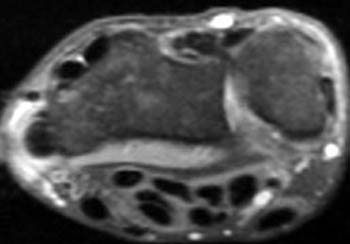
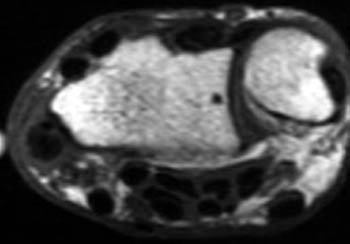
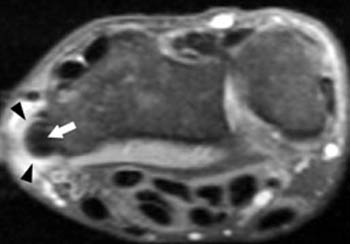
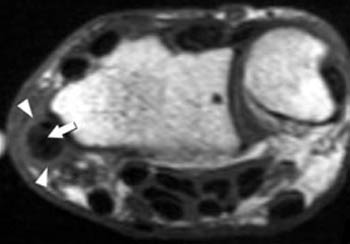
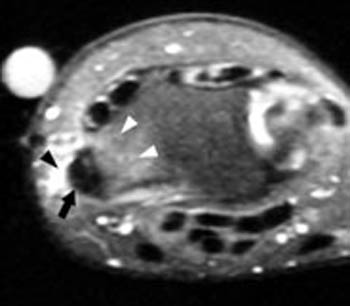
Clinical History: Dorsoradial wrist pain in a 50 year-old golfer. Axial (1a) fat-suppressed proton density and (1b) T1-weighted images through the distal radius are provided. What are the findings? What is your diagnosis?
Findings
Diagnosis
De Quervain’s Tenosynovitis.
Discussion
Tenosynovitis and tendinosis of the abductor pollicis longus (APL) and extensor pollicis brevis (EPB) tendons is called de Quervain’s tenosynovitis. First described by Swiss surgeon Fritz de Quervain in 1895,1 this condition is commonly encountered as an overuse injury. Swelling associated with tenosynovitis and tendinosis in the first dorsal compartment leads to painful restriction of movement of the thumb.
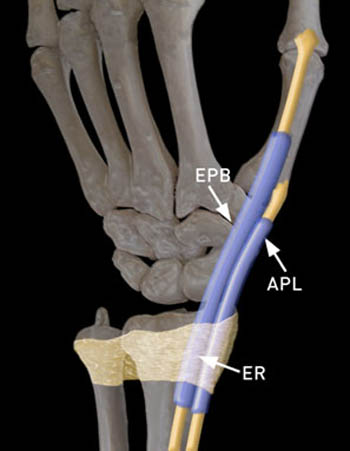
The extensor retinaculum, through septa and direct attachments, forms the roof of the six extensor compartments. These fibro-osseous tunnels contain the extensor tendons of the wrist and hand. The first dorsal compartment overlies the radial styloid and contains the APL and EPB tendons, which are responsible for abduction and extension of the thumb at the carpometacarpal joint (4a). In de Quervain’s tenosynovitis, thickening and edema result in restriction of the normal gliding of the tendons through the relatively non-pliable first extensor fibro-osseous compartment.
Patients with de Quervain’s tenosynovitis typically present with dorsoradial wrist pain, limitation of thumb motion, and swelling. In almost all cases, there is a history of repetitive forceful gripping coupled with ulnar deviation or repetitive use of the thumb. Statistically most common in females, this condition may be seen in any age or sex, if the appropriate provocative overuse mechanisms are present. De Quervain’s tenosynovitis is the most common tendinopathy of the wrist in athletes, particularly those who participate in golf and racquet sports.2 It is also seen as an occupational injury in the workplace. An association between de Quervain’s and pregnancy in the immediate postpartum period is felt to be largely a result of endocrine influences and fluid retention.3 Recently “baby wrist” has been coined to describe the entity when seen in new mothers further removed from the postpartum. Prolonged carrying of babies with the wrist held in flexion and ulnar deviation and with the thumb in extension is felt to be the etiology.4
The diagnosis of de Quervain’s is usually made on physical examination by the Finkelstein’s test, in which ulnar deviation of the wrist with the fist closed over the flexed thumb illicits pain over the dorsoradial aspect of the wrist. Although the diagnosis is usually clinically apparent, the condition may be confused with other entities including intersection syndrome, radioscaphoid and trapeziometacarpal arthritis, scaphoid fracture, ligamentous sprains, ganglia and masses.
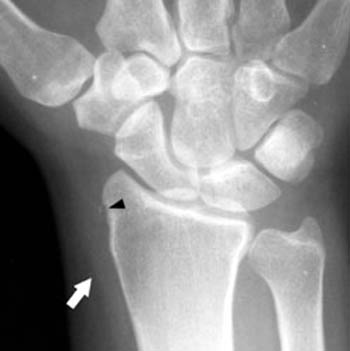
In longstanding cases, plain films may reveal bony changes of the radial styloid as well as soft tissue swelling (5a). Ultrasound may be used to detect the tenosynovitis but may fail to identify other conditions that may mimic the diagnosis. MRI proves most effective in identifying and differentiating such conditions as well as diagnosing de Quervain’s tenosynovitis. MRI findings of tenosynovitis include T2 hyperintense fluid signal within a thickened and distended tendon sheath, often with surrounding reactive soft tissue or marrow edema (6a). Tendinopathy associated with this condition ranges from mild tendon swelling to longitudinal splitting in severe cases.
Rest and immobilization are advocated in the early stages of de Quervain’s tenosynovitis. Corticosteroid injections into the first extensor compartment are often curative. Surgical release is necessary if these treatment regimens fail.
Conclusion
The diagnosis of de Quervain’s tenosynovitis is usually made clinically. However, in patients with a confusing clinical presentation, MRI is preferred for confirming the diagnosis and differentiating the entity from other conditions that cause dorsoradial wrist pain.
References
1 DeQuervain F: Ueber eine Form von chronischer Tendovaginitis. Corresp Blatt Schweizer Arzte 1895; 25: 389-94.
2 Rettig AC Athletic Injuries of the Wrist and Hand, Part II: Overuse Injuries of the Wrist and Hand and Traumatic Injuries to the Hand. The American Journal of Sports Medicine;32:262-273.
3 Schned ES. De Quervain tenosynovitis in pregnant and postpartum women. Obstet Gynecol 1986;68:411-414.
4 Anderson SE, et al. “Baby Wrist”: MRI of an Overuse Syndrome in Mothers. AJR 2004;182:719-724.