Clinical History:
A 43 year-old male presents with pain for 3 days after injury. He is experiencing forearm cramping and is unable to extend his thumb.
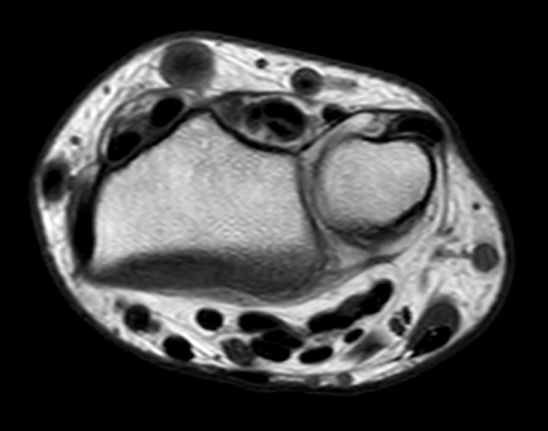
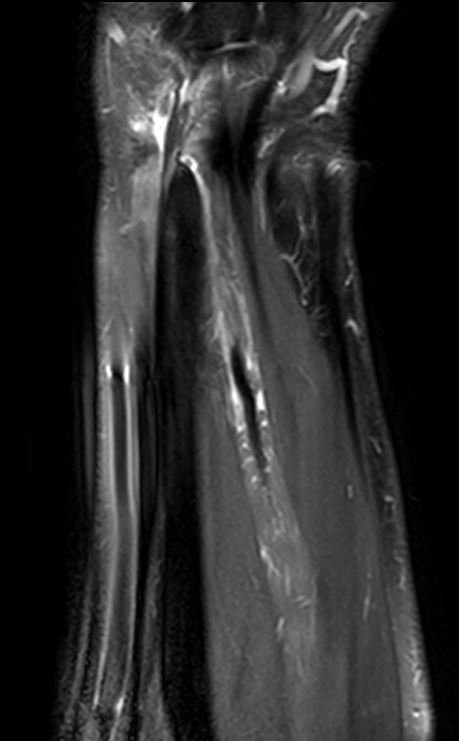
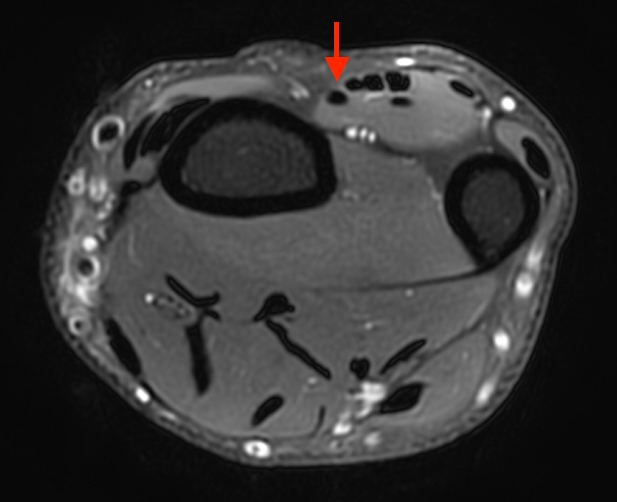
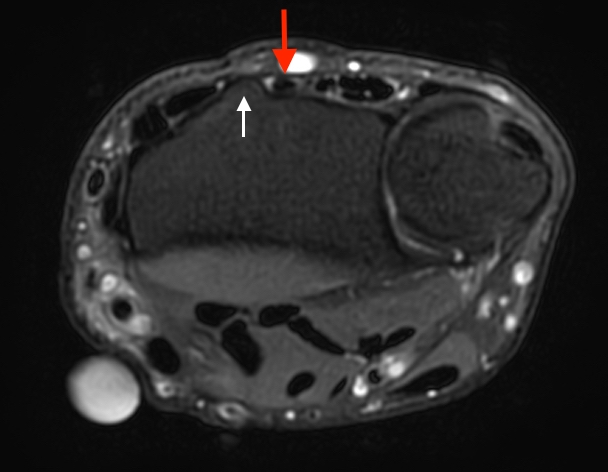
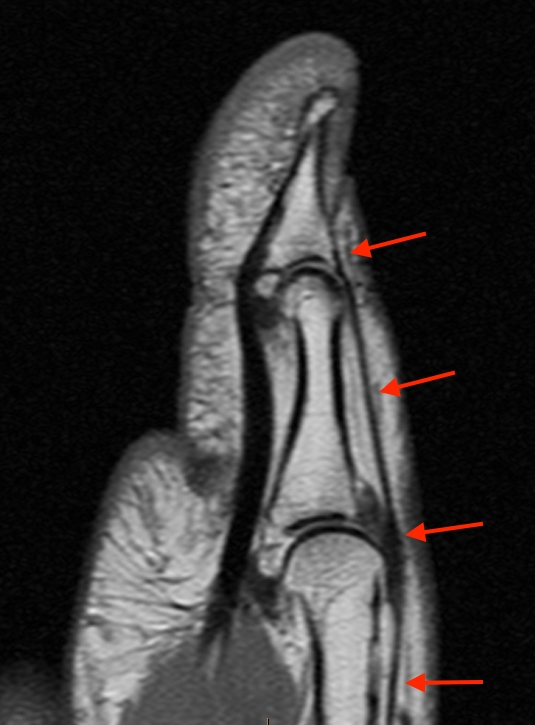
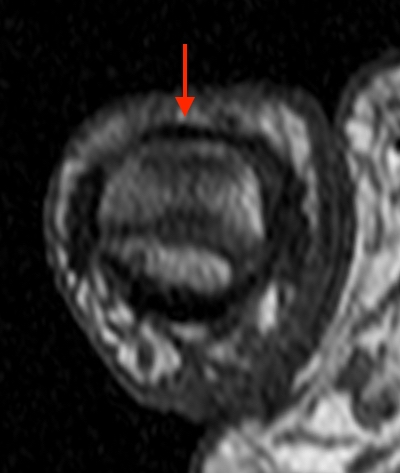
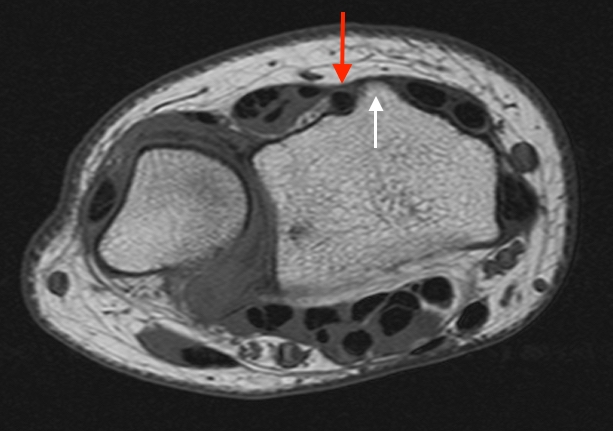
