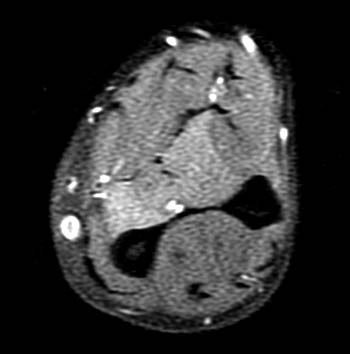
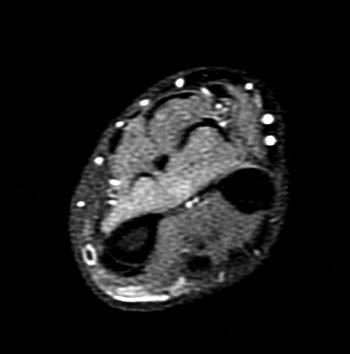
Clinical history: A 53 year-old male presents with a 3 week history of forearm pain and acute onset of loss of thumb flexion. Fat-suppressed proton density-weighted axials images through the distal forearm (1a) and (1b) are presented for interpretation. What are the findings? What is your diagnosis?
Findings
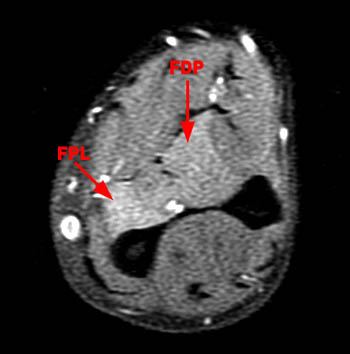
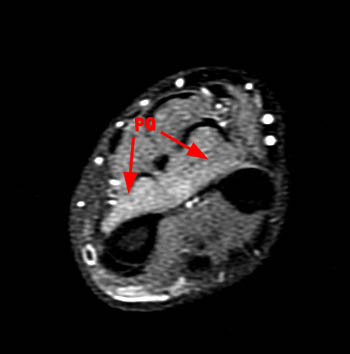
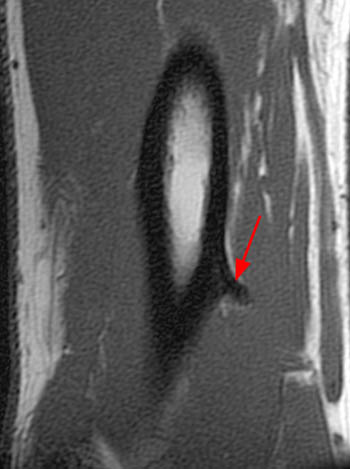
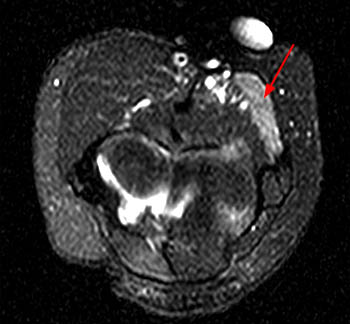
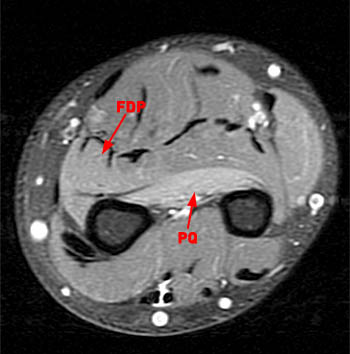
Figure 2:
Axial fat-suppressed image (2a) demonstrates abnormal increased signal in the flexor pollicis longus (FPL) and within the radial half of the flexor digitorum profundus (FDP). Image (2b) demonstrates edema of the pronator quadratus muscle (PQ). These muscles are innervated by the anterior interosseous nerve.
Diagnosis
Complete anterior interosseous nerve syndrome
Discussion
Carpal tunnel syndrome, a disorder of the median nerve at the wrist, is the most common entrapment neuropathy of the upper extremity. Though less common, entrapment of the median nerve can occur more proximally and can be equally debilitating. The median nerve and its branches are susceptible to compression in the elbow and forearm, leading to characteristic patterns of motor and sensory deficits. The clinical presentations of these entrapment syndromes frequently overlap, and electrodiagnostic tests are often inconclusive . MRI can assist in the evaluation of these patients by identifying pathological lesions and anatomical variants causing nerve compression. In cases where no cause of nerve entrapment is readily identifiable, MRI can focus the clinical search by demonstrating patterns of denervation that point to the injured nerve.
