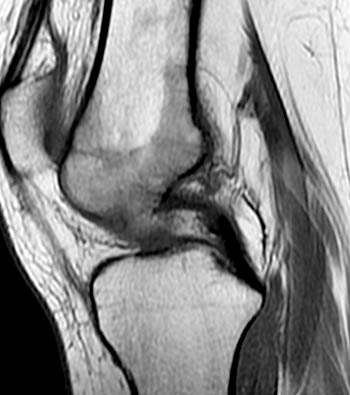
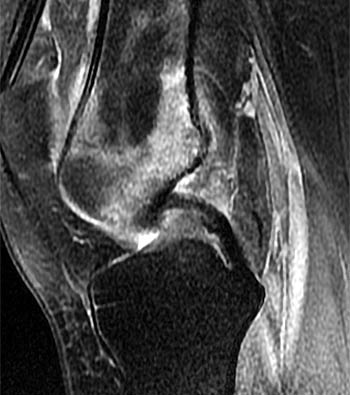
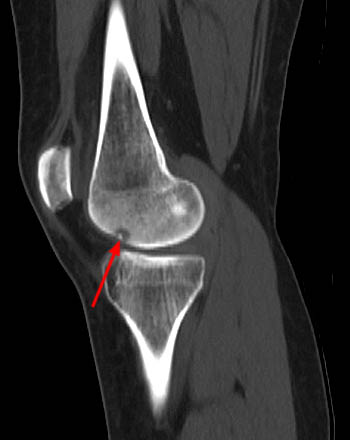
Clinical History: A 29 year-old female complains of progressive knee pain and stiffness without a history of trauma. A radiograph (not shown) demonstrated no abnormality. T1-weighted (1a) and proton density fat suppressed (1b) sagittal images of the knee are provided. What are the findings? What is your diagnosis?
Findings
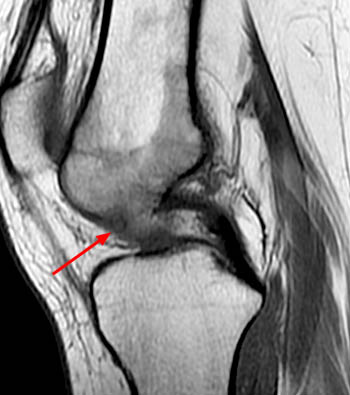
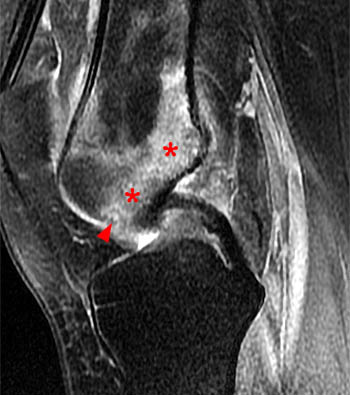
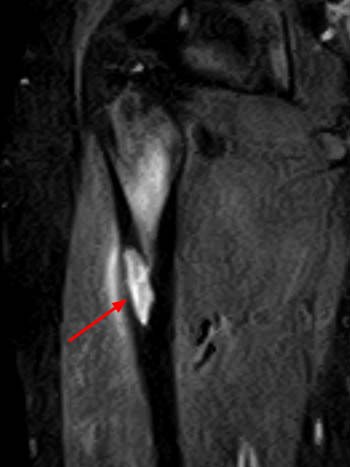
Figure 2:
(2a) The sagittal T1-weighted image demonstrates a cortical and subcortical lesion with a circular rim of decreased signal intensity (arrow). (2b) The sagittal proton density fat-suppressed image reveals that the very center of the lesion has decreased signal intensity (arrowhead). Prominent marrow edema involves the distal femur (asterisks).
Diagnosis
Intraarticular osteoid osteoma.
