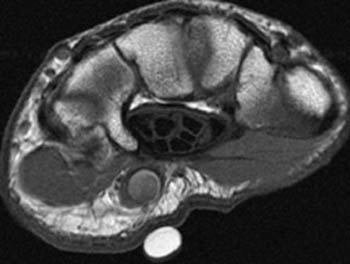
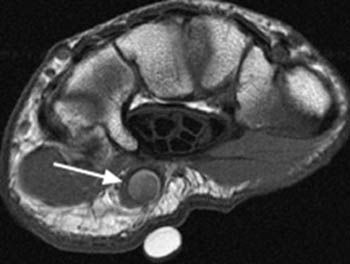
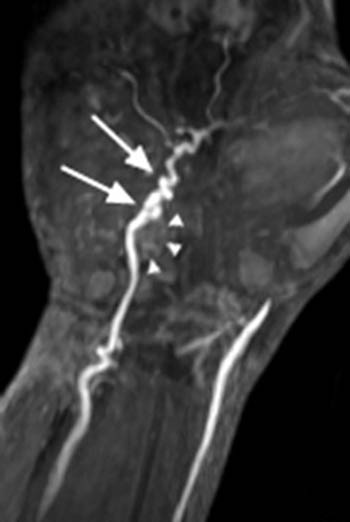
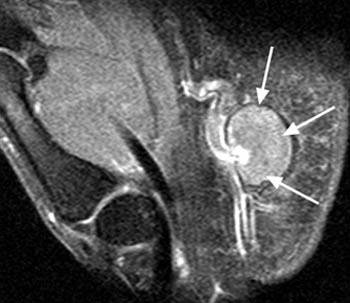
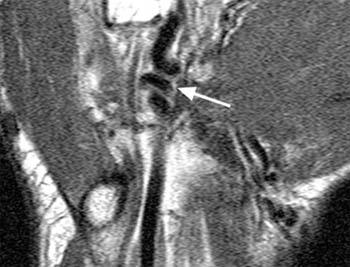
Clinical History: A 35 year old male carpenter presents with pain in the hypothenar region of the right hand and ischemia in the third, fourth and fifth fingers. (1a) An axial T1-weighted image and (1b) a coronal plane maximal intensity projection (MIP) image from a contrast enhanced MRA are provided. What are the findings” What is the diagnosis?
Findings
Diagnosis
Hypothenar hammer syndrome with a thrombosed ulnar artery aneurysm and the pathognomonic “corkscrew” appearance of the superficial ulnar artery.
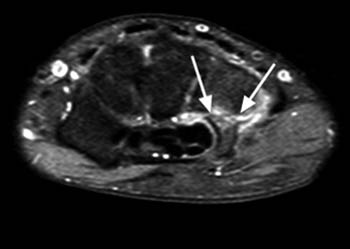
The thrombosed aneurysm and the diseased portion of the ulnar artery were subsequently resected (4a). An interposition vein graft was placed between the distal ulnar artery and the superficial palmar arch.
Introduction
The term Hypothenar Hammer Syndrome (HHS) refers to the spectrum of abnormalities resulting in damage to the superficial palmar arch of the ulnar artery. The clinical syndrome is hallmarked by unilateral finger ischemia caused by digital artery occlusions from ulnar artery emboli, and is associated with repetitive striking of the palm.1-7
Anatomy
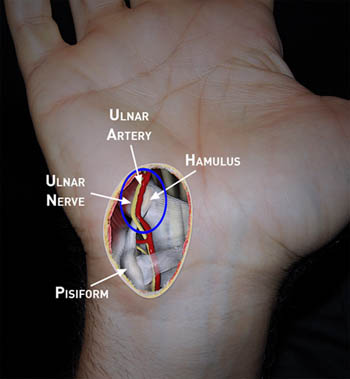
In HHS, the ulnar artery is damaged over a 2 cm segment just distal to Guyon’s canal before penetrating the palmar aponeurosis. This arterial segment is susceptible to injury because of its superficial position and resultant limited protection from overlying soft tissues.1 With palmar trauma, the at-risk ulnar artery segment is compressed against the adjacent hamulus and has been compared to a hammer-on-anvil phenomenum. The relationship of the ulnar artery to the hamulus is variable but most commonly, the artery is located just lateral to the hamulus.8
The arterial anatomy of the hand is variable. The deep and superficial palmar arches provide the arterial supply to the digits. Typically, the ulnar artery has a deep palmar branch that usually arises proximal to the level of the hamulus and communicates with the deep palmar arch. Distal to the deep palmar branch, the superficial ulnar artery typically continues to the superficial palmar arch. A complete palmar arch where the ulnar side of the superficial palmar arch anastomoses to the superficial palmar side of the radial artery is found in only 10% of patients.9 A variable number of ulnar veins follow the course of the ulnar artery and are typically seen medial and lateral to the artery.