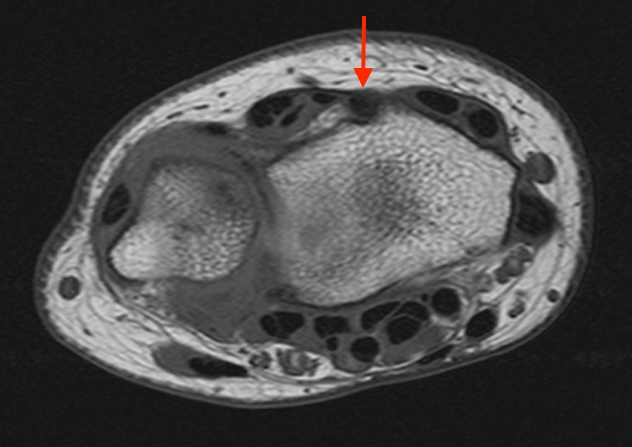
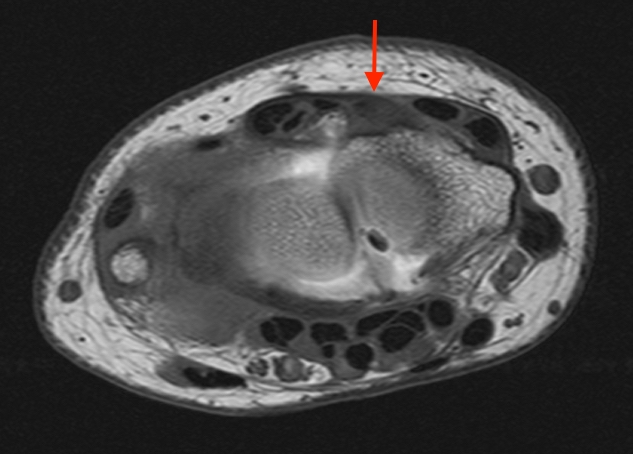
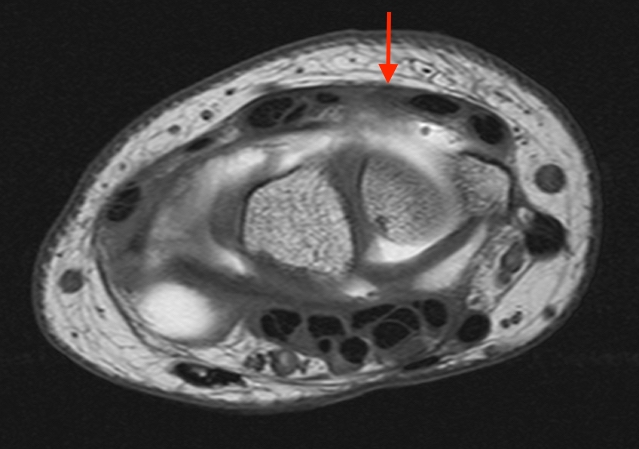
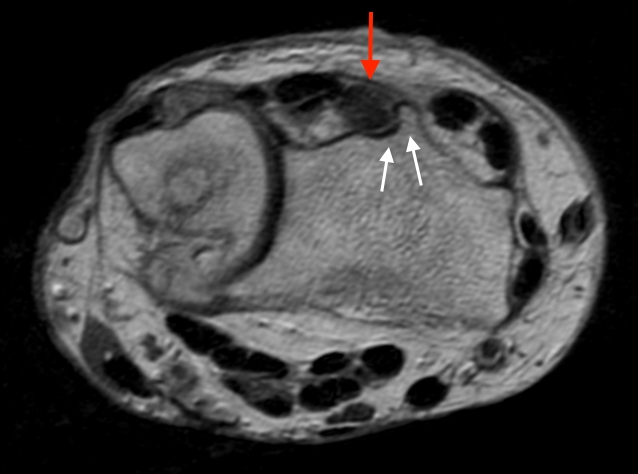
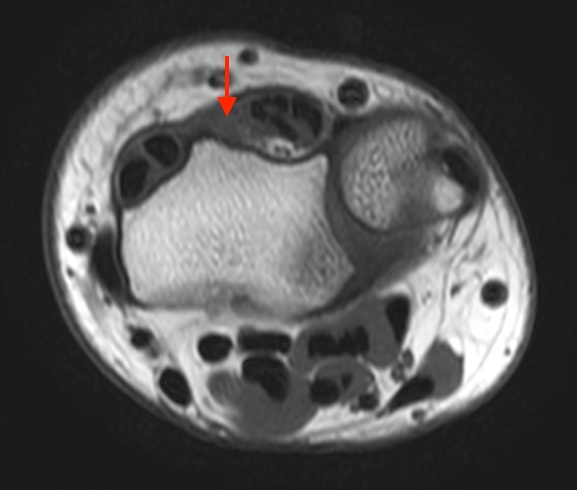
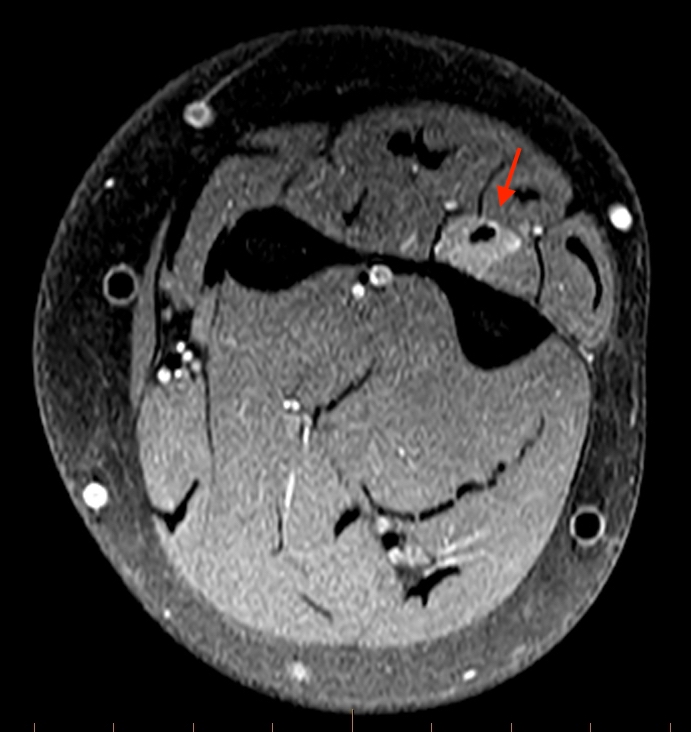
T1-weighted (1a) and fat-suppressed proton density-weighted (1b) axial images as well as sequential fat-suppressed proton density-weighted coronal images (1c,d) are provided.