Anatomy
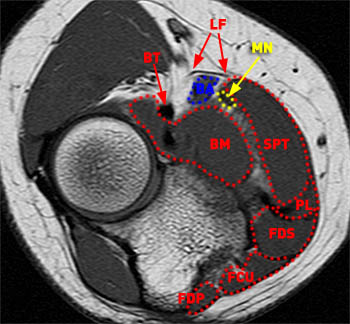
The median nerve arises from the medial (C8 and T1 nerve roots) and lateral (C5-C7 nerve roots) cords of the brachial plexus and extends down the arm medial to the biceps and brachialis muscles and anterior to the brachial artery. The median nerve has no branches in the upper arm. At the elbow, the median nerve lies deep to the lacertus fibrosus and courses deep to the pronator teres muscle and medial to the brachialis muscle, just lateral to the brachial artery and biceps tendon (3a). The median nerve enters the forearm between the superficial (humeral) and the deep (ulnar) heads of the pronator teres muscle, accompanying the ulnar artery (4a). In approximately 22% of individuals the deep head of the pronator teres is absent2. The median nerve then passes deep to the fibrous arch formed by the two heads of the flexor digitorum supericialis. As it continues distally it lies between the flexor digitorum superficialis and flexor digitorum profundus muscles (5a). Approximately 5 cm proximal to the flexor retinaculum, it emerges from behind the lateral edge of the flexor digitorum superficialis, moving to a more superficial position (6a). Motor branches of the median nerve innervate the pronator teres, the flexor carpi radialis, the palmaris longus, and the flexor digitorum superficialis. Branches to the palmaris longus, flexor carpi radialis, and flexor digitorum superficialis arise from the median nerve before it passes through the pronator teres muscle3. It also supplies branches to proximal portions of the flexor pollicis longus and flexor digitorum profundus4.
Figure 3:
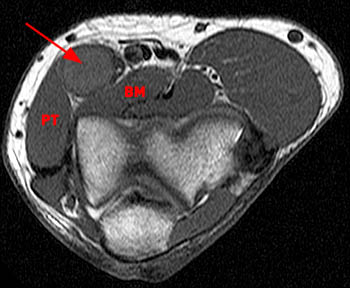
Axial T1-weighted image at the elbow demonstrates the median nerve (MN) between the superficial head of the pronator teres (SPT) and the brachialis muscle (BM) just medial to the brachial artery and vein (BA). The close proximity of the lacertus fibrosus (LF) to the median nerve at this level is demonstrated. The biceps tendon (BT), palmaris longus (PL), flexor digitorum superficialis (FDS), flexor carpi ulnaris (FCU), flexor digitorum profundus (FDP) muscles are also indicated.
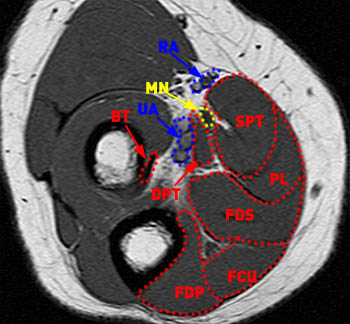
Figure 4:
Axial T1-weighted image just distal to (Figure 3a) demonstrates the median nerve (MN) entering the forearm by passing between the superficial head of the pronator teres (SPT) and the deep head of the pronator teres (DPT). The radial (RA) and ulnar (UA) arteries and veins are demonstrated. The biceps tendon (BT), palmaris longus (PL), flexor digitorum superficialis (FDS), flexor carpi ulnaris (FCU), flexor digitorum profundus (FDP) muscles are also indicated.
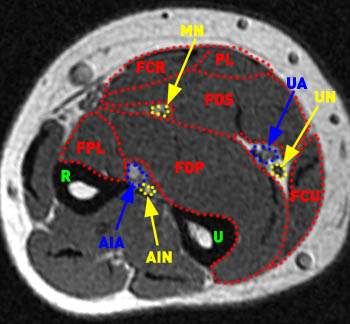
Figure 5:
In the mid forearm the anterior interosseous nerve (AIN) is identified deep to the flexor digitorum profundus (FDP) and flexor pollicis longus (FPL) muscles anterior to the interosseous membrane accompanying the anterior interosseous artery and vein (AIA). The median nerve continues distally between the flexor digitorum profundus (FDP) and flexor digitorum superficialis (FDS) muscles. The flexor carpi radialis (FCR), palmaris longus (PL), and flexor carpi ulnaris (FCU) muscles, the ulnar nerve (UN) and ulnar artery and vein (UA), and the radius (R) and ulna (U) are indicated.