The ulnar nerve is usually located medial to the hamulus but this relationship is variable. Within Guyon’s canal, the ulnar nerve bifurcates into the superficial branch (which contains superficial sensory branches and innervates the palmaris brevis muscle) and the deep branch (a motor nerve).8
Clinical Presentation
HHS most commonly occurs in the dominant hand of men, with a mean age of 40 years. HHS has been associated with different occupations and sports.1,3,4,6,7 HHS can occur in any occupation where the worker uses the hypothenar portion of the hand as a tool to hammer, push or squeeze hard objects. Workers at risk include metal workers, auto mechanics, lathe operators, machinists, miners, sawmill workers, butchers, bakers, brick layers and carpenters.1,3,4,6,7 HHS has been associated with numerous sports including handball, baseball, tennis, squash, martial arts, break dancing, and golf.6
The clinical presentation of HHS can range from an abrupt presentation after injury to intermittent signs and symptoms that are temporally remote from the injury.1,3,4,6,7 The ischemia involves the second, third, fourth or fifth digits of the dominant hand. Other complaints can include digital pain with paresthesias, cold sensitivity, phasic blanching or discoloration of the fingertips, finger claudication, hypothenar pain and Raynaud’s phenomenon.
In HHS, findings on physical examination include hypothenar callus and tenderness, a postive Allen test (test for ulnar artery patency by occluding radial and ulnar arteries and then releasing ulnar artery pressure), pulsatile hypothenar mass in the case of aneurysm formation, and unilateral episodic blanching or purplish discoloration of the second, third, fourth or fifth fingertips. In severe cases, gangrene, ulceration or eschar formation of the involved fingertips may occur.3,5,7
In one large series, 45% of patients with HHS presented with digital ischemia and necrosis and 23% presented with symptoms referable to the sensory branch of the ulnar nerve. Abnormalities of the ulnar artery included occlusion (60%), aneurysm (40%) and embolic occlusions of the digital arteries ( 57%).5 Compression of the sensory branches of the ulnar nerve occur because of the close proximity to the ulnar artery, with resultant neurologic symptoms including paresthesias and pain.1
HHS should be suspected when a patient with vascular ischemia involving the digits presents without an underlying medical problem. It has been suggested that regular screening of hands by occupational health services in individuals with high risk jobs should be considered.7
Imaging of HHS
The initial imaging of patients with problems in the hypothenar region begins with routine radiography. The routine radiographic views should include posteroanterior, lateral and carpal tunnel views. Other views that may be helpful include semisupinated oblique view and a lateral view with the hand radially deviated and the thumb abducted.8 Routine radiography can diagnose osseous abnormalities such as hamulus fractures and arthropathies.
The next imaging study could be Duplex sonography, CT/CTA, MR/MRA or catheter angiography. The best choice depends on local expertise, the suspected clinical diagnosis and the preferences of the local hand surgeons.
Duplex sonography, in the appropriate hands, can be an excellent method to screen the ulnar artery for patency and aneurysm formation. Duplex sonography is inexpensive and non-invasive.10 The technique requires expertise and is operator dependent. The field of view is limited and it is difficult to use for surgical mapping. The exam is best considered a screening tool for HHS.
