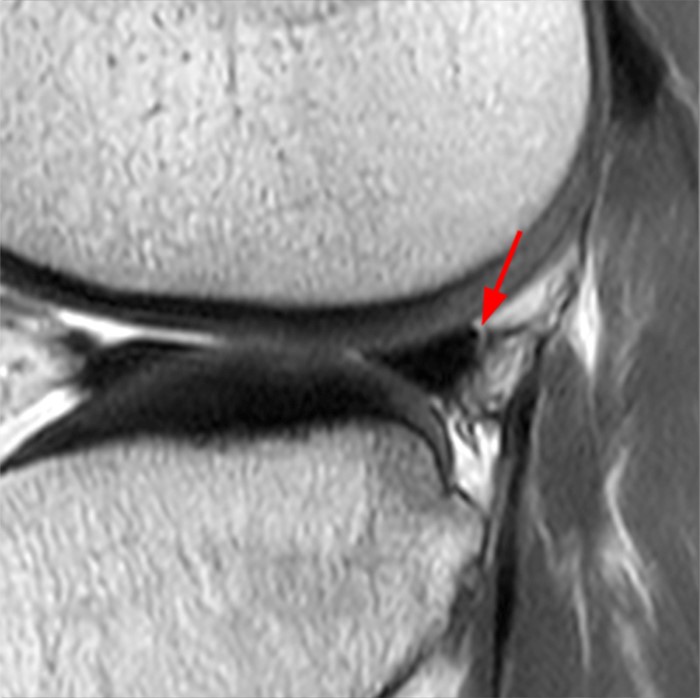
Posteriorly the lateral meniscus is stabilized by the popliteomeniscal fascicles, meniscofemoral ligaments, and the coronary ligaments. On this sagittal proton density-weighted image through the popliteal hiatus, the posterosuperior (long arrow) and anteroinferior (short arrow) popliteomeniscal fascicles attach the posterior horn of the lateral meniscus to the capsule and form a passageway that allows the popliteus tendon (arrowhead) to pass from intra-articular to extra-articular. The posterosuperior fascicle is the most consistently found fascicle. A more detailed review of this anatomy can be found at Hypermobile Lateral Meniscus-February 2015.
Both menisci are firmly attached to the tibia anteriorly and posteriorly by the meniscal root ligaments. Because the anatomy is more complex and injuries are more common, this discussion focuses on the posterior meniscal roots rather than the anterior meniscal roots. The posterior root of the medial meniscus attaches posterior to the apex of the medial tibial spine and anteromedial to the PCL tibial attachment. 7 The posterior root of the lateral meniscus is found posteromedial to the lateral tibial eminence apex and anterolateral to the posterior root of the medial meniscus near the posterior aspect of the ACL footprint.7,8
The posterior meniscal root ligaments are best visualized utilizing a combination of sagittal and coronal images.9 The coronal oblique imaging plane that parallels Blumensaat’s line and is carried through the posterior tibia is also helpful in visualizing the posterior meniscal roots.
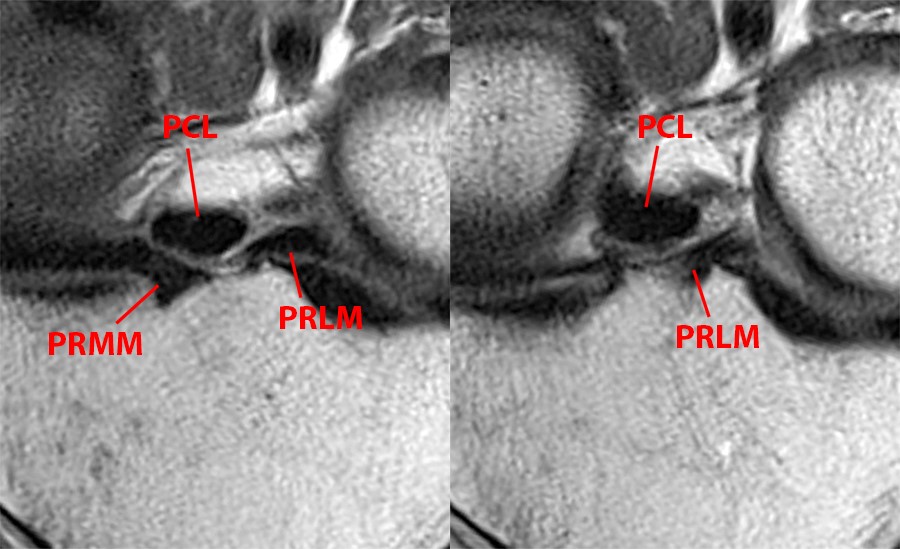
Figure 6:
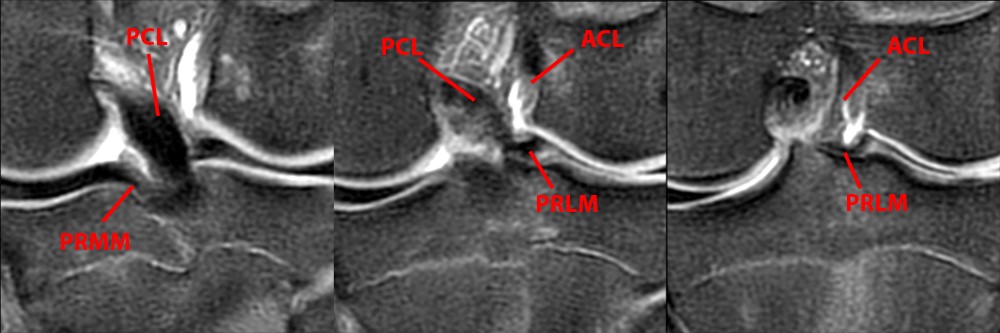
T2-weighted coronal oblique images better detail the root insertions of the medial meniscus (PRMM) and lateral meniscus (PRLM) by imaging the insertions in profile. Note that in this plane, the PCL is foreshortened and the image slice angle is close to perpendicular to the meniscal root footprints.
