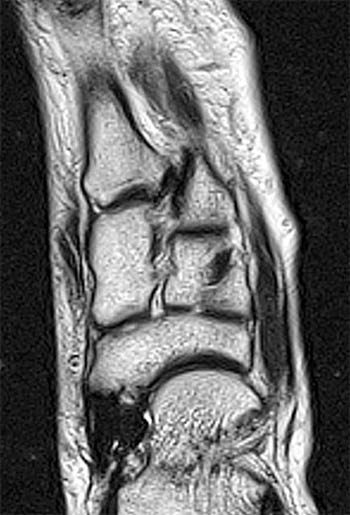
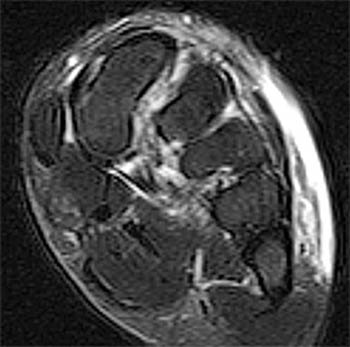
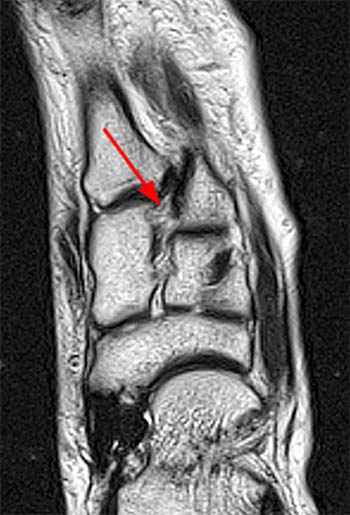
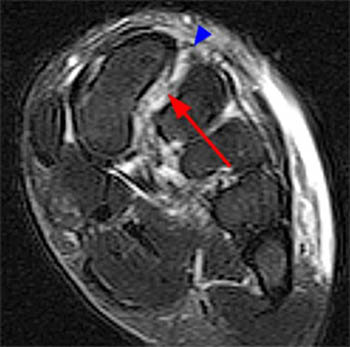
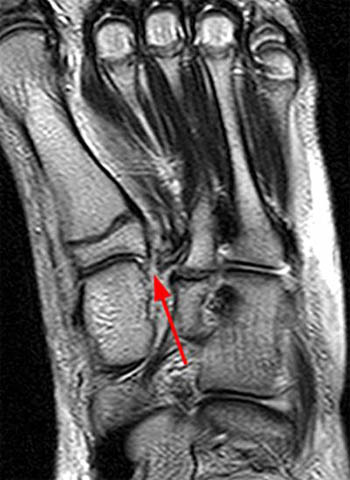
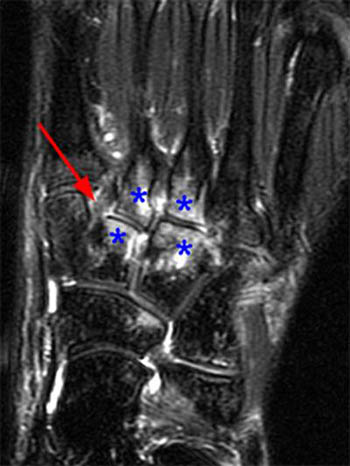
Clinical History: A 17 year-old male presents with the history of pain due to a football injury incurred three days prior. (1a) Axial T2-weighted and (1b) coronal fat suppressed T2-weighted images of the right midfoot are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
Lisfranc ligament tear.