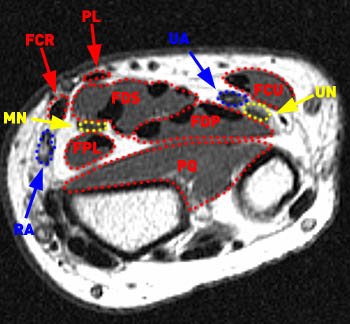
Figure 6:
At the distal forearm the median nerve (MN) moves to the lateral edge of the flexor digitorum superficialis (FDS) eventually becoming more superficial in location as it progresses distal to this level into the wrist. The flexor carpi radialis (FCR) and palmaris longus (PL) tendons, the flexor pollicis longus, flexor digitorum profundus, flexor carpi ulnaris, and pronator quadratus muscles, the ulnar nerve (UN), and the radial (RA) and ulnar (UA) arteries and veins are indicated.
The anterior interosseous nerve (AIN) is the major branch off the median nerve in the forearm, arising 5 to 8 cm distal to the lateral epicondyle near the inferior margin of the pronator teres. Proximal to this level the nerve fibers that become the AIN are a distinct fascicle within the posterior aspect of the median nerve, which may be observed on gross examination but not MRI5. Like the median nerve, the AIN continues deep to the flexor fibrous arch of the digitorum superficialis before continuing distally into the forearm anterior to the interosseous membrane and deep to the flexor digitorum profundus and flexor pollicis longus muscles (E). The AIN is a motor branch to the deep ventral muscles of the forearm, innervating the flexor pollicis longus, the radial half of the flexor digitorum profundus and the pronator quadratus muscles.
Distally within the forearm, the palmar cutaneous nerve arises from the radiopalmar aspect of the median nerve approximately 5 cm proximal to the flexor retinaculum, travels between the palmaris longus and the flexor carpi radialis tendons and remains superficial to the carpal tunnel6. The palmar cutaneous nerve supplies sensation to the radial aspect of the palm and thenar eminence. At the wrist, the median nerve passes through the carpal tunnel to provide motor supply to the thenar eminence muscles (opponens pollicis, abductor pollicis brevis, and flexor pollicis brevis muscles) and the first and second lumbricals. Terminal sensory braches supply the volar surface of the lateral 3 1/2 digits.
Variations in innervation are common in the upper extremity. The most frequently encountered variation is the Martin-Gruber anastomosis, which is reportedly seen in up to 50% of the population7. In this variant, one or two branches from the median nerve or AIN anastomose with the ulnar nerve. This variant alters innervation patterns within the forearm, wrist and hand with some or all of the ulnar-supplied muscles receiving contribution from the median nerve branches. In the hand, the first dorsal interosseous, adductor pollicis, and abductor digiti minimi most commonly receive anomalous innervation from the median nerve or AIN. In addition branches arising from the median nerve, its muscular branches, and the AIN may innervate the ulnar half of the flexor digitorum profundus and flexor digitorum superficialis muscles. When present the Martin-Gruber anastomosis may confound the clinical examination and may limit the accuracy of electromyographic studies8.
Entrapment neuropathies occur because of anatomic constraints at specific locations. The nerve is most vulnerable to entrapment where it passes through a narrow anatomic space, such as a fibro-osseous tunnel or at the site of muscle penetration. These normally occurring points of narrowing can be further narrowed by repetitive stresses, anatomic variants, or degenerative change resulting in compression of the nerve. Additionally, compression and neurologic symptoms may occur because of masses or abnormal collections intrinsic or extrinsic to the nerve.
MRI evaluation
In general, axial images are the most useful for evaluating the nerves and muscles of the upper extremity. T1-weighted axial images readily identify muscles, nerves, and vessels as they traverse the upper extremity because of the fat which often surrounds and highlights these structures. Water-sensitive sequences such as fat-suppressed T2-weighted FSE, fat-suppressed proton density-weighted FSE, and STIR images are valuable in assessing the nerve for edema or masses. The normal nerve is only slightly hyperintense in these sequences. Nerve compression may result in a decreased caliber of the nerve at the level of compression. Increased caliber and edema of the nerve proximal or distal to the site of compression may also be seen. Normal nerves do not appear to enhance with intravenous gadolinium-based contrast agents. Tumors that are intrinsic or extrinsic to the nerve, hematoma, abnormal fluid collections, and fractures are all well depicted by MRI.