Findings
Figure 2:
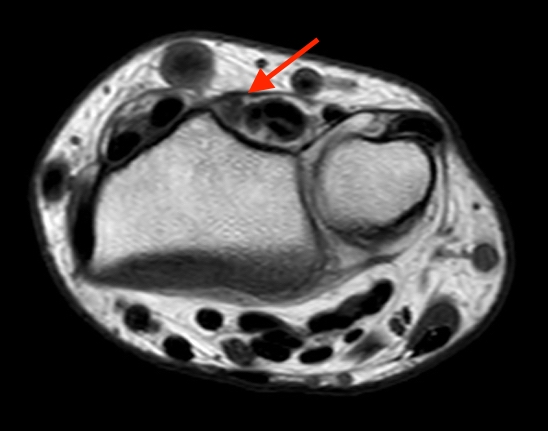
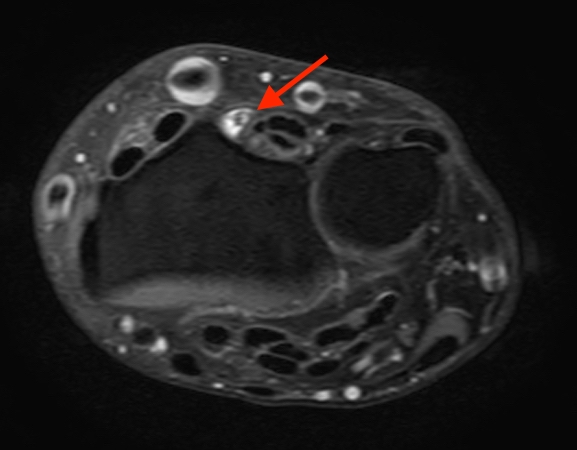
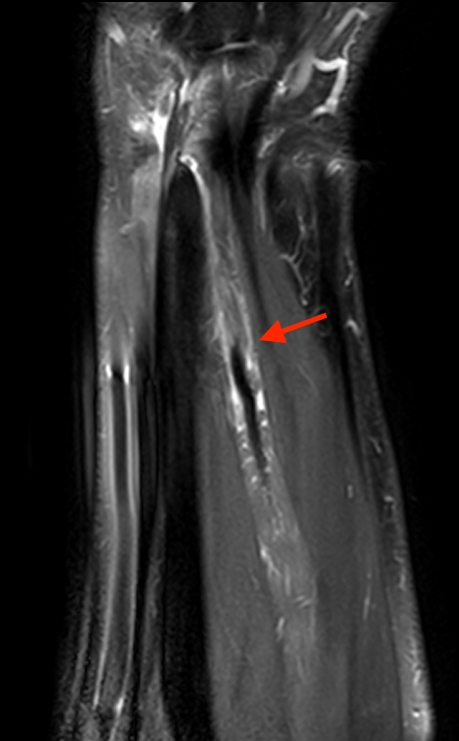
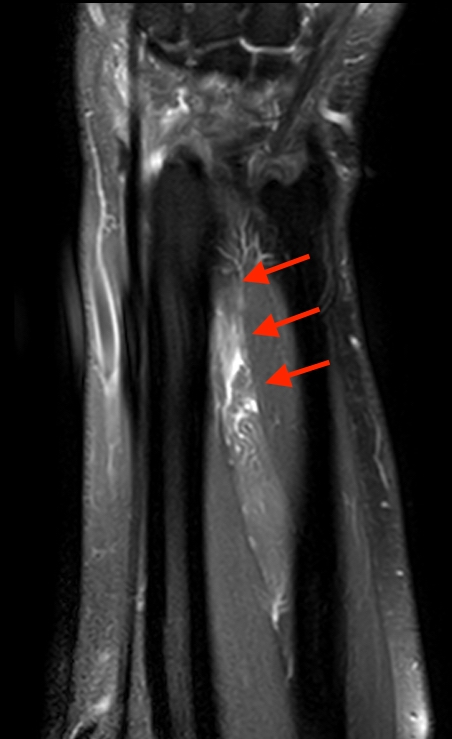
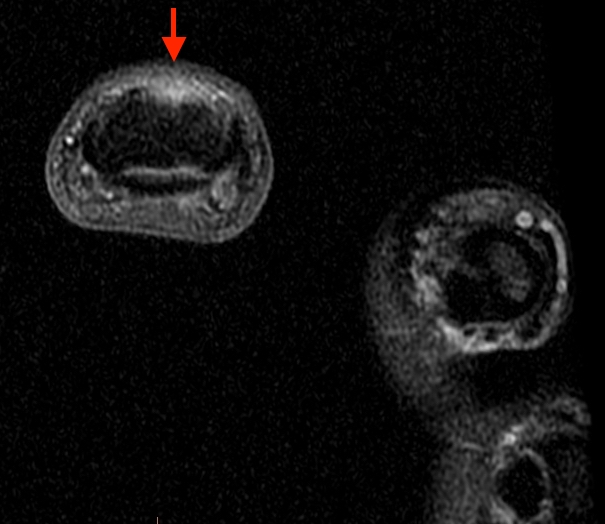
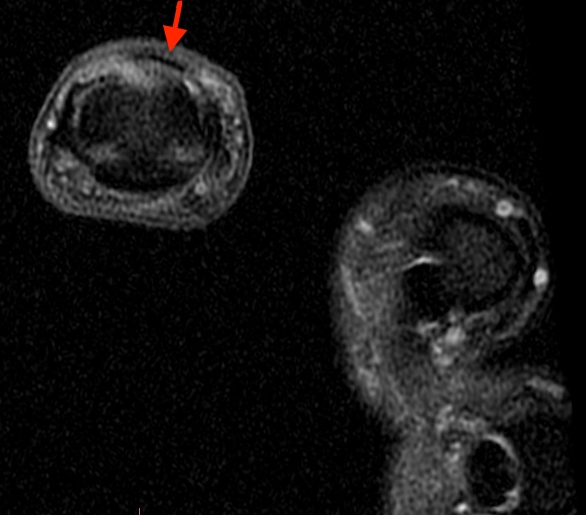
2a-b: Axial T1-weighted and axial fat-suppressed proton density-weighted images at the level of Lister’s tubercle demonstrate a completely disrupted extensor pollicis (EPL) tendon, with a fluid filled cleft at the rupture site (arrow).
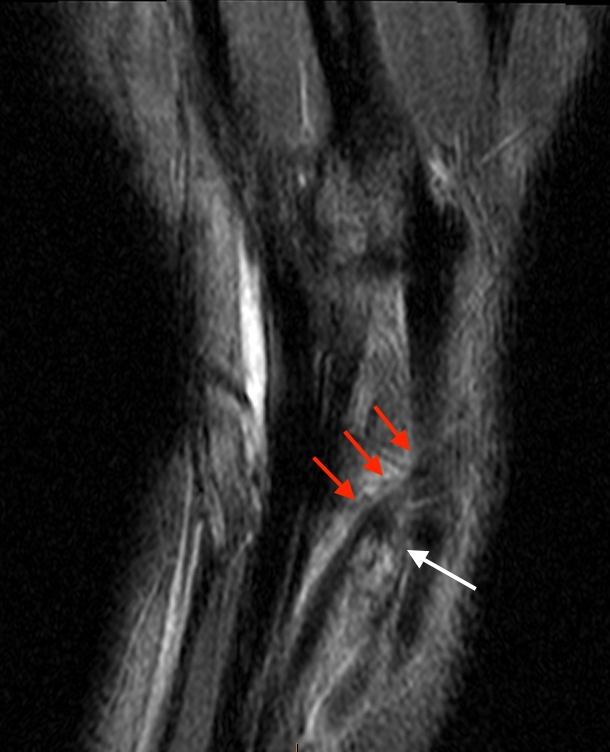
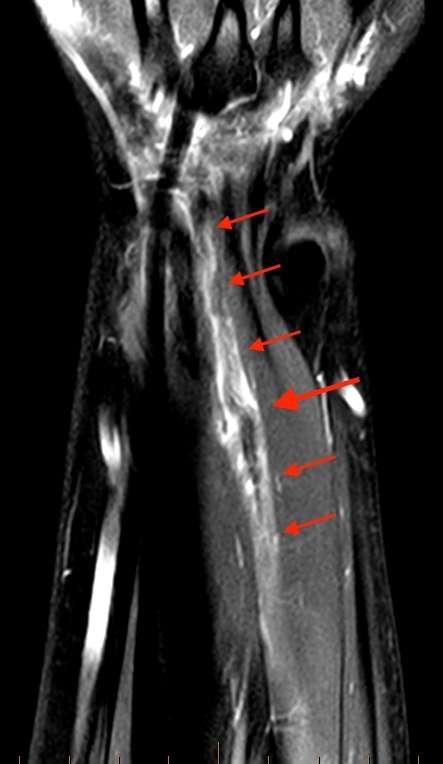
2c-d: Coronal fat-suppressed proton density weighted images demonstrate the proximally retracted torn EPL tendon (2c arrow), with fluid along the rupture tract extending towards the retracted EPL muscle (2d arrows).