By MRI the posterior root of the medial meniscus is identified on the sagittal view immediately anterior to the PCL along the posterior slope of the tibial eminence. On coronal and coronal oblique images, the posterior root of the medial meniscus is a band-like structure with a horizontal or slightly angled inferiorly orientation.10
The posterior root of the lateral meniscus is often more difficult to evaluate because of the obliquity and superiorly directed course of the root ligament fibers.10 The posterior root of that lateral meniscus is longer than the posterior root of the medial meniscus. After passing over the lateral tibial spine, the root becomes flattened in appearance at its attachment.10
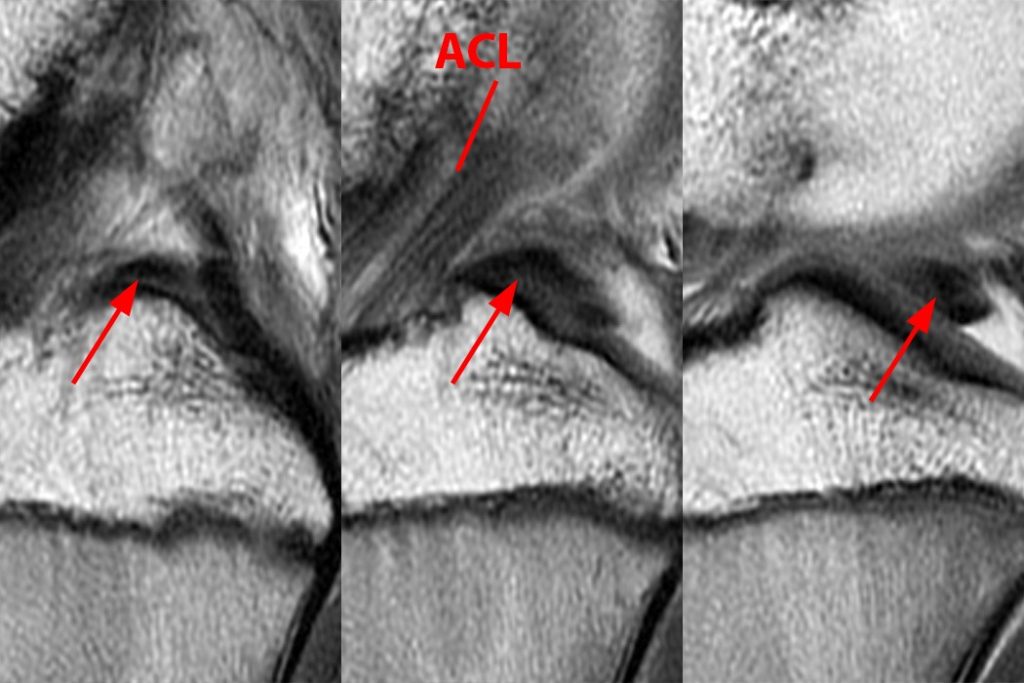
Figure 8:
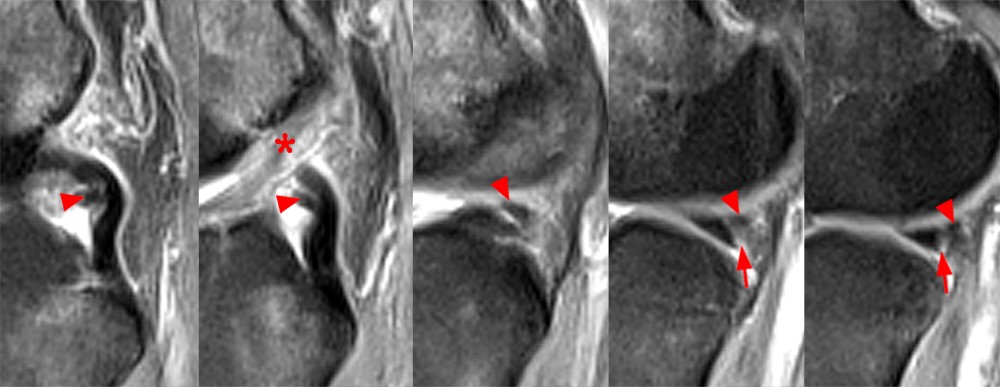
Sagittal proton density-weighted views through the tibial eminence progress from anterior and medial (left) to posterior and lateral (right). The posterior root of the lateral meniscus (arrow) is longer than the posterior root of the medial meniscus. The footprint is found just posterior to the ACL and can be followed in an oblique path posteriorly and laterally to the posterolateral aspect of the tibial eminence.
The main vascular supply to the menisci is from the superior and inferior geniculate arteries with the middle geniculate supplying portions of the anterior and posterior horns.11 The entire menisci are highly vascular in the newborn.1 By the age of 9 months, the inner one-third of the meniscus becomes avascular, and by 10 years of age the vascular supply is similar to an adult with blood supplying the peripheral 10-30% of the meniscus.1 Meniscal tears in the peripheral more vascularized region of the meniscus (red zone) have a better chance of healing in contrast to tears located nearer to the meniscal free edge.
Function
The menisci of the knee have several biomechanical functions, with the most important being load distribution and knee stability. Load transmission is facilitated by the meniscal contour and the meniscal composition. Three distinctly different orientations of collagen fibers are found in the meniscus. Longitudinal, circumferentially oriented fibers are mostly type I collagen and comprise the deep layer of the meniscus.12 This collagen fiber arrangement helps dissipate the downward force on the tibial plateau by converting the axial load into hoop stresses.11,12 The ability to adequately accommodate this hoop stress requires intact anterior and posterior roots in addition to continuity of the circumferential collagen fibers. The lamellar layer has peripheral radially oriented fibers with a mesh like network of collagen fibers that are more loosely organized and serve to tie the longitudinal bundles together and resist longitudinal splitting.12 The superficial layer is composed of randomly oriented collagen fibers mixed with a layer of proteoglycans, which helps to reduce friction with the femoral condyles.12 The contour and fixation points of the menisci assist in conferring knee stability. Because of its firm attachments, the medial meniscus appears to be more important than the lateral meniscus in contributing to anteroposterior stability of the knee, but recent studies also indicate contributions from the lateral meniscus in limiting anterior tibial translation.