Frequently, alterations in the nerve morphology are absent on MRI, and neuropathy is reflected by the effects of denervation on the end-organ. Entrapment of a sensory nerve branch results in dysesthesias along the sensory distribution, and entrapment of motor nerves often leads to muscle signal changes in the innervated muscles. In the mildest form of nerve injury (neuropraxia), damage of the myelin sheath is sustained without associated axonal injury. In this case denervation changes in muscle may be absent. Axonotmesis is a more severe injury in which there is axonal disruption without damage to the surrounding Schwann cells, resulting in Wallerian degeneration. Axonal regeneration is possible. Neurotmesis is the most severe injury indicating disruption of the axons and surrounding myelin and connective tissue9. With axonotmesis and neurotmesis, the supplied muscle demonstrates a predictable sequence of muscle signal abnormalities. In the acute and subacute stage, edema is present within the muscle characterized by increased signal on water-sensitive MRI sequences and may be seen as early as 24-48 hours after denervation10,11. By contrast, electromyographic evidence of denervation may be delayed 2-3 weeks after the nerve injury. The presence of increased intramuscular signal is non-specific, found also with myositis, trauma, and muscle infarction. In general, the muscle signals changes of denervation are most commonly diffuse without associated fascial or perimuscular edema. With long-standing complete denervation, muscle is replaced by fat, leading to increased signal on T1-weighted images.
Figure 7:
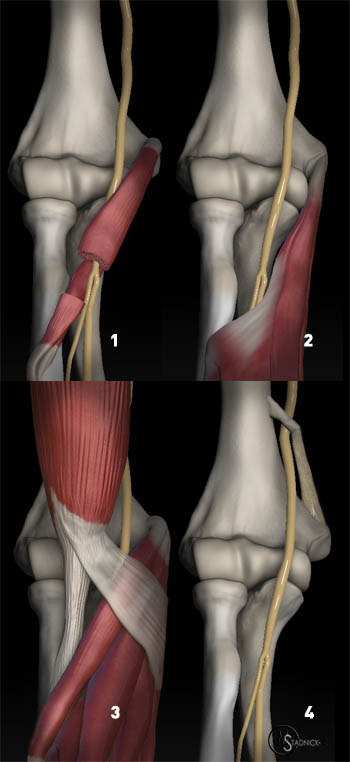
Entrapment at the pronator teres (1) and at the fibrous arch of the flexor digitorum superficialis are the most common causes of entrapment of the median nerve and anterior interosseous nerve at the elbow. Entrapment by the lacertus fibrosus (3) and by the supracondylar process and ligament of Struthers (4) represent less common causes of median nerve entrapment near the elbow.
Proximal to the carpal tunnel, the median nerve and its branches may be compressed at the distal humerus, elbow, or forearm (7a). In general, three clinical syndromes may result depending on the level of entrapment: the supracondylar process syndrome, the pronator syndrome, and the anterior interosseous nerve syndrome.
Supracondylar process syndrome: The median nerve is susceptible to entrapment at the distal humerus in the presence of a fibrosseous tunnel formed by the humerus and the ligament of Struthers. The ligament of Struthers most often arises from a supracondylar process, a bony projection at the anteromedial aspect of the distal humerus approximately 5 cm proximal to the medial epicondyle (8a,8b). The supracondylar process is an anatomic variant seen in approximately 3% of the population and may be bilateral. It is a homologue of a similar bony projection seen in many amphibians, reptiles, and mammals. The ligament of Struthers is thought to be a vestige of the tendon of the latissimo-condyloideus muscle, found in some climbing animals12. In these patients the ligament of Struthers arises from the supracondylar process and attaches to the medial epicondyle, creating a fibrosseous tunnel through which the median nerve passes with or without the brachial artery. This anatomic variation is most commonly asymptomatic and is often found incidentally on plain films. When large enough, the supracondylar process may be palpable. Very rarely, the median nerve may be compressed at this level resulting in paresthesias and numbness of the affected hand. Weakness and atrophy may occur in long-standing cases. With entrapment of the brachial artery, ischemic pain of the forearm and embolization of the distal arteries may occur. Many patients become symptomatic only after a fracture of the process and will experience local pain with palpation of the distal humerus. Several variants have been associated with the supracondylar process and ligament of Struthers that are clinically important in the surgical management of suspected median nerve compression at this level. These include a high origin of the pronator teres muscle arising from the ligament of Struthers and the supracondylar process and a high bifurcation of the brachial artery, both of which have been implicated in median nerve entrapment. In addition, high branching of the AIN from the median nerve may be found13. The ligament of Struthers may be identified extending from the distal humerus to the medial epicondyle in the absence of a supracondylar process and may also serve as a point of entrapment10,14. On rare occasions entrapment of the ulnar nerve may be associated with the supracondylar process15. In symptomatic individuals, MRI demonstrates the courses of the median and ulnar nerves and the brachial artery in relation to the supracondylar process and ligament of Struthers and helps identify associated variant anatomy. In addition, radiographically occult fractures of the supracondylar process are readily demonstrated with MRI.