MR and MRA (MR angiography) provide a comprehensive evaluation of the hypothenar region. MR imaging can be used to evaluate osteochondral, neural, vascular, tendinous and ligamentous structures. MRA can be added to the MR examination to provide more detailed information regarding the vasculature of the hand in patients with HHS.4,11 MR imaging has the potential to detect early changes of arterial wall thickening and edema perhaps before angiographic abnormalities are present, and often demonstrates aneurysms to good advantage (6a). The corkscrew appearance of the ulnar artery as it leaves Guyon’s canal is often well seen even with non-contrasted routine MR images (7a). MRA is capable of demonstrating the site of segmental occlusion of the ulnar artery as well as the abnormal areas of the superficial palmar arch and common volar digital arteries. Collateral vessels and embolic disease can be clearly identified with MRA. Although the spatial resolution of MRA is inferior to catheter angiography, many hand surgeons find the MRA examinations to be adequate for surgical planning. MRA examinations are typically performed with Gadolinium contrast.
CT and CTA (CT angiography) also provide a comprehensive evaluation of the hypothenar region.8 CT can be used to evaluate osseous structures and as a rule has superior spatial resolution compared to MR imaging. The contrast resolution of CT, however, is inferior to MR. Soft tissue edema, masses, tendons, ligament, nerves and vascular structures are better evaluated with MR. CTA is an excellent way to evaluate pathology of the ulnar artery. CTA examinations are technically less demanding than MRA and the spatial resolution is typically superior to MRA. The distal radial and ulnar arteries, the palmar arches, and the first few centimeters of the digital arteries can be visualized with CTA.8 CTA examinations require radiation and iodinated contrast.
Some still consider the “gold standard” for the diagnosis of HHS is conventional angiography.3,7 They believe the aortic arch and the entire upper extremity should be evaluated in these patients to exclude diagnoses other than HHS. Additionally, conventional angiography has superior spatial resolution compared to CTA and MRA. This is particularly important with the smaller hand and digital vessels where conventional angiography will provide superior and important anatomic detail.
Regardless of the imaging technique, the pathognomonic angiographic features of HHS are alternating areas of stenosis and ectasia with elongation and tortuosity of the ulnar artery causing a “corkscrew” appearance. Less commonly, aneurysm formation of the ulnar artery is present. Other findings include occlusion of the ulnar artery segment overlying the hook of the hamate, occluded digital arteries in an ulnar artery distribution, and demonstration of intraluminal emboli at sites of digital obstruction.3,7
Treatment
The treatment of HHS is controversial. Most patients will be treated conservatively if there is adequate collateral circulation. Conservative therapy includes smoking cessation, avoidance of further trauma, padded protective gloves, cold avoidance, calcium channel blockers, hemodilution, antiplatelet agents, anticoagulation, thrombolysis, wound care of fingers with necrosis, and pentoxifylline to reduce blood viscosity.1-3,5-7 Patients treated conservatively need to be followed closely. In one series of 47 patients with HHS, only two patients initially required surgery. The relapse rate, however, was 28%.5
Proponents of surgical treatment cite several rationales for surgery including removal of a source of embolism, removal of a painful mass, relief of ulnar nerve compression, and creation of a local periarterial sympathectomy.7 The type of surgical procedure will depend on the degree of vascular insult and local surgical preferences. If the radial/palmar arch is intact, then a simple arterial ligation can be performed. A second surgical method is resection of thrombosed arterial segment or aneurysm with an end-to-end anastomosis. A third surgical option would be resection and vascular reconstruction with vein or artery graft.7
Pathologic Findings