Diagnosis
Extensor pollicis longus (EPL) tendon rupture at the level of Lister’s tubercle.
Introduction
The extensor pollicis longus (EPL) tendon resides within the 3rd dorsal extensor compartment of the wrist, inserts upon the distal phalanx of the thumb, and is the primary extensor of the thumb. The tendon most commonly ruptures near Lister’s tubercle in association with distal radial fractures, but can also rupture spontaneously. This web clinic reviews the anatomy, pathology, MRI appearance, and treatment of EPL tears.
Anatomy
The EPL origin lies along the mid dorsal surface of the ulna and along the interosseous membrane, crossing the forearm in an oblique fashion, extending towards the radial aspect of the wrist.1 At the level of the distal radius, the EPL tendon is located just ulnar to Lister’s tubercle, within the 3rd dorsal compartment of the wrist, and is covered by the extensor retinaculum, as are the remaining dorsal extensor tendons. At this level, the extensor tendons are lined by a synovial sheath, which promotes smooth gliding motion. Distal to Lister’s tubercle, the EPL continues obliquely towards the thumb, crossing superficially over the 2nd extensor compartment tendons (extensor carpi radialis longus, extensor carpi radialis brevis).2 Along with the extensor pollicis brevis, the EPL creates the triangular “anatomical snuffbox” near the level of the scaphoid. Finally, the EPL inserts at the dorsal base of the thumb distal phalanx. The EPL muscle is innervated by the posterior interosseous nerve and serves to extend the thumb distal phalanx at the CMC and IP joints.1 The cross-sectional area of a muscle is proportional to its generated force, while the length is proportional to its excursion and speed of contraction. With long thin muscles, the extrinsic finger extensor muscles are better suited for excursion and speed rather than force.2
Figure 3:
Normal anatomy.
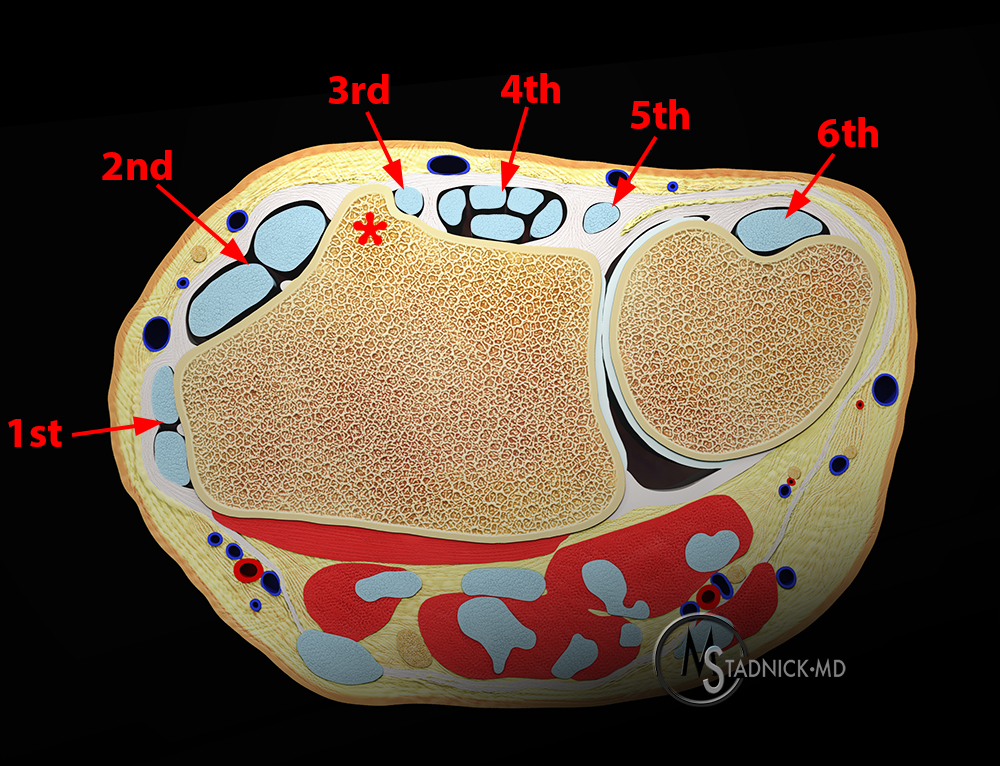
3a: Anatomic rendering at the level of Lister’s tubercle demonstrates the 6 dorsal extensor tendon compartments. The EPL resides within the 3rd compartment, at the ulnar aspect of Lister’s tubercle (asterisk).
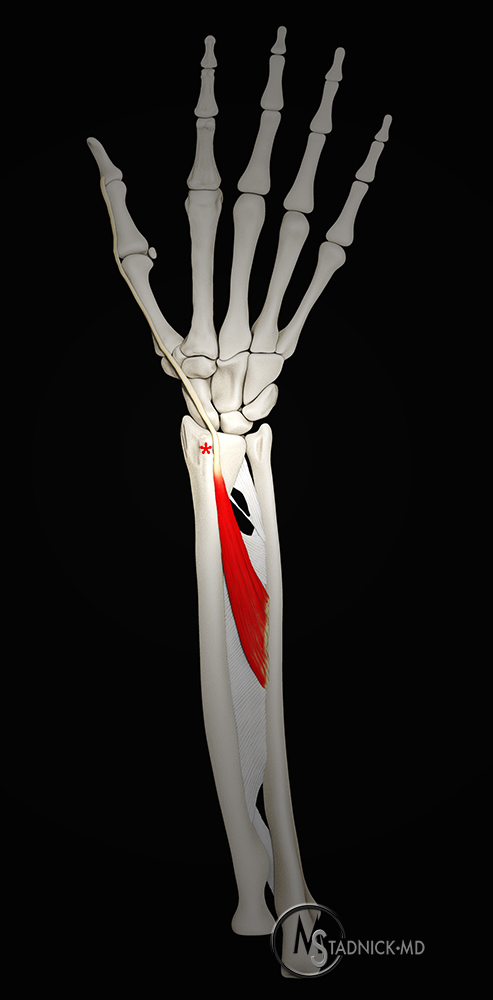
3b: Anatomic rendering demonstrates the normal course of the EPL muscle and tendon, originating at the mid dorsal ulna and interosseous membrane, crossing obliquely along the dorsal radius at the ulnar aspect of Lister’s tubercle (asterisk), inserting upon the thumb distal phalangeal base.
On MR imaging, the EPL tendon is best evaluated on axial series. The dorsal convexity of Lister’s tubercle creates a characteristic bony landmark along the distal radius (figure 4b). Once Lister’s tubercle is identified, the EPL tendon should be visualized just ulnar (medial) to the tubercle. Because the EPL diameter is often smaller than the remaining tendons, subtle pathology of this tendon can be missed unless the tendon is scrutinized. Furthermore, the EPL tendon is also prone to magic angle artifact (non-pathologic signal on low TE sequences, in tendons oriented 55 decrees to the MRI bore), due to its oblique orientation distal to Lister’s tubercle3 (figure 5). Typically, the magic angle effects occur just distal to Lister’s tubercle, as the EPL tendon begins to cross over the second compartment tendons, and the tendon regains homogeneous low signal as it continues distally towards the thumb insertion.
