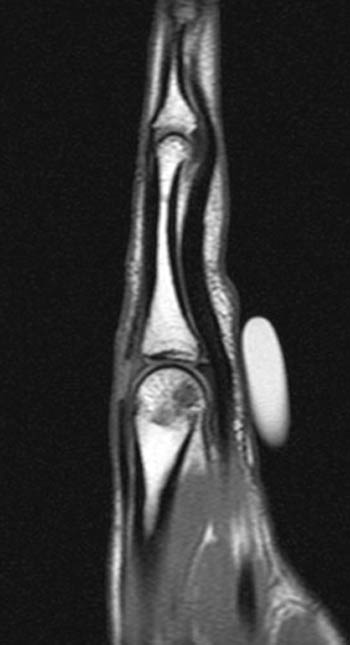
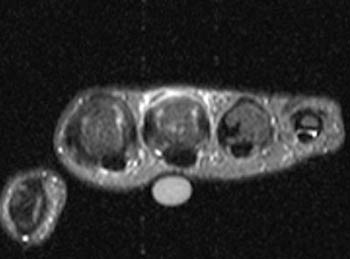
Clinical History: A 39 year-old female who cut her long finger on a tuna can presents with pain and limited extension at the MCP joint. Sagittal T1 (1a) and axial proton-density fat-suppressed (2a) images are provided. What are the findings” What is your diagnosis?
Findings
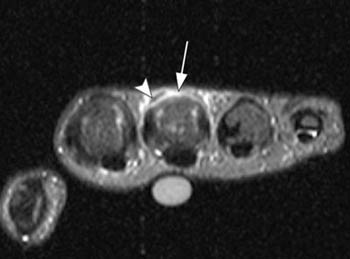
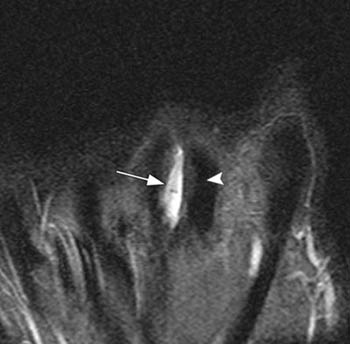
Figure 4:
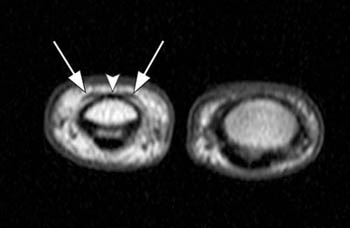
(4a) A fat-suppressed axial proton-density image obtained at the level of the long metacarpal head demonstrates absence of the extensor digitorum communis tendon centrally (arrow) with edema at the site of injury. The sagittal band remains intact radially (arrowhead), likely explaining why the patient was still able to slightly extend the MCP joint.
Diagnosis
Laceration of the extensor digitorum communis tendon just proximal to its insertion at the proximal phalangeal base.
Background
Finger extension involves the coordinated action of both the extrinsic and intrinsic extensor muscles. The extrinsic muscles originate in the forearm and function to extend the metacarpophalangeal (MCP) and interphalangeal joints. The intrinsic muscles originate within the hand and serve to extend the interphalangeal joints and contribute to flexion of the MCP joints. These extrinsic and intrinsic muscles are joined and coordinated by a stabilizing array of fibrous structures known as the extensor mechanism.1
MR imaging of the finger is technically challenging, but the use of optimized protocols, surface coils, and small fields-of-view often allow direct visualization of the components of the extensor mechanism. It is important to be familiar with the normal anatomy so that injuries to this important structure can be identified and appropriate treatment undertaken.
Anatomy
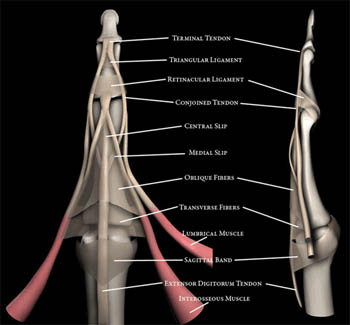
The extensor mechanism is one of the most complex structures in the hand (5a). At the level of the MCP joint, the extensor digitorum tendon is joined by the sagittal bands, one of the main components of the extensor hood. The sagittal bands attach volarly to the palmar plate of the MCP joint and dorsally to the extensor tendon. They serve to stabilize the extensor tendon, limit proximal excursion of the tendon, and aid in extension of the proximal phalanx.2
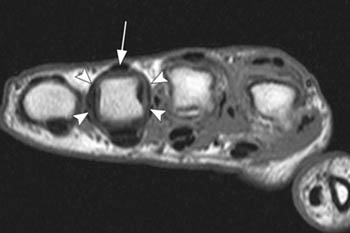
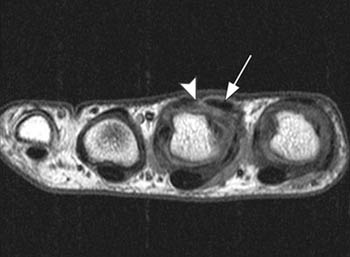
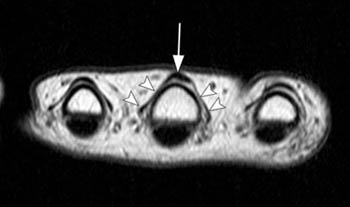
On axial MR images, the central extensor tendon is an oval low signal intensity structure that should be centered over the metacarpal head. The sagittal bands appear as thin, low signal structures extending circumferentially from the volar plate to the central extensor tendon (6a). With injury to the sagittal band, the extensor tendon will be subluxed or dislocated and the sagittal band will be discontinuous (7a, 8a). The patient often complains of pain and swelling at the MCP joint and a snapping sensation.