MRI Findings
Acute Injury
When an ACL tear occurs, the tibia most commonly translates anteriorly with external rotation relative to the femur. Meniscal tears result from entrapment and rotational forces between the tibia and femur and tensile forces from the attached points with the posterior joint capsular structures and ligaments.13,14 Both the medial and lateral menisci are commonly injured in association with an acute ACL tear. Tears can occur throughout the medial and lateral menisci but are considerably more prevalent within the posterior horns.15 Radial, longitudinal, and complex tear patterns are typically found in the posterior horn of the lateral meniscus. Unfortunately, multiple studies indicate that MRI has the lowest sensitivity for identifying meniscal tears in the posterior horn of the lateral meniscus, which has been attributed to various factors including pulsation artifact from the popliteal artery, volume averaging and magic angle associated with the contour of the tibial eminence and the overlying meniscal tissue, and the anatomy of the meniscofemoral ligament.16,17,18,19,20 A variety of tears may also be seen in the medial meniscus, but a higher percentage tend to be longitudinal tears of the posterior horn.15,21 Detection of longitudinal tears near the meniscocapsular junction at the posterior horn of the medial meniscus can also be difficult to detect with only approximately 50% of meniscocapsular lesions identified by MRI according to some studies.22 Furthermore, detection of tears within the posterior menisci and the meniscal periphery is more difficult in the setting of an acute ACL tear resulting in a higher incidence of false negative studies for meniscal tear.23 Consequently, careful inspection in multiple imaging planes is required to optimize detection of subtle tears.
Posterior Meniscal Root Tears
Posterior root tears of the lateral meniscus occur in 8% – 9.8% of patients with an ACL tear and rarely occur in the absence of an ACL tear.24,9 Although posterior root tears of the lateral meniscus can present as an isolated partial tear or avulsion, they commonly involve the adjacent posterior horn of the lateral meniscus.9,25 Tears of the posterior root can be very subtle occurring at or within a few millimeters of the footprint, and as with other meniscal tears, their detection relies on distortion of the root contour or increased signal intensity in the root that extends to the surface.9,17 Fluid-sensitive series are ideal for demonstrating a fluid-filled cleft interrupting the meniscal root (Figure 9). Avulsion fractures are rare but the avulsed bone is readily visible by MRI (Figure 10).
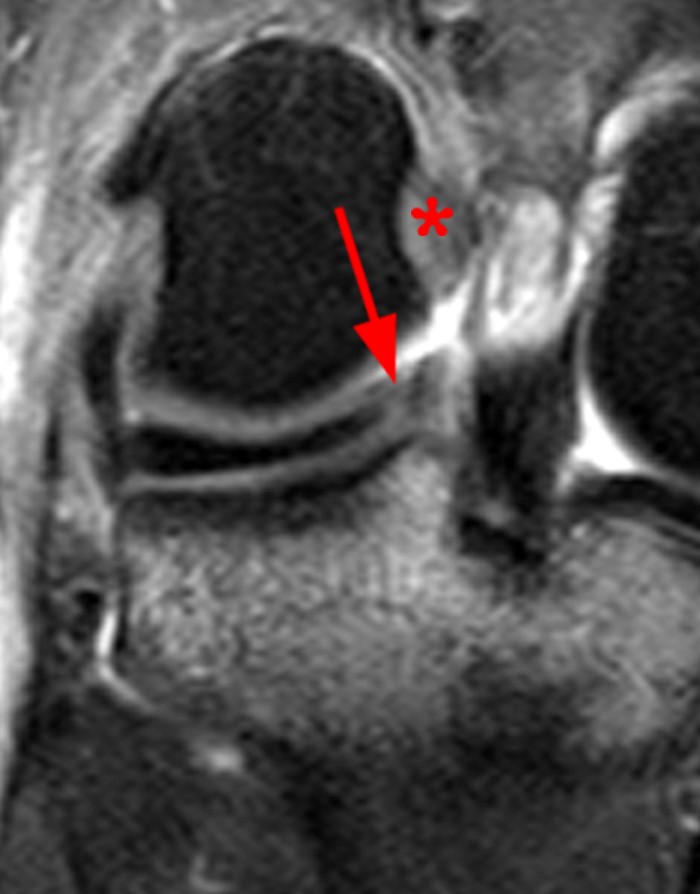
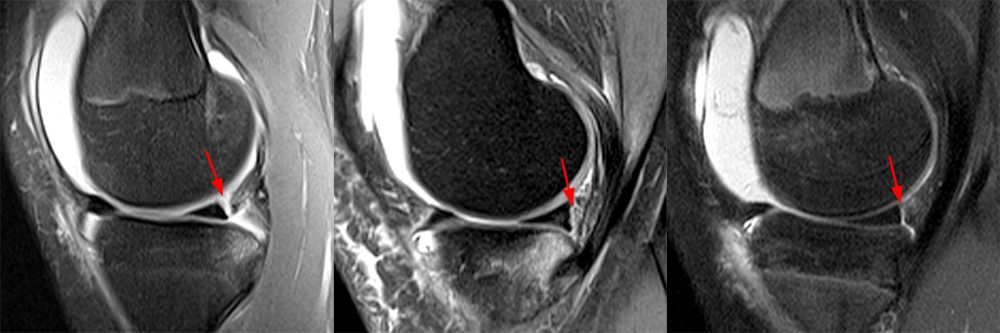
Figure 9:
A 25 year-old male presented after a twisting injury while playing football. A fat-suppressed proton density-weighted coronal (9A) image through the posterior horns of the menisci demonstrates ill-defined irregular thickening and abnormal signal at the junction of the posterior horn of the lateral meniscus and the posterior root overlying the lateral tibial spine (arrow). Edema and distortion of the proximal ACL stump is seen (asterisk). A fat-suppressed proton density-weighted sagittal (9B) image through the lateral aspect of the tibial eminence demonstrates focal interruption of the posterior root of the lateral meniscus by linear fluid signal (arrow), immediately posterior to the distal ACL stump (arrowhead).