Introduction
Osteoid osteomas are relatively common, accounting for approximately 12% of benign osseous tumors.1 Jafee is given credit for correctly identifying osteoid osteoma in 1935 as a distinct benign lesion.2 Prior to Jafee’s description, osteoid osteomas were thought to represent chronic infections and were given diagnoses such as chronic bone abscess and sclerosing nonsuppurative osteomyelitis.3,4
Although the diagnostic criteria for osteoid osteomas is well established and the pathology and clinical presentations have been studied for decades, to date no proven etiology has been established. It is not even certain if osteoid osteomas are inflammatory or neoplastic lesions. Different etiologies have been proposed including antecedent trauma, and infection.1,3,5-8
Pathology
The term nidus as it applies to an osteoid osteoma is a misnomer in that the nidus represents the entire osteoid osteoma and not just the central portion. Abandoning the term nidus would eliminate possible confusion and the inaccuracy of the term. Osteoid osteomas are usually 1 cm or less and are composed of vascular connective tissue with osteoblastic activity.(C) Within the lesion are osteoid and bony trabeculae with variable mineralization.7,8 The host bone surrounding lesion is robust with woven and lamellar bone.3
Prostaglandins are associated with osteoid osteomas and may have a role in the formation of these lesions. Up to a 1000-fold increase in levels of prostaglandins can be found around the lesion and this resolves after surgical removal. The prostaglandins are believed to be involved in the prototypical pain syndromes of osteoid osteomas. Pain relief with salicylates or other nonsteroidal anti-inflammatory drugs (NSAIDs), which inhibit prostaglandins, supports the role of prostaglandins in pain causation with osteoid osteomas.6
Classification
In a 1966 report, Edeiken divided osteoid osteomas into three types:9
- Cortical: Causes fusiform sclerotic cortical thickening of the long bone, most commonly involves the tibia (4a) and femur, has radiolucent area in the center of sclerosis, and the sclerosis regresses after resection.
- Cancellous (medullary): Common sites femoral neck, bones of hand and foot and posterior elements of the vertebrae. Sclerosis, when present, mild to moderate and can be distant from the lesion and the lesion may be eccentric. (5a,5b)
- Subperiosteal: Soft tissue mass adjacent to affected bone, typical locations medial aspect femoral neck, hands and feet, and neck of talus.3,9
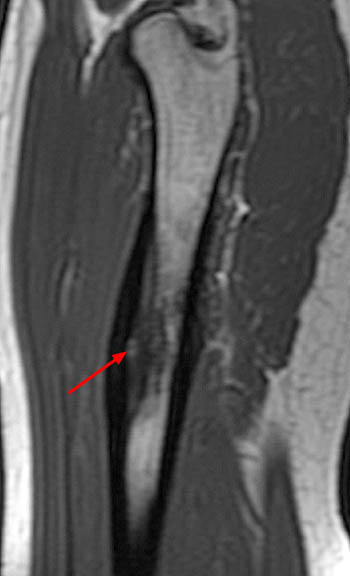
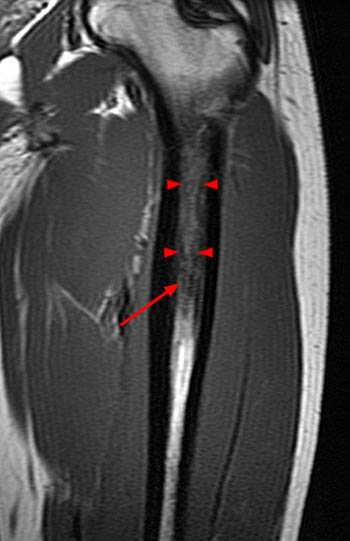
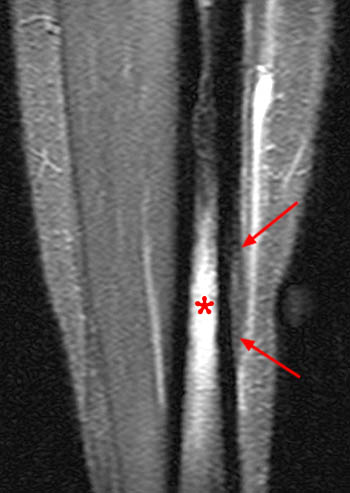
Figure 5:
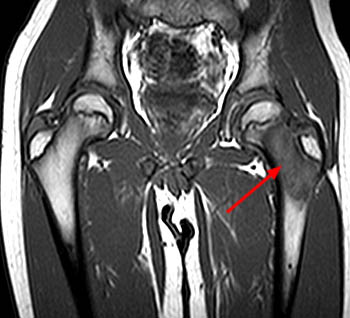
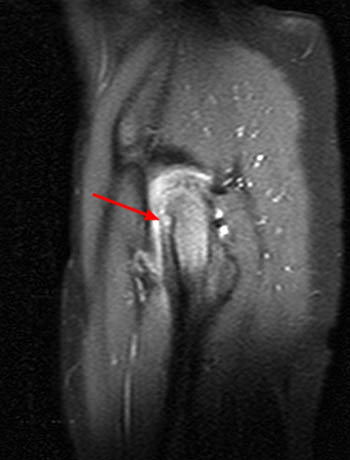
(5a) A sagittal T1-weighted images shows a femoral osteoid osteoma (arrow) in the cancellous subcortical bone, causing a combination of cortical and cancellous bone thickening. (5b) The corresponding T1-coronal image demonstrates that the cancellous bony changes (arrowheads) eccentrically extend superior to the level of the lesion (arrow).