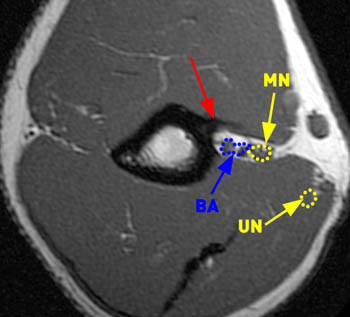
Figure 8:
Coronal and axial T1-weighted images of a 51 year-old male presenting with acute ulnar neuropathy and an abnormal x-ray demonstrate a supracondylar process (arrow) and the close proximity of the median nerve (MN) and brachial artery (BA). The ulnar nerve (UN) is seen medially, maintaining a normal course. In this case the supracondylar process was an incidental finding and did not contribute to the patient's symptoms.
Pronator Syndrome: Median nerve compression at the elbow and in the proximal forearm results in a pain syndrome that was originally coined by Seyffarth as the pronator syndrome, referring to the compressive neuropathy of the median nerve as it passes through the pronator teres16. In fact, a variety of musculotendinous, ligamentous, bony, and vascular structures may result in entrapment of the median nerve at or near the elbow leading to the clinical presentation of pronator syndrome. Median nerve entrapment is most common between the superficial (humeral) and deep (ulnar) heads of the pronator teres muscle17. In addition, variations in the pronator muscle including accessory origins of the deep head predispose to entrapment18. The next most common site of median nerve entrapment is at the fibrous arch formed between the two heads of the flexor digitorum superficialis muscle, found approximately 2 cm distal to the ulnar head of the pronator teres9. The lacertus fibrosus (aponeurosis of the distal biceps tendon) overlies the pronator teres muscle and the median nerve. Thickening of this structure can produce compression of the median nerve just proximal to the pronator muscles9.(7a)
Additional entities implicated in median nerve compression at the elbow include Gantzer’s muscle, palmaris profundus, and the flexor carpi radialis brevis. Gantzer’s muscle is an anomalous head of the flexor pollicis longus found in approximately 50% of individuals. This muscle receives innervation from the AIN and most commonly arises from the medial humeral epicondyle with a less frequent dual origin from the medial humeral epicondyle and the coronoid process19. This structure has a variable anatomic relationship to the AIN, which may pass anterior, medial, posterior, or posterolateral to the accessory muscle20. On axial images at the elbow, the accessory head of the flexor pollicis longus muscle may appear similar to a deep head of the pronator teres (9a). Following the structures distally demonstrates the accessory head of the flexor pollicis longus inserting into the ulnar border of the flexor pollicis longus muscle, allowing differentiation from the deep head of the pronator teres muscle21. Median nerve entrapment at the elbow has also been reported secondary to an enlarged bicipitoradial bursa, prolonged external compression, and fracture or dislocation at the elbow6.
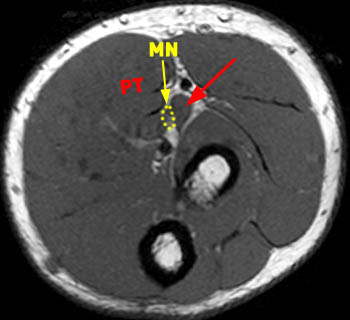
Figure 9:
This axial T1-weighted image demonstrates a presumed accessory head of the flexor pollicis longus muscle (arrow) situated deep to the median nerve (MN) and pronator teres muscle (PT). This accessory muscle may appear very similar to the deep head of the pronator teres. Following the muscle distally can help differentiate the two by demonstrating insertion of the accessory muscle into the flexor pollicis muscle.
Pronator syndrome typically presents with the insidious onset of chronic volar pain and numbness of the elbow, forearm, and hand with numbness and paresthesias of the thumb, index finger, middle finger, and the radial half of the ring finger. Weakness of the thenar muscles may rarely develop. Pronator syndrome is typically associated with strenuous activities such as weight lifting and occupations requiring repetitive pronation and supination of the forearm with the elbow extended. The clinical presentation may be confused with carpal tunnel syndrome because of the similarity of the distribution of sensory disturbance. In contrast to carpal tunnel syndrome, dysesthesias in the palmar triangle or in the skin overlying the thenar eminence are common in pronator syndrome because of innervation by the palmar cutaneous branch of the median nerve. This sensory branch arises proximal to and remains external to the carpal tunnel and is unaffected in carpal tunnel syndrome6. In contrast to the nocturnal symptoms typical of carpal tunnel syndrome, the symptoms of pronator syndrome are typically associated with activity. By physical examination, there may be pain with palpation of the pronator teres muscle, which may feel firm or mass-like. A positive Tinel sign (dysesthesia produced by tapping the nerve) may be elicited over the pronator muscle. Manual compression of the median nerve at the pronator teres muscle may reproduce clinical symptoms. Various provocative tests are used to try and localize the site of median nerve compression. Paresthesias resulting from resisted forearm pronation with elbow extension suggest compression at the pronator teres22. Pain or paresthesias resulting from resisted forearm supination and resisted elbow flexion suggest compression at the bicipital aponeurosis23. Paresthesias of the radial 3 digits with resisted flexion of the middle finger at the proximal interphalangeal joint suggest entrapment at the fibrous origin of the flexor digitorum superficialis15. Electrodiagnostic testing is often normal, but denervation is occasionally seen in the pronator teres, flexor carpi radialis, and flexor digitorum superficialis.