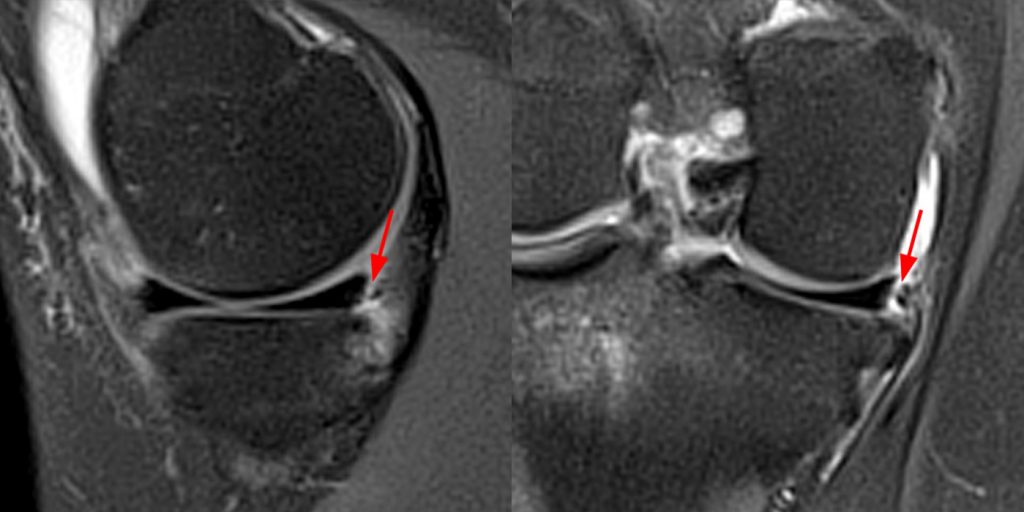
Figure 10:
A 42 year-old male suffered a twisting injury and felt a pop while on a trampoline 6 days prior and presents with instability and locking. Fat-suppressed proton density-weighted coronal (10A) and sagittal (10B) images and a T1-weighted sagittal (10C) image centered on the posterior aspect of the tibial eminence demonstrates distortion of the posterior root of the lateral meniscus (arrowheads) attached to a mildly elevated avulsion fracture at the footprint (arrows). The proximal ACL stump is indicated (small arrow) and multiple bone bruises (asterisks) are present.
A characteristic tear pattern associated with ACL injuries is a parrot-beak tear seen at the free edge of the PHLM just lateral to the tibial eminence. This tear curves medially and can extend into the posterior root of the lateral meniscus with vertical or horizontal elements (Figure 11). Instead of terminating in the posterior root, the parrot beak tear can also continue posteromedially across the posterior horn of the meniscus and root transecting the meniscus This tear typically occurs in proximity to the insertion of the meniscofemoral ligament(s) onto the meniscus, and the intact meniscofemoral ligament helps to stabilize the lateral meniscus and prevent lateral meniscus extrusion. In both instances, an unstable meniscal flap, which remains attached at the posterior root, can be created and can displace in multiple directions (Figure 12).
Figure 11:
A 19 year-old female injured playing soccer. Fat-suppressed proton density-weighted sequential sagittal images (11A) moving from lateral to medial demonstrate a relatively normal posterior horn contour (arrowhead) with progression of the tear from the free edge into the lateral aspect of the meniscal root (arrows). The fat-suppressed proton density-weighted coronal image (11B, left) demonstrates the typical free edge location of the tear (arrow). The fat-suppressed proton density-weighted axial image (11B, right) shows the parrot beak tear of the meniscus en face filled with fluid (arrows).
Posterior root tears of the medial meniscus associated with ACL tears are significantly less frequent than root tears of the lateral meniscus with an incidence of approximately 3%. When present, posterior root tears of the medial meniscus are more frequently associated with extrusion of the medial meniscus.24
Longitudinal Tears
Longitudinal tears run perpendicular to the tibial plateau and parallel the AP contour of the meniscus, dividing the meniscus into central and peripheral portions. These are often associated with significant knee trauma and typically involve the peripheral third of the meniscus.26 There is a close association between ACL tears and peripheral longitudinal tears in the posterior horns of both the medial and lateral menisci.17 Longitudinal, tears at the posterior horn of the lateral meniscus are often more difficult to detect as the tear plane approaches the periphery of the meniscus because of the complex anatomy and posterior attachments of the capsule and popliteomeniscal fascicles, and the lateral meniscus is often interpreted as normal.17 Failure to identify and repair these tears can result in a bucket-handle tear of the lateral meniscus.17 When the tear extends through the meniscal substance it is readily identified against the contrast afforded by the low signal meniscal tissue (Figure 13). Longitudinal tears that occur further peripherally can be more difficult to detect, and identification of an “extra” vertical line or layer in the meniscal periphery can be a subtle finding that indicates a tear (Figure 14). Additional clues to the presence of a lateral meniscal tear include tears of the posterosuperior popliteomeniscal fascicle which have a high association with tears of the posterior horn of the lateral meniscus (Figure 15).27 Even with a high degree of suspicion and careful inspection, a significant number of these type tears found at arthroscopy are not convincingly visualized by MRI.