Some authors add endosteal as a fourth type but Edeiken’s classification system is considered the more traditional.10,11 The differentiation of cortical, subperiosteal and cancellous types can be subjective and the criteria has changed over time. For example, in a 2010 article by Chai and others, an osteoid osteoma in the cortex but towards the outer margin was classified as subperiosteal.10 Many of the lesions now being called subperiosteal would have been categorized as cortical in previous years. Clinically, the type assigned to the lesion is not important. From a diagnostic standpoint, most extraarticular osteoid osteomas occurring near the cortex will have a discernable lesion and prominent sclerotic reaction. The intraarticular osteomas are problematic lesions both in terms of being more difficult to detect and in terms of having a nonspecific appearance. Osteoid osteomas occurring near ends of long bones surrounded by or close to capsule are considered intraarticular.12 Based on what has been learned about osteoid osteomas, a more useful classification in terms of diagnostic criteria, clinical presentation and treatment would be to classify the lesions as being extraarticular, intraarticular and spinal.
Location
The majority of cortical osteoid osteomas are in the lower extremities and >50% involve the femur and tibia. The majority of cortical osteoid osteomas are diaphyseal and metadiaphyseal in location. Approximately 5% of osteoid osteomas are epiphyseal.7,8 The distribution for osteoid osteomas is as follows: cortical (47-80%), subperiosteal (15-47%) and medullary (5%).7,8,11 Approximately 30% of osteoid osteomas are divided between the spine, hand and foot.13 Most spinal osteoid osteomas are found in the lumbosacral region. Spinal osteoid osteomas almost always arise in the posterior elements and only rarely in the vertebral body proper.14 Osteoid osteomas can occur in any osseous structure with unusual sites including the skull, the ribs, the ischium, the mandible, the elbow (6a,6b) and the patella (7a).13
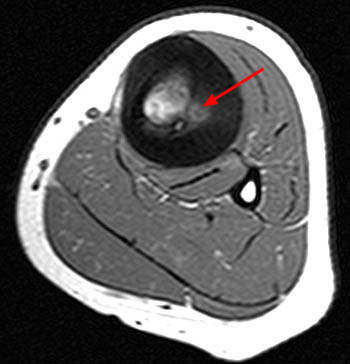
Figure 6:
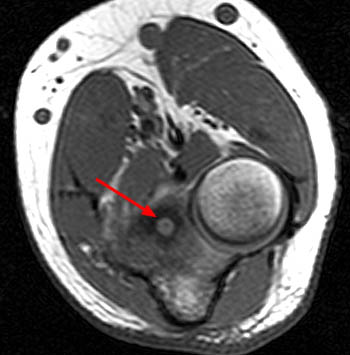
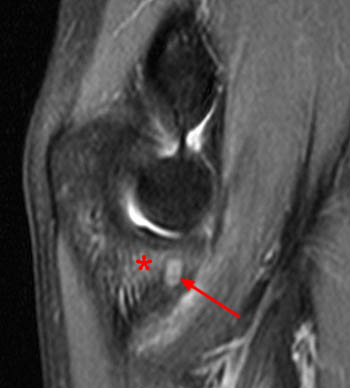
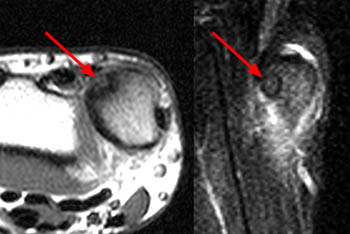
(6a) An axial T1-weighted image demonstrates a well circumscribed osteoid osteoma in the coronoid process of the proximal ulna (arrow). (6b) The corresponding sagittal fat-suppressed proton density image shows the osteoid osteoma in the coronoid process (arrow) surrounded by marrow edema (asterisk). Note that no cortical thickening is present because of the intraarticular location of the lesion.