MRI evaluation typically demonstrates a normal appearing median nerve. Compressing masses or collections and primary masses of the nerve are well depicted (10a,10b). In most cases, entrapment arises from fibrous bands or anomalous muscles, which are not readily apparent on the MRI examination. Muscle signal changes, when present, reveal characteristic patterns of involvement. The pronator teres muscle is most commonly affected. Other muscles innervated by the median nerve and its branches distal to the level of entrapment may also demonstrate signal changes. In addition to the pronator teres, denervation changes may include the flexor carpi radialis, palmaris longus, flexor digitorum superficialis, flexor pollicis longus, and the radial part of the flexor digitorum profundus. In the acute or subacute stages intramuscular edema is present (11a,11b). Atrophy and fatty muscle replacement indicate chronic, irreversible changes of the denervated muscle (12a).
Anterior interosseous nerve syndrome (Kiloh-Nevin syndrome): The anterior interosseous nerve is a motor branch of the median nerve arising at the distal margin of the pronator teres muscle. The AIN is susceptible to injury at similar locations as the median nerve, but in general the compression is typically more distal than those of pronator syndrome. The most frequent causes of AIN syndrome are direct trauma and external compression from surgery, venous punctures or injection and cast pressure. Compression may result from a thickened tendinous origin of the ulnar head of the pronator teres, accessory muscles, a fibrous band arising from the flexor digitorum superficialis, and anomalous arteries. Patients may present with dull pain of the volar forearm and muscle weakness affecting the thumb, index finger, and occasionally the middle finger. Since the AIN is a motor branch, numbness of the skin is not associated with AIN syndrome.
AIN syndrome can be present with varying levels of severity24. In a complete AIN syndrome, as in the test case (Figures 1a and 1b),the flexor pollicis longus, radial half of the flexor digitorum profundus, and pronator quadratus are affected, and MRI demonstrates corresponding muscle edema or atrophy. Incomplete AIN syndromes may be seen with selective involvement of nerve fascicles that innervate the flexor pollicis longus (Fig 13) or of the flexor digitorum profundus (Fig 14) muscles with or without involvement of the pronator quadratus.
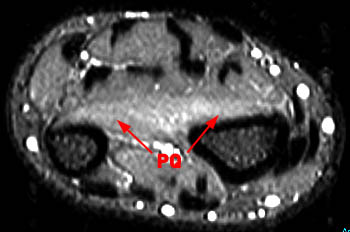
Figure 13:
Axial fat-suppressed proton density-weighted images of the mid (13a) and distal (13b) forearm in a 49 year-old male with acute onset of pain and loss of thumb flexion. Muscle edema is present in the flexor pollicis longus (FDP) and pronator quadratus (PQ) muscles consistent with incomplete AIN syndrome.
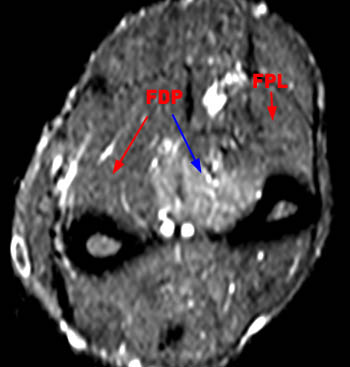
Figure 14:
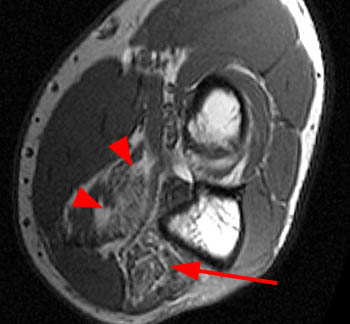
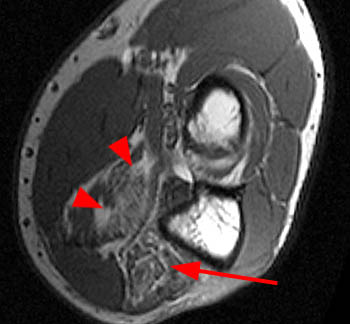
Axial STIR image through the forearm of a patient with a 3 month history of weakness of the index finger demonstrates an abnormal the flexor digitorum profundus muscle (FDP). Muscle edema is present in the radial aspect of the flexor digitorum profundus muscle (blue arrow), sparing the ulnar half of the flexor digitorum profundus muscle (red arrow) and of the flexor pollicis longus muscle (FPL).