A subset of the longitudinal tears of the posterior horn of the lateral meniscus, termed the “Wrisberg Rip” originates at the junction of the posterior horn of the lateral meniscus and the meniscofemoral ligament. These tears can originate at the attachment sites of either the ligament of Wrisberg or the ligament of Humphrey (Figure 16). Differentiation of this tear from the normal pseudo-tear is made by lateral extension of the cleft between the meniscus and meniscofemoral ligament by 1.4 cm or more lateral to the lateral margin of the PCL.28,29,30
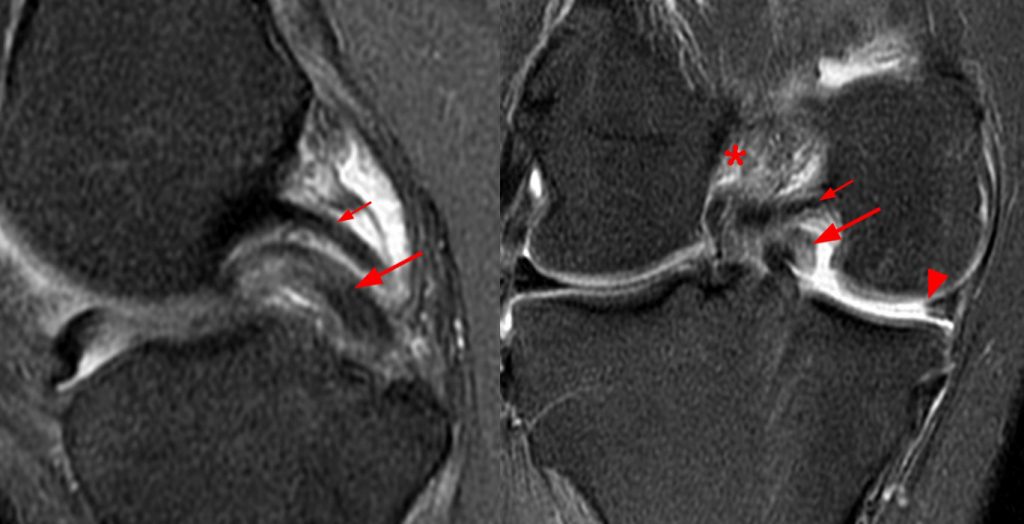
Figure 16:
Fat-suppressed proton density-weighted sequential sagittal images (16A) and reformatted axial oblique image (16B) demonstrate a “Wrisberg Rip” pattern that originates with the ligament of Humphrey. The sagittal images progress from medial to lateral and demonstrate the ligament of Humphrey (arrowheads) passing anterior to the PCL and continuing into the superior margin of the peripheral tear segment created by the longitudinal tear (arrows) of the posterior horn of the lateral meniscus. Axial oblique reformatted image demonstrates the course of the ligament of Humphrey anterior to the PCL (arrowheads) as it joins to the meniscal fragment peripheral to the longitudinal tear (arrows). The abnormally edematous and irregular ACL (asterisk) is seen on the sagittal views.
Longitudinal tears at the far periphery of the posterior horn of the medial meniscus at or near its junction with the posterior capsule are increasingly referred to as “ramp” lesions in the orthopaedic literature, reviving a reference that originated with Strobel.31 There is no clear consensus on the exact anatomic injury associated with this tear, and tears at both the meniscocapsular junction and within the periphery of the meniscus have been included in categories of “ramp lesions”, whereas coronary ligament tears are generally considered separately.32,33 Peripheral longitudinal tears of the medial meniscus are found in up to 19% of acute ACL tears and up to 36% of chronic ACL tears.32,33 Because of the difficulty in evaluating the posteromedial compartment through standard anterior portals, these tears may be missed by the arthroscopist.33 In addition, some of these tears may not extend to the meniscal surface resulting in a hidden tear that requires superficial debridement for visualization.33
While MRI has a high reported sensitivity of >90% for detecting medial meniscal tears, to date, MRI has not proven as successful in diagnosing meniscocapsular separations with reported sensitivity of 48-71%.22,34 The most plausible explanation for the decreased sensitivity is the extended position of the knee during the MRI examination, which reduces meniscocapsular separation. The MRI diagnosis of meniscocapsular separation relies on the presence of increased signal irregularity of the capsule on fluid-sensitive series or a separation at the meniscocapsular junction. Edema and irregularity of the meniscocapsular junction of the posterior horn is the most frequent finding. These changes are best detected on fluid-sensitive, fat-suppressed sequences (Figure 17). A fluid signal cleft at the meniscocapsular junction is most specific for making the diagnosis (Figure 18). Bone bruises of the posterior medial tibia have been cited as a possible indicator of a meniscocapsular tear, however a recently published article concluded that medial tibial contusions are not specific for meniscocapsular or peripheral meniscal tears.22,34
Figure 17:
A 34 year-old male presents following a soccer injury 1 day prior. Fat-suppressed proton density-weighted (left) and T1-weighted (right) sagittal views through the medial meniscus demonstrates edema (arrows) at the meniscocapsular junction which replaces the typical fat signal. Although a discrete fluid-filled cleft is not identified, this appearance is suggestive of a meniscocapsular tear.
Longitudinal tears of the posterior horn or meniscocapsular junction can propagate anteriorly into the meniscal periphery at the posterior junction and body regions (Figure 19).
Figure 19:
Fat-suppressed proton density-weighted sagittal (19A) and coronal (19B) images of an 18 year-old male injured playing football 2 weeks prior to the MRI demonstrates a peripheral longitudinal tear of the meniscus (arrows) with a small peripheral meniscal fragment that continues anteriorly and can be identified at the meniscal periphery on the coronal images.
Meniscal tears in the setting of a chronic ACL Tear
Combined medial and lateral meniscal tears and isolated medial meniscal tears are common with chronic ACL tears (considered to be over 6 weeks after injury), and are felt to be the result of repetitive microtrauma associated with joint laxity.15 Tears of the medial meniscus in the setting of a chronic ACL tear are most often seen in the posterior junction followed by the posterior horn region.15 Bucket-handle tears are more frequently encountered in the setting of a chronic ACL tear and most commonly affect the medial meniscus15 (Figure 20). Chronic peripheral longitudinal tears are frequently easier to identify by a well-defined fluid containing cleft without surrounding edema that frequently accompanies acute injuries. Healed peripheral longitudinal tears are often evident as residual distortion of the peripheral meniscocapsular junction and irregular low signal that presumably represents scar with no fluid containing defect. Untreated meniscal root tears can result in extrusion of the meniscal body and are most commonly seen in the medial meniscus.