Introduction
In the general population, injuries to the Lisfranc ligament complex are uncommon, occurring in approximately 1 in 50,000 people.1 The incidence of Lisfranc joint fracture dislocations is approximately 1 in 55,000 persons each year.2 Thus, these injuries account for fewer than 1 percent of all fractures.3,4
The injuries typically occur as a result of high-velocity indirect trauma, such as from a motor vehicle accident, and result in obvious displacement and disruption of the midfoot anatomy. Midfoot sprains in athletes represent a lower-velocity injury, typically with no displacement or with only subtle diastasis.1
Although sprains of the midfoot are not common in the general population, certain athletes suffer a much higher rate of this injury. Midfoot sprains are the second most common athletic foot injury after injury to the metatarsophalangeal joint, and occur in 4% of football players per year, with offensive linemen incurring 29.2% of midfoot sprains in one study.5
History
The Lisfranc joint, or tarsometatarsal articulation of the foot, is named after Jacques Lisfranc (1790-1847), a field surgeon in Napoleon’s army. Lisfranc described an amputation performed through this joint because of gangrene that developed after an injury incurred when a soldier fell off a horse with his foot caught in the stirrup.3,6
Clinical Presentation
Sprains in the midfoot region have subtle examination findings that can make diagnosis difficult. In one study,5 swelling was not a reliable indicator because it was most often mild. The location of tenderness to palpation to the tarsometatarsal joints and the reproduction of pain localized to the tarsometatarsal region by passive pronation and supination through the midfoot region were found to be the most reliable indicators of the minor sprains. The more severe injuries did not allow weightbearing on the involved foot. The inability of a player to perform a one-legged toe raise, cutting maneuvers, or jumps suggested a significant injury to the tarsometatarsal region.
Normal Anatomy
The Lisfranc joint is a complex skeletal and capsuloligamentous structure that provides significant stability while maintaining the transverse arch of the foot.7 The Lisfranc joint forms a shallow arc between the medial base of the second metatarsal and the lateral margin of the distal medial cuneiform, a configuration that gives it little bony stabilization.8 The bony architecture of this joint, specifically the “keystone” wedging of the second metatarsal into the cuneiform, forms the focal point that supports the entire tarsometatarsal articulation.3
To lessen ambiguity, some investigators have suggested that the term “Lisfranc joint complex” should be used to refer to tarsometatarsal articulations and that the term “Lisfranc joint” should be applied to medial articulation involving the first and second metatarsals with the medial and middle cuneiforms.9
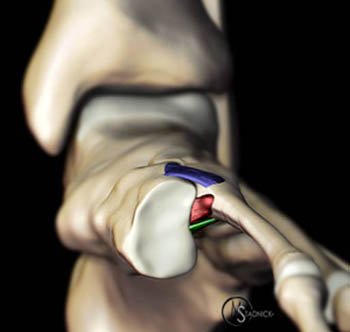
Unlike the other metatarsal bases, there is no intermetatarsal ligament between the base of the first and second metatarsals. This allows the first metatarsal increased sagital mobility, being tethered only by its attachments to the medial cuneiform.10 Instead, stability between the first and second rays is achieved by ligaments extending from the lateral margin of the medial cuneiform to the medial margin of the second metatarsal base. In the interest of simplicity and clarity, at least one author 8 suggests that the ligaments between the medial cuneiform and second metatarsal be referred to as the “dorsal,” “interosseous,” and “plantar” Lisfranc ligaments (Figures 5a,6a,7a and 8a) and that the three ligaments in combination be designated the “Lisfranc ligament complex.”
Mechanism of Injury
The anatomic complexity at the Lisfranc joint complex leads to multiple injury patterns.11 Sprains are the most common injury, with the midfoot sprain being the least severe injury.12 The severity of the sprain usually depends upon the energy absorbed at the time of injury. Most tarsometatarsal ligament injuries are grade I (pain at the joint, with minimal swelling and no instability) or grade II (increased pain and swelling at the joint, with mild laxity but no instability). The more severe grade III sprain represents complete ligamentous disruption and may represent fracture-dislocation.13 Several further classifications of true fracture-dislocations are used,14 but they do not predict prognosis.11,15
Lisfranc joint fracture dislocations and sprains can be caused by high-energy forces in motor vehicle crashes, industrial accidents and falls from high places.3,4,6 Occasionally, these injuries result from a less stressful mechanism, such as a twisting fall. Since Lisfranc joint fracture dislocations and sprains carry a high risk of chronic secondary disability, physicians should maintain a high index of suspicion for these injuries in patients with foot injuries characterized by marked swelling, tarsometatarsal joint tenderness and the inability to bear weight.3
HIGH-VELOCITY INJURY
This type of injury to the Lisfranc joint typically occurs with major, high-velocity trauma such as motor vehicle accidents or falls from a height. The force on the Lisfranc joint is abduction and/or plantar flexion. The joint is grossly dislocated, and fractures of the metatarsals or cuneiforms are commonly seen.16
Fracture dislocations are classified as either homolateral with all five metatarsals displaced in either the medial or lateral direction, or divergent, where a separation of the first and second metatarsals occurs.