Clinical presentation
Osteoid osteomas typically occur in younger individuals, and approximately 50% occur between the ages of 10-20 years. Osteoid osteomas are uncommon for patients <5 or >40 years of age.15 Multiple series have confirmed a male predominance, and in Kransdorf’s series from the Armed Forces Institute of Pathology, the male:female ratio was 3.85:1 and in the same series, osteoid osteomas were uncommon in non-white patients.3 Pain is the dominant and often the only presenting complaint of a patient with an osteoid osteoma. The pain typically progresses from mild and intermittent to severe and constant. The pain is often worse at night and studies have shown that up to 75% get symptomatic relief with salicylates.1,6 Occasionally osteoid osteomas are painless. In the AFIP series, 5% of the osteoid osteomas were painless and presented with swelling and half of these occurred in the fingers.3 Patients with osteoid osteomas typically do not have systemic symptoms, lab abnormalities, erythema and heat. Lower extremity osteoid osteomas can be associated with limp and muscle atrophy. Growth disturbances can occur including leg length discrepancy. Osteoid osteomas of the spine can cause painful scoliosis from reactive spasm.3,6 (8a)
Prior to the advent of the widespread use of nuclear scintigraphy, CT and MRI, osteoid osteomas were notorious for having a delay in diagnosis. Pettine reported that the implementation of bone scanning decreased the mean interval from the beginning of symptoms to diagnosis from 35 months to 12 months.14
Intraarticular osteoid osteomas present with nonspecific joint related symptoms including joint effusions and synovitis. Findings on physical examination include loss of range of motion, weakness, flexion deformity, atrophy and advanced epiphyseal development.1,6,13,16 Osteoarthritis is a reported complication of intraarticular osteoid osteomas.17
In the hands and feet, osteoid osteomas tend to cause less reactive sclerosis. Because of the proximity of the osseous structures, an inflammatory reaction originating in one osseous structure can spread to adjacent bones and joints. Accompanying soft tissue swelling can resemble infection or inflammatory arthritis.10 (9a) Many of the lesions in the hand and feet are intraarticular.
The natural history of osteoid osteomas is poorly understood. A small number of reports indicate that some osteoid osteomas spontaneously involute.3,18 Many of the osteoid osteomas that reportedly spontaneously resolved or “burned out”, however, never had histologic verification. Currently, many osteoid osteomas that are treated with minimally invasive techniques do not have histologic proof. The diagnosis of these lesions is based on clinical and imaging presentations. The reasons for not doing biopsies is that frozen sections cannot be done on osteoid material so a staged procedure would be necessary. Additionally, the diagnostic accuracy of needle biopsies of osteoid osteomas has been reported as being in the range of 50%.19
The clinical presentations of osteoid osteomas have been divided into two stages: Stage one is hallmarked by acute pain that lasts 18-36 months, during which the patient will require a steady regimen of analgesics. The second stage or recovery stage, involves healing of the lesion over a period of 3-7 years.20
Imaging
Routine radiography
Osteoid osteomas can vary from being radiolucent to radiopaque on routine radiography. Typically the lesion is centrally positioned in an area of reactive sclerosis.3 The lesion is typically <1.5 cm and may not be visible when the sclerosis is advanced. Disuse regional osteoporosis may be present. Intraarticular osteoid osteomas can be particularly difficult to diagnose with routine radiography because of the relative absence of sclerotic reactions. The intraarticular periosteum does not produce a sclerotic reaction, unlike extraarticular periosteum.3,12 Subperiosteal osteoid osteomas typically present as juxtacortical masses with cortical disruption.3,12 As would be expected, osteoid osteomas in the spine are difficult to diagnose with routine radiography. The level of suspicion should be high in an adolescent with painful scoliosis. If a spinal osteoid osteoma can be seen with routine radiography, it presents as an area of sclerosis in the posterior neural arch.