Pathologically, findings include intimal hyperplasia, and duplication and fragmentation of the internal elastic lamina. Arterial wall damage predisposes to aneurysm formation, vessel thrombosis and microemboli formation.3,7,12 With advanced thrombosis, involvement of the adventitia may affect periarterial sympathetic fibers, resulting in reflex vasospasm and thus further decreasing the surrounding collateral circulation.6
Abnormalities of the at risk segment of the distal ulnar artery are present in asymptomatic patients, and may be detected on MR scanning of the wrist for other reasons (E). In a study of 21 randomly selected autopsy specimens, intimal hyperplasia, as measured via an intima/media ratio, was significantly higher in the right hands of males compared to either the corresponding left hand or in either hand of females.12 In another study, bilateral palmar ulnar artery disease was detected in 12 of 13 patients in whom bilateral upper extremity angiography was performed.3
One study proposed that preexisting fibromuscular hyperplasia of the palmar ulnar artery exists in patients with HHS. The authors hypothesize that fibromuscular dysplasia predisposes the artery to form intraluminal thrombus from repetitive striking of the palm.3 It is uncertain why a minority of patients with HHS form unlar artery aneurysms. It has been suggested that damage to the intima would result in arterial thrombosis while damage to the media would cause aneurysmal formation.7
Differential Diagnosis
The differential diagnosis for HHS includes osteoid osteoma, benign tumors of the hand (most commonly lipomas, schwannomas, and vascular malformations), malignant tumors (less common than benign tumors), ganglion cysts, tendinopathy of the flexor carpi ulnaris tendon, arthropathy of the triquetral-pisiform articulation, fracture of the hamulus (8a), Guyon Canal syndrome, hypothenar syndrome, and anomalous musculature.8
Conclusion
HHS syndrome is caused by damage to the exposed superficial segment of the ulnar artery by either occupational or sporting activities. The diagnosis should be suspected when a younger male presents with symptoms of pain and ischemia in the dominant hand. MR and MRA can conclusively diagnose HHS by depicting arterial abnormalities including aneurysm formation and the pathognomonic “corkscrew” appearance.
References
1 Ablett CT, Hackett LA. Hypothenar hammer syndrome: case reports and brief review. Clin Med Res 2008; 6:3-8.
2 Brodmann M, Stark G, Aschauer M, et al. Hypothenar hammer syndrome caused by posttraumatic aneurysm of the ulnar artery. Wien Klin Wochenschr 2001; 113:698-700.
3 Ferris BL, Taylor LM, Jr., Oyama K, et al. Hypothenar hammer syndrome: proposed etiology. J Vasc Surg 2000; 31:104-113.
4 Jagenburg A, Goyen M, Hirschelmann R, Carstens IM, Kroger K. [Hypothenar hammer syndrome: causes, sequelae and diagnostic aspects]. Rofo 2000; 172:295-300.
5 Marie I, Herve F, Primard E, Cailleux N, Levesque H. Long-term follow-up of hypothenar hammer syndrome: a series of 47 patients. Medicine (Baltimore) 2007; 86:334-343.
6 Mueller LP, Mueller LA, Degreif J, Rommens PM. Hypothenar hammer syndrome in a golf player. A case report. Am J Sports Med 2000; 28:741-745.
7 Vayssairat M, Debure C, Cormier JM, Bruneval P, Laurian C, Juillet Y. Hypothenar hammer syndrome: seventeen cases with long-term follow-up. J Vasc Surg 1987; 5:838-843.
8 Blum AG, Zabel JP, Kohlmann R, et al. Pathologic conditions of the hypothenar eminence: evaluation with multidetector CT and MR imaging. Radiographics 2006; 26:1021-1044.
9 Ruengsakulrach P, Eizenberg N, Fahrer C, Fahrer M, Buxton BF. Surgical implications of variations in hand collateral circulation: anatomy revisited. J Thorac Cardiovasc Surg 2001; 122:682-686.
10 Genchellac H, Demir MK, Unlu E, Temizoz O, Ozdemir H. Hypothenar hammer syndrome: gray-scale and color Doppler sonographic appearances. J Clin Ultrasound 2008; 36:98-100.
11 Winterer JT, Ghanem N, Roth M, et al. Diagnosis of the hypothenar hammer syndrome by high-resolution contrast-enhanced MR angiography. Eur Radiol 2002; 12:2457-2462.
12 Stone JR. Intimal hyperplasia in the distal ulnar artery; Influence of gender and implications for the hypothenar hammer syndrome. Cardiovasc Pathol 2004; 13:20-25.