Figure 20:
A 25 year-old male complains of a twisting injury followed by locking. Fat-suppressed proton density-weighted sagittal (left) and coronal (right) images demonstrate the classic finding of a “double PCL” sign resulting from lateral displacement of a medial meniscal bucket handle fragment (large arrows) that lies anterior and inferior to the PCL (small arrows). On the coronal image, the peripheral, nondisplaced meniscal body remnant demonstrates a blunted inner margin (arrowhead).
Functional Implications
Root tears
Posterior root tears of the medial meniscus are clearly linked to an accelerated progression of arthritis associated with meniscal destabilization, extrusion, and altered tibiofemoral biomechanics.35 Posterior root repair is becoming increasingly recognized as necessary to restore the normal function of the meniscus and help prevent the progression of osteoarthritis.
The consequences of untreated posterior root tears of the lateral meniscus are less well understood and continue to evolve. One study indicated no significant difference between the study and control groups for most objective and subjective outcomes at 10 years after surgery.36 A second study reported successful clinical outcomes with considerable healing and functional restoration on MRI and second-look arthroscopy at 3 years for stable posterior horn tears of the lateral meniscus, including posterior root tears.37 Extrusion of the lateral meniscus in association with a posterior root tear is much less common compared to posterior root tears of the medial meniscus.38,25 The meniscofemoral ligaments, which are generally present, appear to help maintain stability of the lateral meniscus, presumably by contributing tensile properties to the circumferential strength of the lateral meniscus, thus preventing meniscal extrusion.25,38,24 In addition, intact meniscofemoral ligaments help protect the lateral compartment from increased contact pressure in the setting of a posterior root tear of the lateral meniscus.39 Recent anatomic studies stress the importance of the posterior root of the lateral meniscus as a stabilizer of the knee against internal rotation and anterior tibial translation even with an intact meniscofemoral ligament, suggesting that failure to repair a posterior root tear of the lateral meniscus may contribute to ACL reconstruction graft failure.40,41
Longitudinal Tears
Cadaveric studies have demonstrated the importance of the posteromedial meniscocapsular junction in preventing anterior translation and external rotation of the tibia and suggested the importance of repairing the posteromedial meniscocapsular junction at the time of ACL repair.42,43 Failure to address an unstable tear of the posteromedial meniscocapsular junction can result in persistent tibiofemoral and meniscal laxity even after successful ACL reconstruction.44,42,43 This leads to increased strain on the ACL reconstruction and can contribute to eventual ACL graft failure. Extension of an untreated or undiagnosed peripheral tear can result in further meniscal injury and instability and eventually lead to accelerated osteoarthritis.
Within the lateral meniscus, untreated longitudinal peripheral tears may become increasingly unstable leading to displacement and a bucket-handle tear or symptoms associated with a hypermobile lateral meniscus 17,45
Treatment
For root tear reattachment, transtibial pull-out repair is most commonly used, utilizing a transtibial bone tunnel to allow passage of sutures from the meniscal root to a surgical button on the anterior aspect of the tibia. Suture anchor techniques are less commonly used and may be more technically challenging. Suture repair can be used with healthy meniscal tissue on either side of the tear. Small, stable tears are treated with debridement without repair.25
Peripheral longitudinal meniscal or meniscocapsular junction tears are generally repaired by all inside or inside-out methods when identified. Tears of the meniscocapsular junction are more likely to heal spontaneously because of the more robust blood supply, whereas tears within the meniscal substance or with greater than a 2 mm gap are less likely to do so.46 Peripheral tears can show evidence of healing with longer times to surgery and obviate surgical repair.
Conclusion
A wide variety of meniscal tears can be encountered in the setting of ACL disruption, but several specific meniscal tear patterns are common. Failure to recognize and repair these injuries may adversely affect the success of ACL reconstruction surgery and can hasten the progression of osteoarthritis, and the current orthopaedic surgical trend is to repair meniscal tears associated with an ACL tear when possible. Peripheral longitudinal tears of the posterior horns of the menisci and tears involving the posterior root of the lateral meniscus are strongly associated with an ACL injury. An understanding of the location and appearance of these meniscal tears can help to improve detection of these often subtle and easily missed abnormalities.