Nuclear medicine
Bone scintigraphy is a sensitive diagnostic tool in the evaluation of osteoid osteomas. Although bone scintigraphy has limited specificity, it is usually correlated with other imaging studies. Some centers still rely on bone scintigraphy as part of the initial evaluation of osteoid osteomas. Other centers have moved to the use of CT and/or MRI because of the increased specificity, more precise localization of the lesion, ability to pre-operatively plan the approach to the lesion and the ability to diagnose processes other than osteoid osteomas.
Computed axial tomography (CT)
CT is both sensitive and specific for most osteoid osteomas. Typically the lesion is well defined with rounded margins surrounded by sclerosis. The lesion will have variable degrees of mineralization, varying from punctate calcifications to dense central calcification. Approximately 50% of lesions will have some degree of calcification.3 (10a) In clinical practice, when a routine radiograph shows a sclerotic reaction in a long bone consistent with an osteoid osteoma, then CT is the next study of choice to delineate the lesion. Some investigators have used dynamic contrast-enhanced CT to differentiate between osteoid osteomas and osteomyelitis, but this technique has not been widely embraced.21
MRI
The use of MRI in the evaluation of osteoid osteomas is evolving. Some studies have cautioned against the use of MRI because of a lack of sensitivity and specificity.22,23 Other investigators have found that MRI is superior to CT24 and in current clinical practice, the diagnosis of osteoid osteomas is routinely made with MRI alone. When the routine radiograph does not have sclerotic changes typical of an osteoid osteoma, then the next study of choice is MRI because it can detect soft tissue and marrow abnormalities that CT cannot detect. There are situations where CT is performed in addition to MRI when the lesion is not clearly defined with MRI.
For cortical and subperiosteal osteoid osteomas, the thickened cortex has predominately low signal intensity on all sequences. The osteoid osteoma lesion has low to intermediate signal intensity on T1-weighted and proton density-weighted sequences and low to high signal intensity on T2-weighted images. (11a,11b) In the marrow adjacent to the osteoid osteoma, the signal intensity is decreased on T1-weighted images and increased on T2-weighted images. After administration of gadolinium, variable enhancement patterns of the lesion can be seen. Gadolinium enhancement can be seen in the marrow and soft tissue adjacent to the osteoid osteomas because of reactive fibrovascular tissue and inflammatory cells. Intraarticular osteoid osteomas present with lesions that exhibit variable enhancement patterns. Dynamic enhanced MRI has been used to increase the conspicuity of osteoid osteomas but this technique has not been widely embraced.27
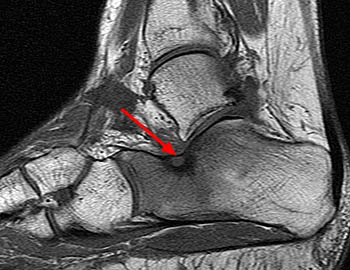
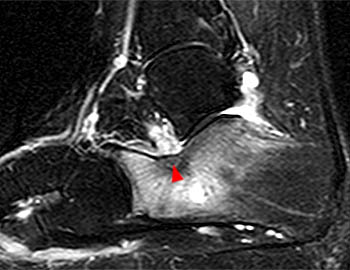
Figure 11:
(11a) A sagittal T1-weighted image reveals an osteoid osteoma in the calcaneus at the angle of Gissane (arrow), demonstrating intermediate signal intensity. (11b) The sagittal fat-suppressed T2 weighted image shows the lesion has small punctate foci of decreased signal intensity (arrowhead) and is surrounded by marked marrow edema. The signal intensity of osteoid osteomas varies depending on its composition.