LOW-VELOCITY INJURY: MIDFOOT SPRAIN
Low-velocity injuries can also result in mechanically significant disruption of the Lisfranc joint. Two injury mechanisms have been described. The first mechanism is plantar flexion and axial load, sometimes with a component of inversion.4 It occurs when the patient’s foot is plantar flexed and suffers an axial load injury. This injury may occur during running and jumping sports or when a patient trips going downstairs or stepping off a curb. It also may occur when a downward force is applied to the heel when the patient’s knee is on the ground and the ankle is dorsiflexed.
The second mechanism is forced forefoot abduction.12 This injury may also occur when an athlete wearing cleats plants the foot and turns quickly. In both mechanisms of injury, stress is applied to the Lisfranc ligament complex, and ligament failure, referred to as “midfoot sprain”, occurs. Midfoot sprain is uncommon in non-athletes, but in athletes it is the second most common athletic foot injury, occurring in 4% of football players per year.5
MRI Findings
As many as 20 percent of Lisfranc joint injuries are missed on initial anteroposterior and oblique radiographs.4,15 MR imaging has been shown to demonstrate the Lisfranc ligament complex reliably in the normal foot.17 Three distinct structures can be identified: the dorsal, plantar, and interosseous ligaments (Figures 4a-7a). The interosseous ligament is the strongest and thickest of the three ligaments. It is 8 to 10 mm long and 5 to 6 mm thick.8(Figure 8a) The three components in the Lisfranc ligament complex fail sequentially from dorsal to plantar.(Figure 9a) MR imaging frequently shows small avulsion fractures that are not visible on radiographs.18 The fractures usually arise from the base of the second metatarsal, though other midfoot contusions and fractures are often seen as well.(Figure 10a) Bone bruises without avulsions are commonly encountered and are a useful secondary sign raising suspicion for a Lisfranc ligament complex injury.(Figure 11a)
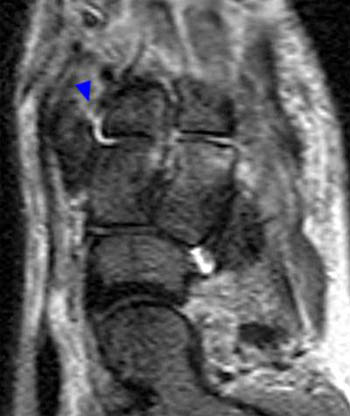
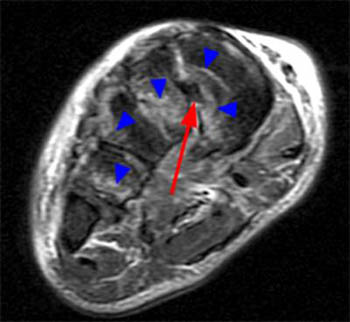
Figure 8:
Axial T2 image demonstrating tear of the interosseous component of the Lisfranc ligament complex(arrow) in a 15 year old following a jet ski accident. The patient also suffered disruption of the other Lisfranc components, as well as comminuted fracture of the base of the second metatarsal.
Discussion
Lisfranc joint injuries are very uncommon and often misdiagnosed. Typical signs and symptoms include pain, swelling and the inability to bear weight. These injuries vary from mild sprains (typically in an athlete) to fracture-dislocations (as seen in motor vehicle accidents). On physical examination, swelling is found primarily over the midfoot region. Pain is elicited with palpation along the tarsometatarsal articulations, and force applied to this area may elicit medial or lateral pain.