References
- Clark CR, Ogden JA. Development of the Menisci of the Human Knee Joint MORPHOLOGICAL CHANGES AND THEIR POTENTIAL ROLE IN CHILDHOOD MENISCAL INJURYY. JBJS. 1983;65-A(4):538-547. ↩
- Greis PE, Bardana DD, Holmstrom MC, Burks RT. Meniscal injury: I. Basic science and evaluation. J Am Acad Orthop Surg. 2002. doi:10.5435/00124635-200205000-00003 ↩
- Cho JM, Suh JS, Na JB, et al. Variations in meniscofemoral ligaments at anatomical study and MR imaging. Skeletal Radiol. 1999;28(4):189-195. doi:10.1007/s002560050499 ↩
- Nagasaki S, Ohkoshi Y, Yamamoto K, Ebata W, Imabuchi R, Nishiike J. The Incidence and Cross-sectional Area of the Meniscofemoral Ligament. Am J Sports Med. 2006;34(8):1345-1350. doi:10.1177/0363546506287825 ↩
- Bozkurt M, Elhan A, Tekdemir I, Tonuk E. An anatomical study of the meniscofibular ligament. Knee Surgery, Sport Traumatol Arthrosc. 2004;12(5):429-433. doi:10.1007/s00167-003-0450-z ↩
- Thompson WO, Thaete FL, Fu FH, Dye SF. Tibial meniscal dynamics using three-dimensional reconstruction of magnetic resonance images. Am J Sports Med. 1991;19(3):210-216. doi:10.1177/036354659101900302. ↩
- Johannsen AM, Civitarese DM, Padalecki JR, Goldsmith MT, Wijdicks CA, LaPrade RF. Qualitative and Quantitative Anatomic Analysis of the Posterior Root Attachments of the Medial and Lateral Menisci. Am J Sports Med. 2012;40(10):2342-2347. doi:10.1177/0363546512457642 ↩
- Johnson DL, Swenson TM, Livesay GA, Aizawa H, Fu FH, Harner CD. Insertion-Site Anatomy of the Human Menisci: Gross, Arthroscopic, and Topographical Anatomy as a Basis for Meniscal Transplantation. Arthrosc – J Arthrosc Relat Surg. 1995;11(4):386-394. http://www.arthroscopyjournal.org/article/0749-8063(95)90188-4/pdf. Accessed February 11, 2018. ↩
- De Smet AA, Blankenbaker DG, Kijowski R, Graf BK, Shinki K, Smet DA. MR Diagnosis of Posterior Root Tears of the Lateral Meniscus Using Arthroscopy as the Reference Standard. AJR. 2009;192:480-486. doi:10.2214/AJR.08.1300 ↩
- De Smet AA. How I diagnose meniscal tears on knee MRI. AJR Am J Roentgenol. 2012. doi:10.2214/AJR.12.8663 ↩
- Kelly JD. Meniscal injuries: Management and surgical techniques. Meniscal Inj Manag Surg Tech. 2013:1-129. doi:10.1007/978-1-4614-8486-8 ↩
- Petersen W, Tillmann B. Collagenous fibril texture of the human knee joint menisci. Anat Embryol (Berl). 1998;197(4):317-324. doi:10.1007/s004290050141 ↩
- MacMahon PJ, Palmer WE. A Biomechanical Approach to MRI of Acute Knee Injuries. Am J Roentgenol. 2011;197(3):568-577. doi:10.2214/AJR.11.7026 ↩
- Hayes CW, Brigido MK, Jamadar DA, Propeck T. Mechanism-based Pattern Approach to Classification of Complex Injuries of the Knee Depicted at MR Imaging. RadioGraphics. 2000;20(suppl_1):S121-S134. doi:10.1148/radiographics.20.suppl_1.g00oc21s121 ↩
- Hagino T, Ochiai S, Senga S, et al. Meniscal tears associated with anterior cruciate ligament injury. Arch Orthop Trauma Surg. 2015;135(12):1701-1706. doi:10.1007/s00402-015-2309-4 ↩
- DeSmet AA, Graf BK. Meniscal Tears Missed on MR Imaging: Relationship to Meniscal Tear. AJR. 1994;162(4):905-911. doi:162.4.8141016 ↩
- De Smet AA, Mukherjee R. Clinical, MRI, and Arthroscopic Findings Associated with Failure to Diagnose a Lateral Meniscal Tear on Knee MRI. Am J Roentgenol. 2008;190(1):22-26. doi:10.2214/AJR.07.2611 ↩
- Justice WW, Quinn SF. Error Patterns in the MR Imaging Evaluation of Menisci of the Knee. Radiology. 1995;196:617-621. ↩
- Quinn SF, Brown TF. Meniscal Tears Diagnosed with MR Imaging versus Arthroscopy: How Reliable a Standard Is Arthroscopy. Radiology. 1991;181(12):842-847. http://pubs.rsna.org/doi/pdf/10.1148/radiology.181.3.1947108. Accessed February 2, 2018. ↩
- De Smet AA, Tuite MJ, Norris MA, Swan JS. MR Diagnosis of Meniscal Tears: Analysis of Causes of Errors. AJR. 1994;163:1419-1423. https://www.ajronline.org/doi/pdf/10.2214/ajr.163.6.7992739. Accessed February 2, 2018. ↩
- Boxheimer L, Lutz AM, Zanetti M, et al. Characteristics of displaceable and nondisplaceable meniscal tears at kinematic MR imaging of the knee. Radiology. 2006;238(1):221-231. doi:10.1148/radiol.2381041234 ↩
- DePhillipo NN, Cinque ME, Chahla J, Geeslin AG, Engebretsen L, LaPrade RF. Incidence and Detection of Meniscal Ramp Lesions on Magnetic Resonance Imaging in Patients With Anterior Cruciate Ligament Reconstruction. Am J Sports Med. 2017;45(10):2233-2237. doi:10.1177/0363546517704426 ↩
- Ahn JH, Jeong SH, Kang HW. Risk Factors of False-Negative Magnetic Resonance Imaging Diagnosis for Meniscal Tear Associated With Anterior Cruciate Ligament Tear. Arthrosc J Arthrosc Relat Surg. 2016;32(6):1147-1154. doi:10.1016/j.arthro.2015.11.046 ↩
- Brody JM, Lin HM, Hulstyn MJ, Tung GA. Lateral Meniscus Root Tear and Meniscus Extrusion with Anterior Cruciate Ligament Tear. Radiology. 2006;239(3):805-810. doi:10.1148/radiol.2393050559 ↩