Figure 4:
Normal MR anatomy.
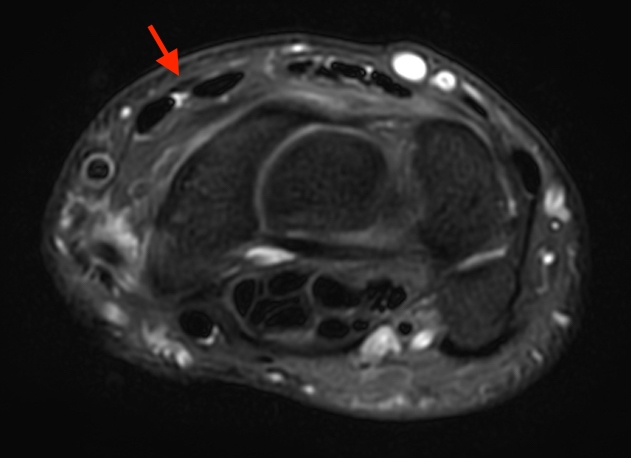
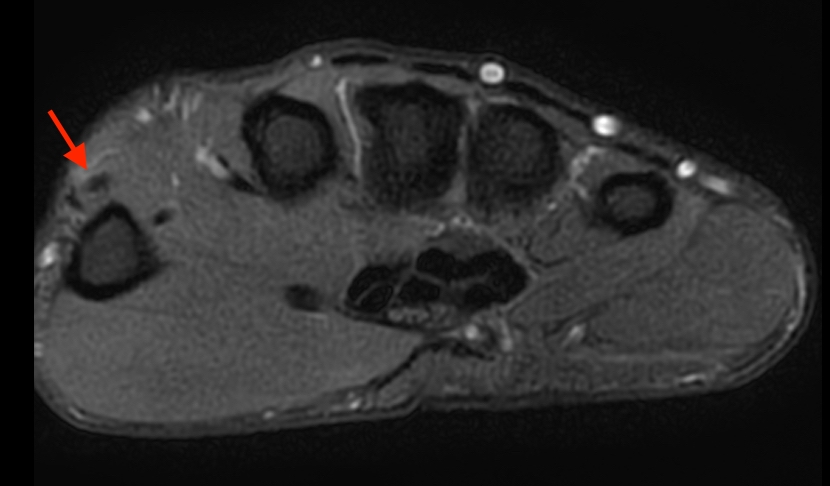
4a-e: Progressive axial fat-suppressed proton density-weighted images extending from the distal forearm into the proximal hand demonstrate the normal oblique course of the EPL tendon (red arrows). The tendon is normally identified along the ulnar aspect of Lister’s tubercle (4b white arrow), continuing along the dorsal aspect of the second extensor compartment tendons (4c-d) towards the thumb insertion.
4f-g: Sagittal proton density-weighted and inversion recovery images through the thumb demonstrate the normal course of the distal EPL tendon, inserting upon the distal phalangeal base.
4h: Axial T1-weighted image near the level of the thumb proximal phalangeal head demonstrates the normal distal EPL tendon, just proximal to the insertion.
Figure 5:
“Magic angle” artifact.
Progressive axial T1-weighted images (TE 8.6, TR 681) of a normal EPL tendon, following intra-articular contrast injection.
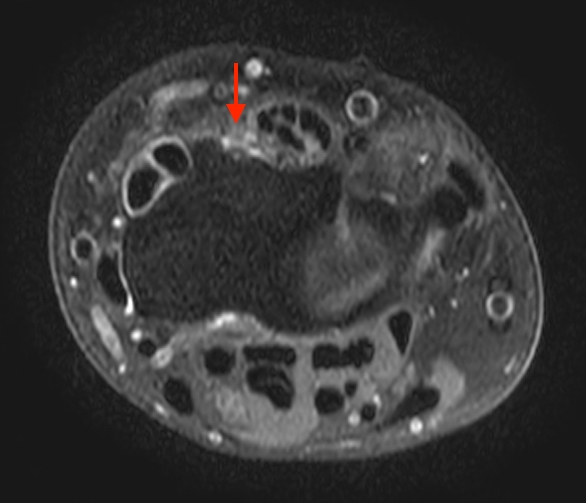
5a: At the level of Lister’s tubercle (white arrow) the EPL (red arrow) demonstrates normal low signal intensity, similar to the other tendons.
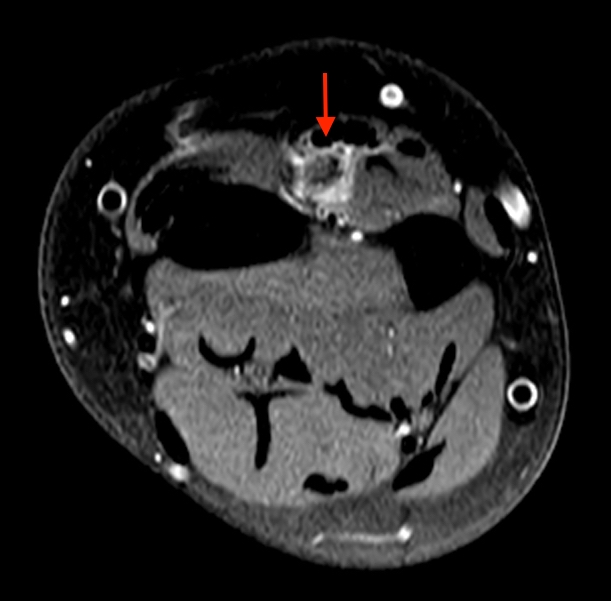
5b-d: Distal to Lister’s tubercle, the normal EPL tendon (red arrows) demonstrates increased signal as the tendon courses obliquely, approximating 55 degrees to the MRI bore. Note this occurs with low TEs (T1 and proton density-weighted images), and is less pronounced with longer TEs (T2 weighted images). Alternative positioning of the patient can also mitigate this artifact.
Pathology
Rupture of the EPL tendon is most commonly associated with fractures of the distal radius (figure 6), with a reported incidence of 0.2-5%4,5, and typically occurring 6-8 weeks after the fracture.6 Interestingly, EPL tendon ruptures are more commonly associated with nondisplaced distal radial fractures rather than displaced fractures.5 EPL tendon ruptures may also occur spontaneously with risk factors including underlying chronic inflammation (such as rheumatoid arthritis or lupus), prior local or systemic steroid injections, and chronic repetitive motion of the wrist.5,7,8,9
EPL ruptures typically occur beneath the extensor retinaculum, at Lister’s tubercle.5, 10 Lister’s tubercle acts as a pulley for the tendon and can be a source of mechanical irritation, particularly if irregularities of the dorsal cortex are present (figure 7). Physical exam correspondingly demonstrates loss of thumb extension at both the MP and IP joints (potentially with weak residual MP joint extension remaining due to assistance of the extensor pollicis brevis).