Differential diagnosis
The differential diagnosis will vary according to the type and location of the osteoid osteoma. For cortical, subperiosteal and cancellous osteoid locations, a Brodie abscess can be difficult to distinguish from an osteoid osteoma. Both lesions typically occur in younger patients, typically occur in long bones, cause sclerotic reactions and have lucent central areas that can contain areas of mineralization. Patients with a Brodie abscess may or may not have helpful systemic or laboratory findings. It has been reported that an osteoid osteoma has smooth inner margins whereas a Brodie abscess has irregular margins and a sequestrum, if present, is irregular and eccentric.28 Stress fractures may also be in the differential, as they typically present in the younger population and can also cause intense sclerotic reactions. Often but not always, with CT or MR, a fracture line can be seen even when the sclerotic reaction is profound.(12a,13a) Other lesions in the differential diagnosis include osteoblastoma and sclerosing osteomyelitis.7,8
For cortical and subperiosteal osteoid osteomas, other lesions in the differential include parosteal osteosarcoma, osteofibrous dysplasia, adamantinoma, fibrous cortical defect and osteoma. For cancellous osteoid osteomas, other lesions in the differential diagnoses would include bone island, metastatic disease and hemangioma.7,8
The differential diagnosis for intraarticular osteoid osteomas includes osteoblastoma and Brodie abscess, and also includes eosinophilic granuloma, inflammatory synovitis, septic joint, osteochondral lesions, chondroblastoma, intraosseous ganglion (14a) and synovial pit.7,8,10
Figure 14:
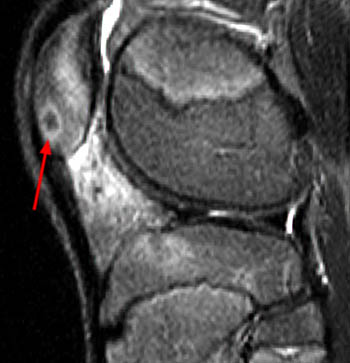
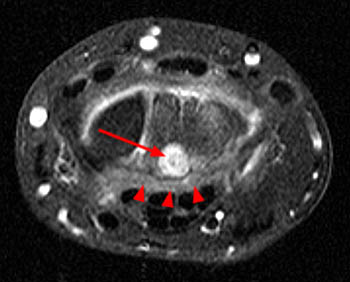
T1-weighted axial and coronal STIR images demonstrate a well circumscribed lesion in the distal ulna (arrows) with marrow and soft tissue edema. Pre-operatively this was diagnosed as an osteoid osteoma but at surgical excision, this proved to be an intraosseous ganglion. The relatively low signal intensity appearance on the STIR image is an atypical appearance for an intraosseous ganglion.
In the spine, osteoid osteomas are indistinguishable from smaller osteoblastomas in terms of imaging and histology. Osteoblastomas are typically larger than osteoid osteomas (>2 cm) and have a different biological behavior with continued growth if left untreated.