- LaPrade CM, James EW, Cram TR, Feagin JA, Engebretsen L, LaPrade RF. Meniscal Root Tears. Am J Sports Med. 2015;43(2):363-369. doi:10.1177/0363546514559684 ↩
- Nguyen JC, De Smet AA, Graf BK, Rosas HG. MR Imaging–based Diagnosis and Classification of Meniscal Tears. RadioGraphics. 2014;34(4):981-999. doi:10.1148/rg.344125202 ↩
- Rosas HG, De Smet A a. Magnetic Resonance Imaging of the Meniscus. Magn Reson Imaging Clin N Am. 2014;22(4):493-516. doi:10.1097/RMR.0b013e3181d657d1 ↩
- Vahey TN, Bennett HT, Arrington LE, Shelboume KD, Ng J. MR Imaging of the Knee: Pseudotear of the Lateral Meniscus Caused by the Meniscofemoral Ligament MR images of the knee often show a linear band of increased signal in the. AJR. 1990;154(6):1237-1239. https://www.ajronline.org/doi/pdf/10.2214/ajr.154.6.2110735. Accessed February 3, 2018. ↩
- Park LS, Jacobson JA, Jamadar DA, Caoili E, Kalume-Brigido M, Wojtys E. Posterior horn lateral meniscal tears simulating meniscofemoral ligament attachment in the setting of ACL tear: MRI findings. Skeletal Radiol. 2007;36(5):399-403. doi:10.1007/s00256-006-0257-3 ↩
- Mohankumar R, White LM, Naraghi A, Naraghi A. Pitfalls and Pearls in MRI of the Knee. AJR. 2014;20314:516-530. doi:10.2214/AJR.14.12969 ↩
- Strobel M. Menisci. In: Fett HM, Flechtner P, eds. Manual of arthroscopic surgery. New York: Springer, 1988;171-178. ↩
- Liu X, Feng H, Zhang H, Hong L, Wang XS, Zhang J. Arthroscopic Prevalence of Ramp Lesion in 868 Patients With Anterior Cruciate Ligament Injury. Am J Sports Med. 2011;39(4):832-837. doi:10.1177/0363546510388933 ↩
- Sonnery-Cottet B, Conteduca J, Thaunat M, Gunepin FX, Seil R. Hidden Lesions of the Posterior Horn of the Medial Meniscus. Am J Sports Med. 2014;42(4):921-926. doi:10.1177/0363546514522394 ↩
- Hatayama K, Terauchi M, Saito K, Aoki J, Nonaka S, Higuchi H. Magnetic Resonance Imaging Diagnosis of Medial Meniscal Ramp Lesions in Patients With Anterior Cruciate Ligament Injuries. Arthrosc J Arthrosc Relat Surg. 2018:1-7. doi:10.1016/j.arthro.2017.12.022 ↩
- Allaire R, Muriuki M, Gilbertson L, Harner CD. Biomechanical Consequences of a Tear of the Posterior Root of the Medial Meniscus. J Bone Jt Surgery-American Vol. 2008;90(9):1922-1931. doi:10.2106/JBJS.G.00748 ↩
- Shelbourne KD, Roberson TA, Gray T. Long-term Evaluation of Posterior Lateral Meniscus Root Tears Left In Situ at the Time of Anterior Cruciate Ligament Reconstruction. Am J Sports Med. 2011;39(7):1439-1443. doi:10.1177/0363546511398212 ↩
- Lee DW, Jang HW, Lee SR, Park JH, Ha JK, Kim JG. Clinical, Radiological, and Morphological Evaluations of Posterior Horn Tears of the Lateral Meniscus Left In Situ During Anterior Cruciate Ligament Reconstruction. Am J Sports Med. 2014;42(2):327-335. doi:10.1177/0363546513508374 ↩
- Pula DA, Femia RE, Marzo JM, Bisson LJ. Are Root Avulsions of the Lateral Meniscus Associated With Extrusion at the Time of Acute Anterior Cruciate Ligament Injury? Am J Sports Med. 2014;42(1):173-176. doi:10.1177/0363546513506551 ↩
- Geeslin AG, Civitarese DM, Turnbull TL, Dornan G, Fuso F, LaPrade RF. Biomechanical Consequences of Lateral Meniscal Posterior Root Avulsions. Orthop J Sport Med. 2015;3(7_suppl2):1-2. doi:10.1177/2325967115S00111 ↩
- Frank JM, Moatshe G, Brady AW, et al. Lateral Meniscus Posterior Root and Meniscofemoral Ligaments as Stabilizing Structures in the ACL-Deficient Knee: A Biomechanical Study. Orthop J Sport Med. 2017;5(6):232596711769575. doi:10.1177/2325967117695756 ↩
- Moatshe G, Frank JM, Dornan G, Brady A, Slette E, LaPrade RF. The LM Posterior Root Stabilizes the ACL Deficient Knee. Orthop J Sport Med. 2017;5(7_suppl6):1-2. doi:10.1177/2325967117S00349 ↩
- Peltier A, Lording T, Maubisson L, Ballis R, Neyret P, Lustig S. The role of the meniscotibial ligament in posteromedial rotational knee stability. Knee Surgery, Sport Traumatol Arthrosc. 2015;23(10):2967-2973. doi:10.1007/s00167-015-3751-0 ↩
- Stephen JM, Halewood C, Kittl C, Bollen SR, Williams A, Amis AA. Posteromedial Meniscocapsular Lesions Increase Tibiofemoral Joint Laxity with Anterior Cruciate Ligament Deficiency, and Their Repair Reduces Laxity. Am J Sports Med. 2016;44(2):400-408. doi:10.1177/0363546515617454 ↩
- Papageorgiou CD, Gil JE, Kanamori A, Fenwick JA, Woo S-Y, Fu FH. The Biomechanical Interdependence Between the Anterior Cruciate Ligament Replacement Graft and the Medial Meniscus*. Am J Sports Med. 2001;29(2):226-231. http://journals.sagepub.com/doi/pdf/10.1177/03635465010290021801. Accessed February 11, 2018. ↩
- Makdissi M, Eriksson KO, Morris HG, Young DA. MRI-negative bucket-handle tears of the lateral meniscus in athletes: a case series. Knee Surgery, Sport Traumatol Arthrosc. 2006;14(10):1012-1016. doi:10.1007/s00167-005-0011-8 ↩
- Kijowski R, Rosas HG, Lee KS, Cheung A, Munoz del Rio A, Graf BK. MRI Characteristics of Healed and Unhealed Peripheral Vertical Meniscal Tears. Am J Roentgenol. 2014;202(3):585-592. doi:10.2214/AJR.13.11496 ↩