Figure 6:
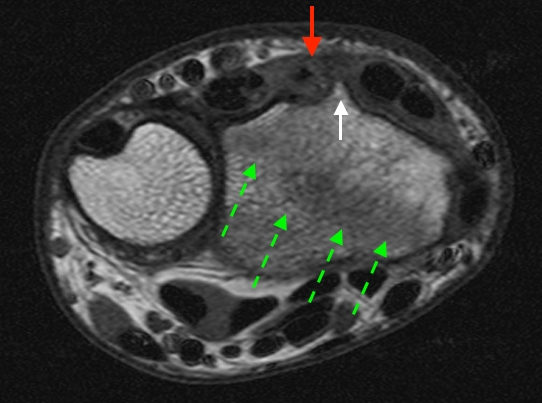
Distal radial fracture with partial EPL tendon tear.
6a-b: Axial T1-weighted (6a) and fat-suppressed proton density-weighted (6b) images at the level of Lister’s tubercle (white arrow) demonstrate a nondisplaced distal radial fracture (green arrows). The EPL tendon is irregular and fragmented (red arrows), consistent with high grade partial tearing.
6c: Coronal inversion recovery image demonstrates the course of the partially torn EPL tendon (red arrows) near Lister’s tubercle (white arrow).
Two major theories (mechanical and vascular) describe the pathophysiology of spontaneous EPL tendon ruptures. According to the mechanical theory, the EPL tendon is closely approximated along the dorsum of the distal radius near Lister’s tubercle. Dorsal cortical irregularities (figure 7) from fractures or osteophytes can abrade the tendon, resulting in attrition and eventual disruption. The extensor retinaculum keeps the EPL tendon closely approximated to the distal radius, and is thought to contribute to mechanical irritation.5,8 According to the vascular theory, a relatively avascular zone exists within the EPL tendon near Lister’s tubercle, with tendon sustenance in this zone primarily occurring via diffusion from the tendon sheath. Hematomas within the tendon sheath increase pressure and interfere with the production of synovial fluid, causing relative localized ischemia within this segment of the EPL tendon and risk for rupture.5,6,8,11,12
Figure 7:
EPL tendinosis and irregular tubercle.
7 a-b: Axial proton density-weighted images near the level of Lister’s tubercle demonstrate an irregular pedunculated appearance of the tubercle with notching of the adjacent cortical bone (white arrows). The EPL tendon is abnormally thickened with intermediate signal, consistent with tendinosis.
On MRI, Acute complete tears of the EPL tendon are the easiest to identify, as they are typically accompanied by bright tenosynovial fluid surrounding a retracted tendon. On axial images, a circular defect of absent tendon is seen adjacent to Lister’s tubercle within the 3rd extensor compartment, akin to the appearance of the empty intertubercular groove seen on axial imaging with proximal long head biceps tendon ruptures. Coronal and sagittal images are useful for confirming and measuring tendon retraction. Chronic tears are easier to overlook, since there is usually little fluid or edema and because of the small caliber of the tendon. Tendinosis and partial tears of the EPL can be more challenging to diagnose as they may be confused with magic angle artifacts. In our experience, artifacts typically occur distal to Lister’s tubercle while the tears typically occur at Lister’s tubercle. If desired, obtaining long TE axial sequences or alternating wrist positioning can be performed to differentiate magic angle artifact from interstitial EPL tendon pathology. A differential consideration for absent/decreased thumb extension includes posterior interosseous nerve (PIN) injury, and can also be evaluated with MRI.
Figure 8:
EPL rupture near Lister’s tubercle – additional example.