Treatment and Prognosis
The initial treatment of osteoid osteoma is with medications consisting of aspirin or other NSAIDs. (15a,16a) If patients can tolerate the side effects of NSAIDs, lasting pain relief can be achieved without the need for an interventional procedure. It has been suggested that ablative procedures be reserved for those who are unable or unwilling to take NSAIDs until their symptoms resolve.29
Interventional therapy for treatment of an osteoid osteoma involves either conventional surgical excision or a percutaneous procedure, of which there are several types. Complete surgical resection of the lesion is usually curative with immediate relief of symptoms and regression of osseous changes.3,5 The success rate is in the range of 88%-97%.30,31 Intraoperative localization of the lesion can be difficult and can be aided with needle localization with CT, CT guidance for resection, intraoperative scintigraphy and preoperative administration with tetracycline and examination of the tissue in situ with ultraviolet light.3,32,33 Most surgical failures are because the lesion was not recognized and resected. Surgical complications, although infrequent, include fractures secondary to structural weakening from the osseous resection. Articular or epiphyseal lesions require arthrotomy which can cause impairment of growth and joint mobility. The average hospital stay is 3-5 days and weight bearing activity is limited for 1-6 months.33-37
Percutaneous therapies are an attractive alternative to conventional surgical resection. Access is easier without the need for extensive soft tissue dissection. The lesion can be directly visualized during the procedure and this ensures precise localization. Percutaneous techniques include needle excision, alcohol ablation, laser ablation and thermal radiofrequency ablation. Typically these are done as outpatient procedures and daily activity can be resumed immediately. Complications tend to be infrequent and minor compared to conventional surgery.33-37
Summary
Osteoid osteomas are common benign osseous lesions of unknown etiology that typically present with progressive pain relieved with NSAIDs. Osteoid osteomas occur in younger patients, can spontaneously regress and are more common in males. Extraarticular osteoid osteomas elicit prominent sclerosis of the native bone surrounding the osteoid osteoma. Intraarticular osteomas tend to cause much less sclerosis, present with non-specific joint symptoms, can be difficult to detect and can have an appearance that is similar to other pathologic processes. Spinal osteoid osteomas should be suspected when younger patients present with painful scoliosis. Routine radiography can be helpful in the diagnosis of extra-articular lesions but is less sensitive for intraarticular and spinal lesions. Although nuclear medicine bone scans have a high sensitivity, CT and MRI are more specific and better suited for treatment decisions. The initial treatment of osteoid osteomas is with NSAIDs and ablative procedures are used when medical therapy fails or cannot be tolerated. Many osteoid osteomas are now treated percutaneously without histologic confirmation. It is important that the lesions undergoing percutaneous ablative therapy meet the clinical and imaging criteria for osteoid osteomas.
References
1 Dahlin DC, Unni KK. Bone tumors: general aspects and data on 8,542 cases. Springfield, IL: Thomas, 1987.
2 Jaffe HL. Osteoid osteoma: a benigh osteoblastic tumor composed of osteoid and atypical bone. Arch Surg 1935; 31:709-728.
3 Kransdorf MJ, Stull MA, Gilkey FW, Moser RP, Jr. Osteoid osteoma. Radiographics 1991; 11:671-696.
4 Jaffe HL, Lichtenstein L. Osteoid osteoma: further experience with this benign tumor of bone. J Bone Joint Surg 1940; 22:645-682.
5 Freiberger RH, Loitman BS, Helpern M, Thompson TC. Osteoid osteoma; a report on 80 cases. Am J Roentgenol Radium Ther Nucl Med 1959; 82:194-205.
6 Healey JH, Ghelman B. Osteoid osteoma and osteoblastoma. Current concepts and recent advances. Clin Orthop Relat Res 1986:76-85.
7 Mulder JD, Schutte HE, Kroon HM, Taconis WK. Osteoid osteoma. In:Radiolgic atlas of bone tumors. Amsterdam: Elsevier, 1993; 385-397.
8 Myers SP. Osteoid osteoma. In:MRI of bone and soft tissue tumors and tumorlike lesions. New York: Thieme, 2008; 660-667.
9 Edeiken J, DePalma AF, Hodes PJ. Osteoid osteoma. (Roentgenographic emphasis). Clin Orthop Relat Res 1966; 49:201-206.
10 Chai JW, Hong SH, Choi JY, et al. Radiologic diagnosis of osteoid osteoma: from simple to challenging findings. Radiographics 2010; 30:737-749.
11 Kayser F, Resnick D, Haghighi P, et al. Evidence of the subperiosteal origin of osteoid osteomas in tubular bones: analysis by CT and MR imaging. AJR Am J Roentgenol 1998; 170:609-614.
12 Kattapuram SV, Kushner DC, Phillips WC, Rosenthal DI. Osteoid osteoma: an unusual cause of articular pain. Radiology 1983; 147:383-387.
13 Jackson RP, Reckling FW, Mants FA. Osteoid osteoma and osteoblastoma. Similar histologic lesions with different natural histories. Clin Orthop Relat Res 1977:303-313.