Because approximately 50% of variant Martin-Gruber anastomoses arise between the AIN and ulnar nerve, AIN entrapment may involve ulnar nerve-supplied muscles. Denervation may affect the ulnar half of the flexor digitorum profundus muscle, which supplies the ring (FDP3) and little (FDP4) fingers resulting in weakness in all the fingers and signal changes throughout the entire flexor digitorum profundus muscle. In 30% of specimens the flexor digitorum superficialis is also innervated from the AIN24. AIN innervation may also include the flexor carpi radialis. The first dorsal interosseous, adductor pollicis, and/or abductor digiti minimi are most commonly affected in the hand. Therefore the presence of signal alterations within these muscles should not preclude a diagnosis of AIN entrapment in the presence of the characteristic muscle involvement and clinical symptoms25. Although described as the most common muscle involved in AIN syndrome, care should be taken in interpreting isolated pronator quadratus signal changes as evidence of AIN syndrome (15a). Mildly increased T2 signal is a frequent finding in asymptomatic individuals. In combination with signal abnormality of the FPL or flexor digitorum profundus, a denervation pattern consistent with AIN syndrome is more certain.
The clinical presentation of AIN syndrome often mimics rupture of the flexor tendons to the affected finger26. The patient is unable to form an “OK” with the index finger and thumb due to weakness of the flexor pollicis longus and/or the flexor profundus muscle of the index finger which are supplied by the AIN. In such cases, MRI easily identifies possible flexor tendon disruption. Brachial plexus neuritis (Parsonage-Turner syndrome) is another differential consideration in patients presenting with symptoms of AIN syndrome. In brachial neuritis there is typically no history of trauma, pain often precedes motor symptoms, and there is frequently a history of previous viral illness or vaccination. In these patients, MRI demonstrates patterns of denervation muscle edema that do not correspond to a single nerve distribution (16a).
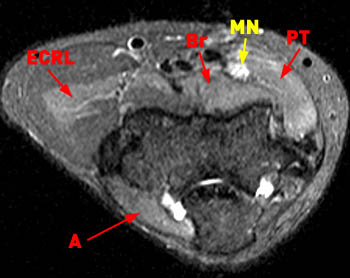
Figure 16:
Axial STIR image at the elbow in a patient with onset of right forearm numbness and tingling with weakness and no history of trauma. Increased muscle signal is demonstrated in the pronator teres (PT), brachialis (Br), extensor carpi radialis longus (ECRL), and anconeus (A). On more distal images increased signal was seen in the flexor carpi radialis muscle. There is increased signal along the median nerve (MN) indicating edema and neuritis, however the distribution of muscle signal changes include those innervated by the median nerve as well as the radial nerve and musculocutaneous nerve suggesting brachial neuritis as the likely etiology.
Treatment
In patients with supracondylar process syndrome, surgical resection of the ligament of Struthers or supracondylar process is curative. Treatment of pronator syndrome and anterior interosseous syndrome are similar. Conservative measures including physical therapy, modification of activities, and anti-inflammatory medication are indicated for initial management. Various lengths of conservative management are reported with most recommending a conservative trial of 12 weeks27. Surgery is reserved for patients failing conservative measures or in those patients with a compressing tumor or other underlying lesion.
Conclusion
Clinically differentiating the syndromes caused by compression of the median nerve and its branches at and near the elbow is often confusing. Variations in muscular anatomy and innervation may lead to ambiguous clinical and electrodiagnostic examinations. MRI is helpful in differentiating these syndromes. MRI is very effective in detecting masses or other lesions that result in nerve compression and can identify conditions which may mimic nerve compression. In cases of entrapment, MRI demonstrates patterns of muscle signal abnormalities, which indicate the compressed nerve and level of involvement and can differentiate acute and subacute denervation from chronic denervation of the muscle. This information is valuable for the clinician in directing conservative or surgical therapy.
References
1 Linda D, Harish S, Stewart B, Finlay K, Parasu N, Rebello R. Multimodality Imaging of Peripheral Neuropathies of the Upper Limb and Brachial Plexus. Radiographics 2010; 30:1373-1400.
2 Nebot-Cegarra J, Perez-Berruezo J, Reina de la Torre F. Variations of the pronator teres muscle: predispositional role to median nerve entrapment. Arch Anat Histol Embryol. 1991-1992; 74:35-45.