Distal to the MCP joint, the extensor digitorum tendon divides into three parts, the central slip and two lateral bands. The central slip inserts on the base of the middle phalynx. The lateral bands are joined by fibers from the intrinsic tendons, forming the conjoined tendons. The conjoined tendons merge distally to form the terminal tendon, which inserts on the base of the distal phalanx. The triangular ligament is located between the conjoined tendons and serves to keep them centered over the finger.2
The extensor mechanism is best evaluated on sagittal and axial MR images. The tendons are of low signal intensity on all pulse sequences. The specific appearance will depend upon the level of the finger imaged (10a,11a). Midline sagittal images are useful for evaluation of the insertion of the central slip and the terminal tendon (9a).
Figure 10:
(10a) Axial T1 image at the level of the proximal phalanx. The dorsal bundle of fibers is the central extensor tendon (arrow). The areas of thickening medially and laterally (arrowheads) represent the contribution of the intrinsic tendons (oblique and transverse fibers) to the extensor mechanism.
Mechanism of Injury
Injuries to the extensor tendons of the hand and wrist are common. The structures involved are thin and superficially located. These factors predispose to lacerations and also to closed injuries, including avulsions. The tendon rupture may be partial or complete. Typically, patients will present with pain and diminished function of the affected tendon. Prior to the advent of MR imaging, clinical examination or tenography were utilized for evaluation of suspected tendon injuries. Radiography remains an important examination to exclude bone avulsion or other subtle osseous injury.3
Treatment
For the purposes of diagnosis and treatment, extensor tendon injuries are classified into anatomic zones based on location. The most widely accepted is the Verdan system,4,5 which includes eight zones. The odd zones are the joint areas (Zone I is at the level of the DIP joint, Zone III at the PIP joint, Zone V at the MCP joint, and Zone VII at the wrist). In these locations, the extensor apparatus contains longitudinal fibers as well as transverse elements that keep the tendon centered and attached to the joint. The even zones are between the joints. In these locations, the extensor mechanism is semicircular, covering the dorsal aspect of the finger. Therefore, a partial lesion is usually found in the even zones. The extensor mechanism is highly vascular, predisposing to formation of adhesions from the injured tendon to adjacent structures. A brief summary of treatment options in injuries to the finger extensor mechanism (Zones I ” V) follows.4,5
Injuries in Zone I (the DIP joint) are typically closed and involve the terminal tendon insertion to the distal phalanx (mallet finger). The mechanism is commonly a sudden forceful flexion of the DIP joint in an extended digit. The most common treatment is closed splinting with the DIP joint in extension.
Injuries in Zone II (middle phalanx) are usually due to a laceration. As the conjoined tendons surround the dorsal half of the phalanx, a laceration seldom disrupts the entire extensor apparatus. If less than 50% of the tendon is involved, treatment consists of splinting followed by active motion. If more than 50% of the tendon is disrupted, it is typically primarily repaired.
Zone III (PIP joint) injuries involve the insertion of the central slip and may be open or closed. An avulsion fracture of the middle phalangeal base is often associated. A boutonniere deformity may develop as a late complication. Initial treatment is splinting of the PIP joint in extension. Surgical indications include a displaced avulsion fracture, instability of the PIP joint, and chronic symptomatic digits.
Zone IV (proximal phalanx) injuries and treatment considerations are similar to those encountered in Zone II.
Zone V (MCP joint) injuries (like our test case) are almost always open injuries. These commonly occur due to direct trauma, such as a human bite sustained during a fight. As the tendon is injured with the joint in flexion, the site of injury is usually proximal to the skin laceration. Primary surgical repair is indicated. A closed injury can occur to the sagittal bands, resulting in subluxation of the extensor tendon. Surgical repair of the sagittal band is often required in such cases.
Conclusion
With its high spatial resolution and ability to differentiate adjacent soft tissues, MR allows excellent visualization of the structures of the digital extensor mechanism. To take full advantage of the benefits of MR imaging, the intricate anatomy of the extensor mechanism must be appreciated. By understanding the normal appearance and function of the extensor mechanism, the injuries encountered can be accurately diagnosed and appropriate treatment can be undertaken.
References
1 Gilula LA and Yin Y. Imaging of the Wrist and Hand. Philadelphia, PA: W.B. Saunders, 1996
2 Hollinshead, WH. Anatomy for Surgeons: The Back and Limbs. Philadelphia, PA: Harper & Row, 1982.
3 Berquist TH. MRI of the Hand and Wrist. Philadelphia, PA: Lippincott, 2003.
4 Clavero JA, Golano P, Farinaas O, Alomar, X, Monill JM, Esplugas, M. Extensor Mechanism of the Fingers: MR Imaging ” Anatomic Correlation. Radiographics 2003; 23:593-611.
5 Clavero JA, Alomar X, Monill JM, Esplugas M, Golano P, Mendoza M, Salvador A. MR Imaging of Ligament and Tendon Injuries of the Fingers. Radiographics 2002; 22:237-256.