8a-b: Axial T1-weighted and axial fat-suppressed proton density-weighted images at the level of Lister’s tubercle demonstrate a completely disrupted EPL tendon, with a fluid filled cleft at the rupture site (arrow).
8c-d: Axial fat-suppressed proton density-weighted images within the forearm demonstrate edema within and surrounding the EPL muscle (arrows).
8e: Coronal fat-suppressed proton density-weighted image demonstrates fluid and edema along the retracted rupture tract, extending toward the EPL muscle (arrows). The retracted torn EPL tendon stump is denoted with the larger arrow.
Treatment
Direct end-to-end repair of an EPL rupture is often difficult as the ruptured ends are usually fragile and frayed. After removing the unhealthy portion of the tendon, a tendon gap typically remains.5,10 Therefore, tendon grafting or transfer has become standard treatment.5 For grafting, palmaris longus tendon may be used to bridge a gap between the tendon disruption10. For tendon transfer, the extensor indicis proprius (EIP) is typically used5 as it has a similar amplitude and direction of pull to the EPL, and provides a predictable outcome.10 Proper tensioning is important to maintain adequate range of motion, and to balance the forces against the much stronger flexor pollicis longus.10
Figure 9:
EPL repair using palmaris longus graft.
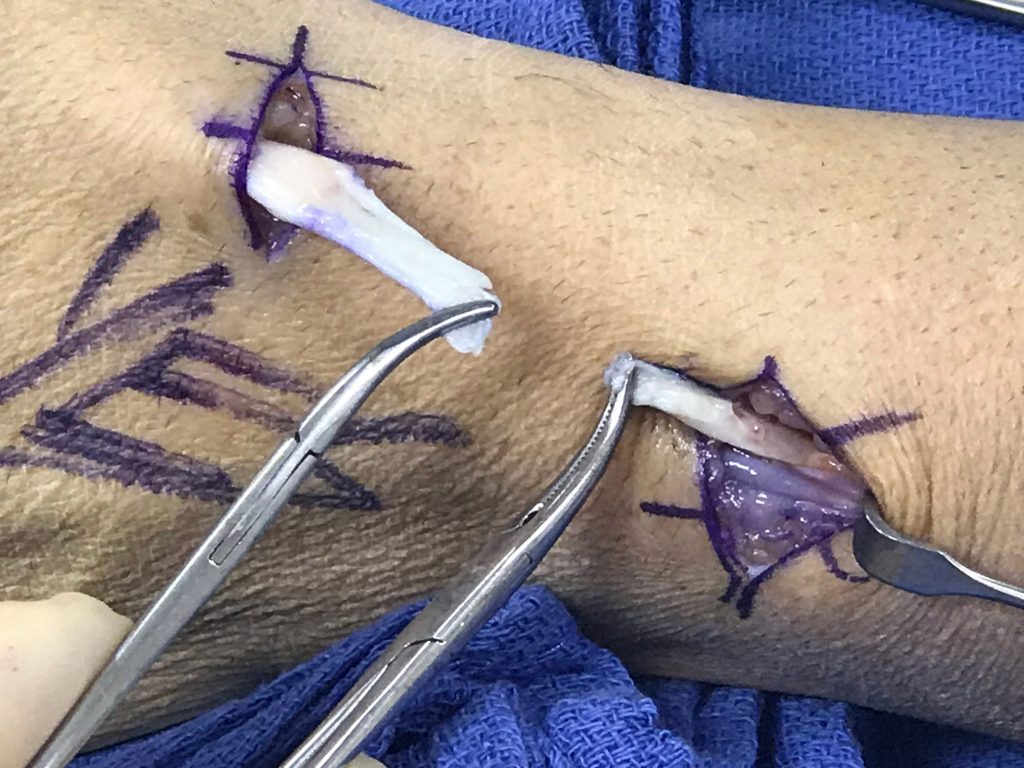
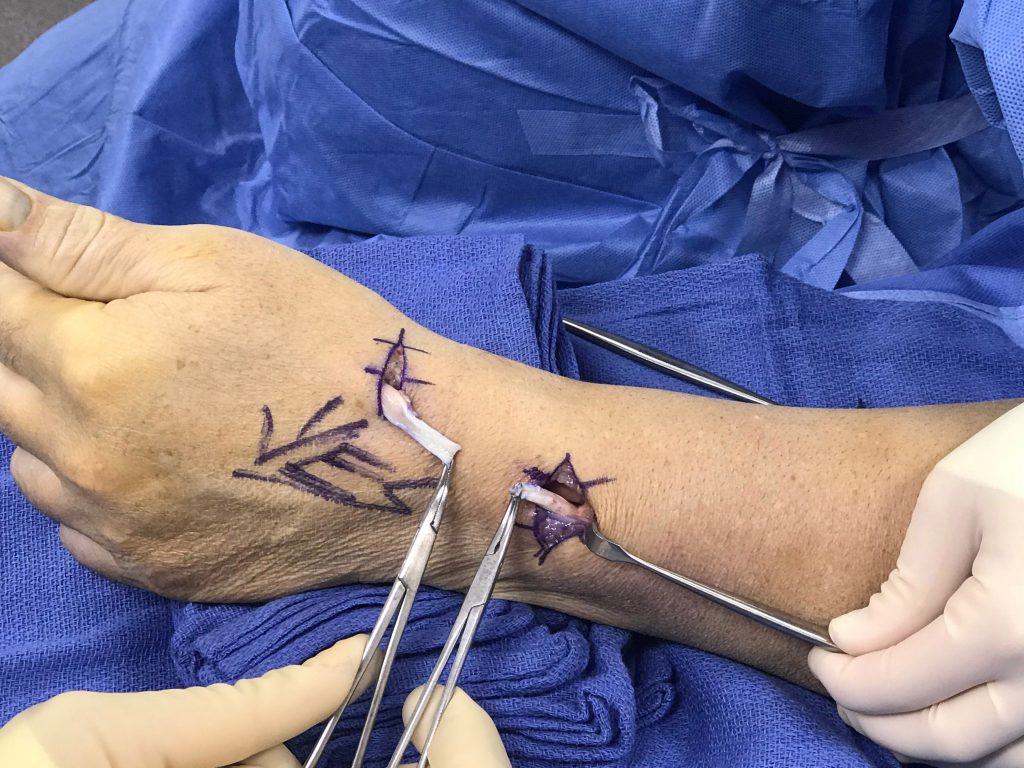
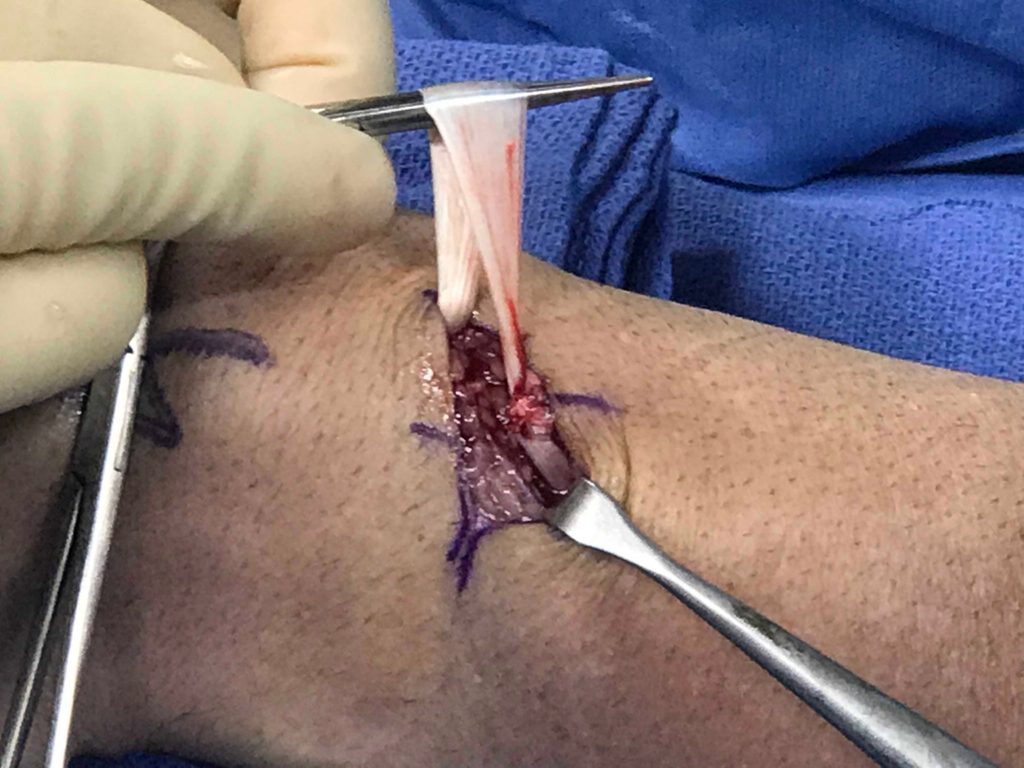
9a-b: Intraoperative photos of our initial unknown case (figures 1-2) confirm complete rupture of the EPL tendon near Lister’s tubercle. The preoperative MRI was used to plan precise small incisions and retrieve the proximal and distal torn tendon stumps (held by forceps).
9c: Intraoperative photo demonstrates the repaired EPL proximal tenorrhaphy site. In this case, palmaris longus graft was used to repair the EPL.
Photographs courtesy of Tom Dovan, MD
Elite Sports Medicine and Orthopaedics
Nashville, TN
Distal EPL Injury – Mallet Thumb
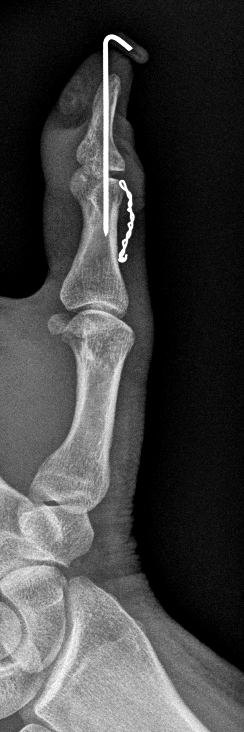
A much less common variation of EPL disruption occurs more distally at the thumb distal phalangeal insertion, also known as “mallet thumb”, originally described by Din and Maggitt in 1983.13 Patients typically report a traumatic injury distal to the thumb MP joint, tenderness near the EPL insertion, and a flexion deformity at the thumb IP joint. Radiography may demonstrate an avulsion fracture at the distal phalanx, but this is not consistently present or visible. With the ability to directly visualize tendinous disruption, tendon retraction, and bony injury, MRI has proven useful in the diagnosis and treatment planning of mallet thumb14 (figures 10a-c). Both surgical (primary suture repair with Kirchner wire immobilization of the IP joint – figure 10d)13,15 and conservative treatment (splinting in extension)16 have been advocated in the literature, with surgery recommended in cases involving greater tendon retraction.14,15
Figure 10:
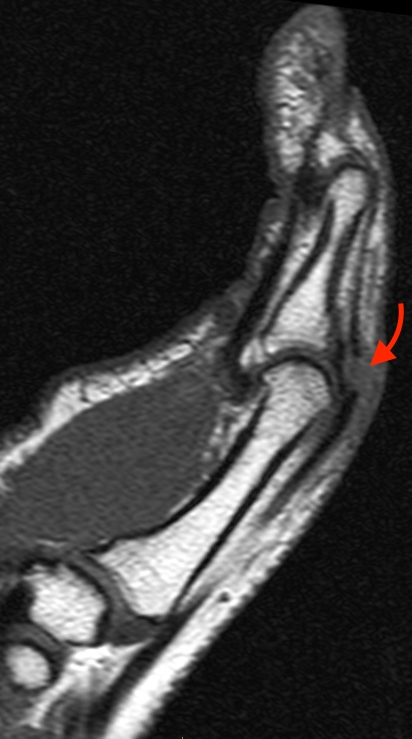
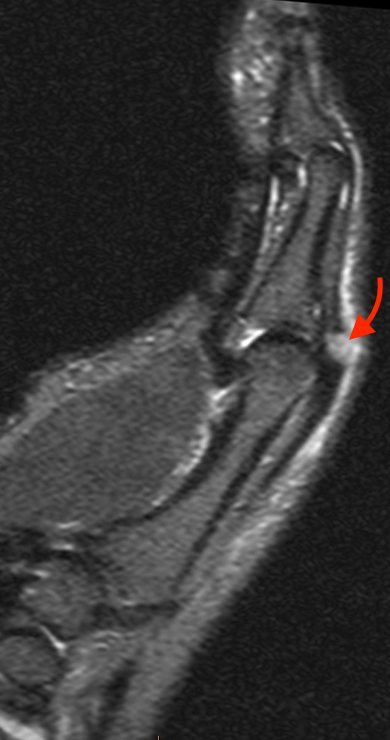
Mallet thumb.