Subtle mid-foot sprains (diastasis of 1 to 5 mm) are difficult to diagnose and can cause significant disability and frustration in athletes. Partial capsular tears result in no diastasis but can result in an inability to play sports at an elite level for many months.1
A missed diagnosis has serious consequences. An untreated midfoot sprain leads rapidly to osteoarthritis and flattening of the longitudinal arch. Treatment is usually surgical.1,15,20
Radiographs showing diastasis of the normal architecture confirm the presence of a severe sprain and possible dislocation. Negative standard and weight-bearing radiographs do not rule out a mild (grade I) or moderate (grade II) sprain. MRI imaging may be necessary if pain and swelling persist days beyond the time of initial injury. Proper treatment of a mild to moderate Lisfranc injury improves the chance of successful healing and reduces the likelihood of complications. Patients with fractures and fracture-dislocations should be referred for surgical management.19
Conclusion
MRI imaging can prove very helpful for the evaluation of injuries to the midfoot, particularly in the setting of normal radiographs. Specific injuries to the components of the Lisfranc ligament complex can be detected. Other injuries to this region that are exclusive of the Lisfranc ligament complex, such as midfoot contusions and fractures, are also well demonstrated. The accurate diagnosis of Lisfranc and related injuries in the patient with midfoot pain allows appropriate conservative or surgical treatment to be instituted.
References
1 Nunley J, Vertullo C. Classification, Investigation, and Management of Midfoot Sprains. Am J Sports Med 2002;30:871-8
2 Cheung Y, Rosenberg ZS. MR Imaging of Ligamentous Abnormalities of the Ankle and Foot. MRI Clinics of North America 2001;9:507-31
3 Englanoff G, Anglin D, Hutson HR. Lisfranc fracture-dislocation: a frequently missed diagnosis in the emergency department. Ann Emerg Med 1995;26:229-33
4 Mantas JP, Burks RT. Lisfranc injuries in the athlete. Clin Sports Med 1994;13:719-30
5 Meyer SA, Callaghan JJ, Albright JP, et al: Midfoot sprains in collegiate football players. Am J Sports Med 1994;22:392-401
6 Vuori JP, Aro HT. Lisfranc joint injuries: trauma mechanisms and associated injuries. J Trauma 1993;35:40-5
7 de Palma L, Santucci A, Sabetta SP, et al: Anatomy of the Lisfranc joint complex. Foot Ankle Int 1997;18: 356-64
8 Crim J. MR Imaging Evaluation of Subtle Lisfranc Injuries: The Midfoot Sprain. MRI Clinics of North America 2008;16:19-27
9 Myerson M. The diagnosis and treatment of injuries to the Lisfranc joint complex. Orthop Clin North Am 1989;20:655-64
10 Shapiro M, Wascher, D, Finerman, G. Rupture of Lisfranc’s Ligament in Athletes. Am J Sports Med 1994;22:687-91
11 Heckman JD. Fractures and dislocations of the foot. In: Rockwood CA, Green DP, Bucholz RD, eds. Rockwood and Green’s Fractures in adults. Vol 2. 3d ed. Philadelphia: Lippincott, 1991:2140-51
12 Curtis MJ, Myerson M, Szura B. Tarsometatarsal joint injuries in the athlete. Am J Sports Med 1993;21:497-502
13 Kraeger DR. Foot injuries. In: Lillegard WA, Rucker KS, eds. Handbook of sports medicine: a symptom-oriented approach. Boston: Andover Medical, 1993:159-71
14 Brown DD, Gumbs RV. Lisfranc fracture-dislocations: report of two cases. J Natl Med Assoc 1991; 83:366-9
15 Trevino SG, Kodros S. Controversies in tarsometatarsal injuries. Orthop Clin North Am 1995;26:229-38
16 Hardcastle PH, Reschauer R, Kutscha-Lissberg E, et al. Injuries to the tarsometatarsal joint: incidence, classification and treatment. J Bone Joint Surg Br 1982;64B:349-56
17 Preidler KW, Wang YC, Brossman J, et al. Tarsometatarsal joint: anatomic details on MR images. Radiology 1996;199:733-6
18 Preidler KW, Brossman J, Daenen B, et al. MR imaging of the tarsometatarsal joint: analysis of injuries in 11 patients. Am J Roentgenol 1996;167:1217-22
19 Burroughs K, Reimer, C, Fields, K. Lisfranc Injury of the Foot: A Commonly Missed Diagnosis. Am Fam Phys 1998;http://www.aafp.org/afp/AFPprinter/980700ap/burrough.html
20 Ly TV, Coetzee JC. Treatment of primarily ligamentous Lisfranc joint injuries: primary arthrodesis compared with open reduction and internal fixation. J Bone Joint Surg 2006;88A:514-20.