14 Pettine KA, Klassen RA. Osteoid-osteoma and osteoblastoma of the spine. J Bone Joint Surg Am 1986; 68:354-361.
15 Mirra JM, Picci P, Gold RH. Bone Tumors. Philadelphia: Lea & Febiger, 1989.
16 Swee RG, McLeod RA, Beabout JW. Osteoid osteoma. Detection, diagnosis, and localization. Radiology 1979; 130:117-123.
17 Norman A, Abdelwahab IF, Buyon J, Matzkin E. Osteoid osteoma of the hip stimulating an early onset of osteoarthritis. Radiology 1986; 158:417-420.
18 Moberg E. The natural course of osteoid osteoma. J Bone Joint Surg Am 1951; 33:166-170.
19 Lindner NJ, Ozaki T, Roedl R, Gosheger G, Winkelmann W, Wortler K. Percutaneous radiofrequency ablation in osteoid osteoma. J Bone Joint Surg Br 2001; 83:391-396.
20 Atar D, Lehman WB, Grant AD. Tips of the trade. Computerized tomography-guided excision of osteoid osteoma. Orthop Rev 1992; 21:1457-1458.
21 McGrath BE, Bush CH, Nelson TE, Scarborough MT. Evaluation of suspected osteoid osteoma. Clin Orthop Relat Res 1996:247-252.
22 Assoun J, Richardi G, Railhac JJ, et al. Osteoid osteoma: MR imaging versus CT. Radiology 1994; 191:217-223.
23 Davies M, Cassar-Pullicino VN, Davies AM, McCall IW, Tyrrell PN. The diagnostic accuracy of MR imaging in osteoid osteoma. Skeletal Radiol 2002; 31:559-569.
24 Spouge AR, Thain LM. Osteoid osteoma: MR imaging revisited. Clin Imaging 2000; 24:19-27.
25 Allen SD, Saifuddin A. Imaging of intra-articular osteoid osteoma. Clin Radiol 2003; 58:845-852.
26 Woods ER, Martel W, Mandell SH, Crabbe JP. Reactive soft-tissue mass associated with osteoid osteoma: correlation of MR imaging features with pathologic findings. Radiology 1993; 186:221-225.
27 Liu PT, Chivers FS, Roberts CC, Schultz CJ, Beauchamp CP. Imaging of osteoid osteoma with dynamic gadolinium-enhanced MR imaging. Radiology 2003; 227:691-700.
28 Mahboubi S. CT appearance of nidus in osteoid osteoma versus sequestration in osteomyelitis. J Comput Assist Tomogr 1986; 10:457-459.
29 Ilyas I, Younge DA. Medical management of osteoid osteoma. Can J Surg 2002; 45:435-437.
30 Motamedi D, Learch TJ, Ishimitsu DN, et al. Thermal ablation of osteoid osteoma: overview and step-by-step guide. Radiographics 2009; 29:2127-2141.
31 Papathanassiou ZG, Megas P, Petsas T, Papachristou DJ, Nilas J, Siablis D. Osteoid osteoma: diagnosis and treatment. orthopaedics 2008; 31:1118.
32 Ayala AG, Murray JA, Erling MA, Raymond AK. Osteoid-osteoma: intraoperative tetracycline-fluorescence demonstration of the nidus. J Bone Joint Surg Am 1986; 68:747-751.
33 Assoun J, Railhac JJ, Bonnevialle P, et al. Osteoid osteoma: percutaneous resection with CT guidance. Radiology 1993; 188:541-547.
34 Albisinni U, Rimondi E, Malaguti MC, Ciminari R. Radiofrequency thermoablation in the treatment of osteoid osteoma. Radiology 2004; 232:304; author reply 304-305.
35 Gangi A. [The treatment of osteoid osteoma: a multitude of choice: surgery, percutaneous resection, alcohol injection or thermocoagulation]. J Radiol 1999; 80:419-420.
36 Gangi A, Alizadeh H, Wong L, Buy X, Dietemann JL, Roy C. Osteoid osteoma: percutaneous laser ablation and follow-up in 114 patients. Radiology 2007; 242:293-301.
37 Sans N, Galy-Fourcade D, Assoun J, et al. Osteoid osteoma: CT-guided percutaneous resection and follow-up in 38 patients. Radiology 1999; 212:687-692.