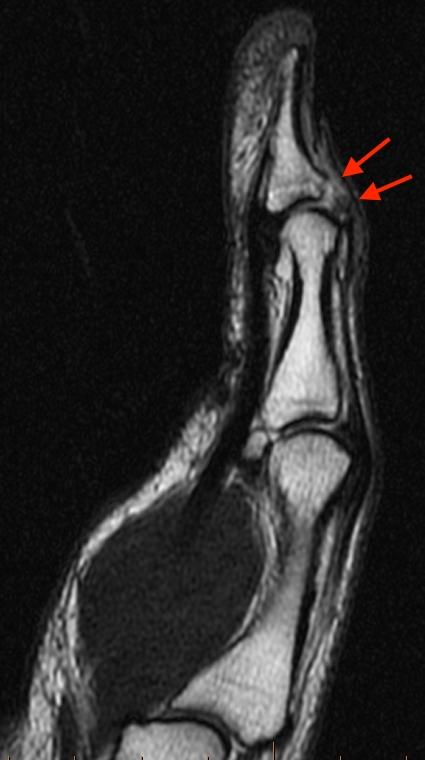
10a: Sagittal T2-weighted image demonstrates a disrupted EPL tendon insertion at the thumb distal phalangeal base, with a tiny cortical avulsion (arrows).
10b-c: Axial fat-suppressed proton density-weighted images near the level of the thumb distal phalangeal base demonstrate an edematous gap (9b arrow) at the EPL insertion site, with retracted tendon noted within the adjacent more proximal slice (9c arrow).
10d: Lateral radiograph of the same patient, obtained post-operatively following mallet thumb repair. Kirchner wire immobilization was performed.
Direct lacerations may also be a cause of distal EPL disruption, and can be preoperatively demonstrated with MRI (figure 11).
Summary
EPL tears most commonly occur at Lister’s tubercle. Tears typically occur as a delayed complication of a non-displaced distal radial fracture, but may also occur spontaneously. Much less commonly, EPL tears may occur at the distal phalangeal insertion or at a site of laceration. In the setting of lost/decreased thumb extension, MRI can evaluate the integrity of the EPL, provide measurements of tendon retraction for preoperative incision planning, and also evaluate for alternative etiologies such as posterior interosseous nerve impingement.
References
- Platzer W. Color Atlas of Human Anatomy, Vol.1: Locomotor System. 6th ed. Thieme; 2008. ↩
- Clavero J a, Golanó P, Fariñas O, Alomar X, Monill JM, Esplugas M. Extensor mechanism of the fingers: MR imaging-anatomic correlation. Radiographics. 2003;23(3):593-611. doi:10.1148/rg.233025079. ↩
- Timins ME, O’Connell SE, Erickson SJ, Oneson SR. MR imaging of the wrist: normal findings that may simulate disease. Radiographics. 1996;16(5):987-995. doi:10.1148/radiographics.16.5.8888385. ↩
- Roth KM, Blazar PE, Earp BE, Han R, Leung A. Incidence of Extensor Pollicis Longus Tendon Rupture After Nondisplaced Distal Radius Fractures. J Hand Surg Am. 2012;37(5):942-947. doi:10.1016/j.jhsa.2012.02.006. ↩
- Hu CH, Fufa D, Hsu CC, Lin Y Te, Lin CH. Revisiting spontaneous rupture of the extensor pollicis longus tendon: eight cases without identifiable predisposing factor. Hand. 2015. doi:10.1007/s11552-015-9746-y. ↩
- Gary M. Lourie, MD, Andrew Putman, MD, Taylor Cates, MD, and Allan E. Peljovich M. Extensor Pollicis Longus Ruptures in Distal Radius Fractures: Clinical and Cadaveric Studies With a New Therapeutic Intervention. Am J Orthop. 2015;44(May):209-212. ↩
- Björkman A, Jörgsholm P. Rupture of the extensor pollicis longus tendon: A study of aetiological factors. Scand J Plast Reconstr Surg Hand Surg. 2004;38(1):32-35. doi:10.1080/02844310310013046. ↩
- Kim CH. Spontaneous Rupture of the Extensor Pollicis Longus Tendon. Arch Plast Surg. 2012;39:680-682. http://dx.doi.org/10.5999/aps.2012.39.6.680. ↩
- Taş S, Balta S, Benlier E. Spontaneous rupture of the extensor pollicis longus tendon due to unusual etiology. Balkan Med J. 2014;31(1):105-106. doi:10.5152/balkanmedj.2013.9027. ↩
- Wheeless CR, Nunley JA, Urbaniak JR, of Orthopaedic Surgery DUMCD. Wheeless’ Online Textbook of Orthopaedics. http://www.wheelessonline.com/ortho/extensor_pollicis_longus_rupture. Published 2017. ↩
- Engkvist O, Lundborg G. Rupture of the extensor pollicis longus tendon after fracture of the lower end of the radius-A clinical and microangiographic study. Hand. 1979;11(1):76-86. doi:10.1016/S0072-968X(79)80015-7. ↩
- Y. Hirasawa, Y. Katsumi, T. Akiyoshi KT and TT. Clinical and Microangiographic Studies on Rupture of the E.P.L. Tendon After Distal Radial Fractures. J Hand Surg (British Vol. 1990;15B(1):51-57. ↩
- Din KM, Meggitt BF. Mallet thumb. J Bone Jt Surgery-British Vol. 1983;65(5):606-607. papers3://publication/uuid/1A0F39B8-8E29-4FE0-AEAA-472708381B71. ↩
- Tabbal GN, Bastidas N, Sharma S. Closed Mallet Thumb Injury: A Review of the Literature and Case Study of the Use of Magnetic Resonance Imaging in Deciding Treatment. Plast Reconstr Surg. 2009;124(1):222-226. doi:10.1097/PRS.0b013e3181ab1172. ↩
- Arvanitakis M, Calcagni M, Giesen T. Closed mallet thumb injury treated surgically: a case report. Case Reports Plast Surg Hand Surg. 2017;4(1):27-29. doi:10.1080/23320885.2017.1308830. ↩
- De Smet L, Van Ransbeeck H. Mallet thumb. Acta Orthop Belg. 2003;69(1):77-78. ↩