3 Fuss FK, Wurzl GH. Median nerve entrapment. Pronator teres syndrome. Surgical anatomy and correlation with symptom patterns. Surg Radiol Anat 1990; 12:267-271.
4 Boles CA, Kannam S, Cardwell A. The Forearm: Anatomy of Muscle Compartments and Nerves. AJR 2000; 174:151-159.
5 Pecina M, Boric I, Anticevic D. intraoperatively proven anomalous Struther’s ligament diagnosed by MRI. Skeletal radiol 2002; 31:532-535.
6 Bezerra A, Carvalho VC, Nucci A. An anatomical study of the palmar cutaneous branch of the median nerve. Surg Radiol Anat 1986; 8:183-188.
7 Doyle J, Botte MJ. Surgical anatomy of the hand and upper extremity. Philadelphia: Lippincott William and Wilkins, 2003: 407-460.
8 Rodriguez-Niedenfuhr M, Vazquez T, Parkin I, Logan B, Sanudo JR. Martin-Gruber anastomosis revisited. Clin Anat 2002; 15(2):129-134.
9 Chung C. Miscellaneous Disorders of the Elbow. In: Chung C and Steinbach L, eds. MRI of the Upper Extremity-Shoulder, Elbow, Wrist and Hand. Philadelphia, Lippincott Williams and Wilkins, 2010, 491-525.
10 Andreisek G, Crook DW, Burg D, Marincek B, Weishaupt D. Peripheral Neuropathies of the Median, Radial, and Ulnar Nerves: MR Imaging Features. Radiographics 2006; 26:1267-1287.
11 Kamath S, Venkatanarasimha N, Walsh M. MRI appearance of muscle denervation. Skeletal Radiol 2008; 37:397-404.
12 Kessel L, Rand M. Supracondylar spur of the humerus. J Bone Joint Surg. 48-B: 765-769, 1966.
13 Gunther S, DiPasquale D, Martin R. Struthers’ ligament and associated median nerve variations in a cadaveric specimen. Yale Journal of Biology and Medicine. 1993; 66:203-208.
14 Smith RV, Fisher RG. Struthers ligament: a source of median nerve compression above the elbow. J Neurosurg 1973; 38:778-779.
15 Resnick D. Entrapment Neuropathies. In: Resnick DL, Kang HS, Pretterklieber ML. Internal Derangements of Joints, 2nd Ed. Philadelphia, Saunders, 2007, 630-710.
16 Seyffarth H. Primary myoses in the m. pronator teres as cause of the n. medianus (the pronator syndrome). Acta Psychiatr Scan Suppl 1951; 74:251-254.
17 Johnson R, Spinner M, Shrewsbury M. Median nerve entrapment syndrome in the proximal forearm. J Hand Surg 1979; 4:48-51.
18 Nebot-Cegarra J, Reina-de la Torre F, P?rez-Berruezo J. Accessory fasciculi of the human pronator teres muscle: incidence, morphological characteristics and relation to the median nerve. Ann Anat. 1994 Jun; 176(3):223.
19 Al-Qattan M. GANTZER’S MUSCLE An anatomical study of the accessory head of the flexor pollicis longus muscle. J Hand Surg (Br) 1996; (21B): 2: 269-270.
20 Mahakkanukrauh P, Surin P, Ongkana N, Sethadavit M, Vaidhayakarn P. Prevalence of accessory head of flexor pollicis longus muscle and its relation to anterior interosseous nerve in Thai population. Clinical Anatomy 2004 ;( 17)8: 631-635.
21 Sookur P, Naraghi A, Bleakney R, Jalan R, Chan O, White L. Accessory Muscles: Anatomy, Symptoms, and Radiologic Evaluation. RadioGraphics 2008; 28:481-499.
22 Tetro A, Pichora DR. High median nerve entrapments: an obscure cause of upper extremity pain. Hand Clin 1996; 12:691-703.
23 Swiggett R, Ruby LK. Median nerve compression neuropathy by the lacertus fibrosis: report of three cases. J Hand Surg 1986; 11A:700-703.
24 Koo JT, Szabo RM. Compression Neuropathies of the Median Nerve. Journal of the American Society for Surgery of the Hand 2004; 4(3):156-175.
25 Dunn AJ, Salonen DC, Anastakis DJ. MR imaging findings of anterior interosseous nerve lesions. Skeletal Radiol. 2007; 36:1155-1162.
26 Mody BS. A simple clinical test to differentiate rupture of flexor pollicis longus and incomplete anterior interosseous paralysis. J Hand Surg (Br). 1992; 17:513-514.
27 Dang AC, Rodner CM. Unusual compression neuropathies of the forearm, Part II: Median Nerve. J Hand Surg 2009; 34A:1915-1920.