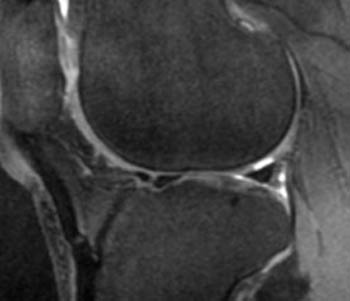
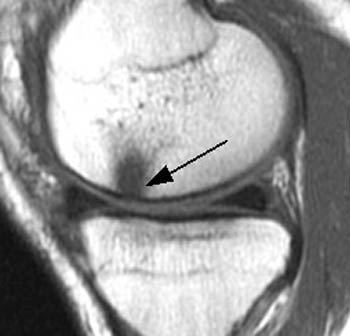
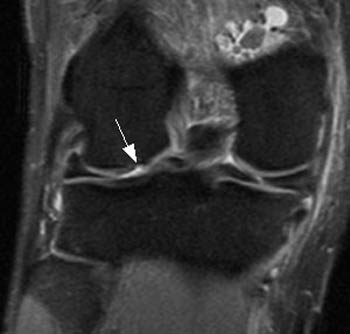
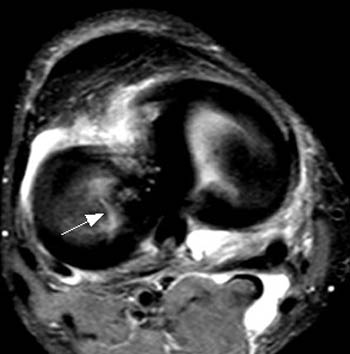
Clinical History: 40 year-old male status-post twisting injury–now with knee pain and clicking. Fat-suppressed water excitation sagittal (1a) and fat-suppressed proton density weighted fast spin-echo coronal (1b) images are provided. What are the findings? What is your diagnosis?
Findings
Answer
Full-thickness cartilage defect at the posterior weight-bearing surface of the lateral femoral condyle.
Discussion
With the advent of improved therapies for the treatment of cartilage injuries, MRI has assumed an increasingly important role in the detection and evaluation of cartilage defects. Such injuries are not uncommon, but are often difficult to diagnose clinically, as symptoms may be indistinguishable from the more prevalent meniscal tear. From an imaging standpoint, without proper technique and awareness of the characteristic findings, cartilage defects may be easily overlooked.
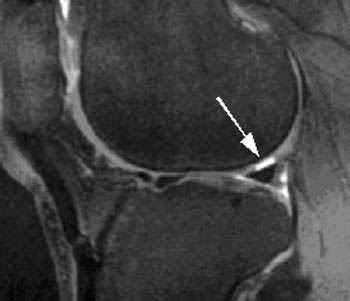
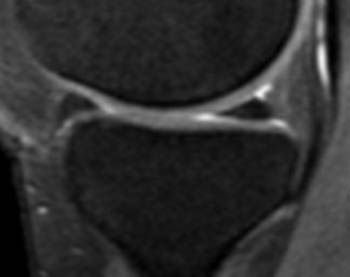
Many different MR techniques have been utilized for the detection of cartilage defects.1 Cutting-edge methods such as T2-mapping and dynamic contrast-enhanced studies of articular cartilage are exciting, but from a practical standpoint, are rarely used in everyday practice. Most imagers rely on gradient-echo sequences (3a) or fast-spin echo images with fat-suppression (4a) for detection of cartilage defects at the knee.2 The key to the success of these techniques is their ability to create high contrast between articular cartilage, adjacent bone, and joint fluid.
When utilizing such techniques for the detection of cartilage defects, one typically relies on the recognition of high signal-intensity joint fluid undermining the contour of normal, lower signal intensity articular cartilage. In acute injuries, adjacent osteochondral injuries and/or bone bruises are often present, and should raise one’s level of suspicion in the search for cartilage lesions.3
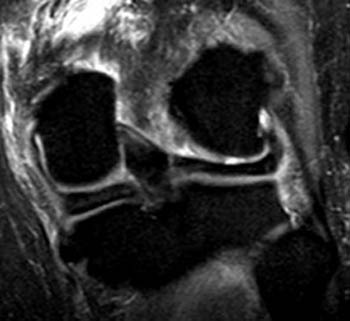
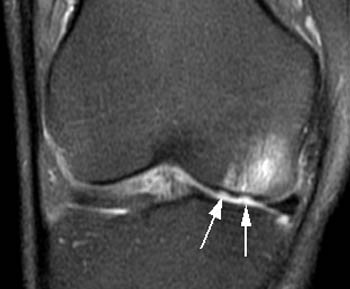
Figure 6:
On (6a), the fat-suppressed fast spin-echo proton density weighted coronal view, two discrete cartilage defects (arrows) are apparent beneath the site of osseous injury. Note that these defects are not visible on (E), as T1-weighted images are relatively insensitive for cartilage lesions.
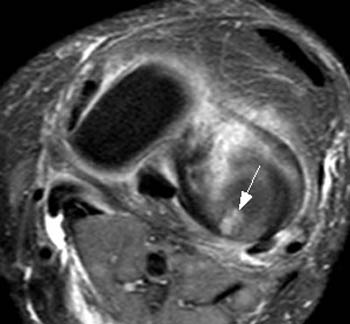
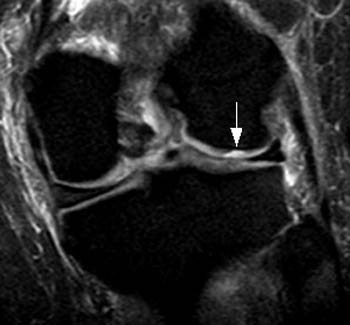
Although radiologists usually rely upon the sagittal and coronal imaging planes for diagnosis of femoral condylar cartilage defects, we have found that fluid-sensitive axial images can actually be quite useful in the detection and characterization of cartilage defects. In patients with intact articular cartilage at the femoral-tibial joint, the congruent cartilage surfaces allow only minimal amounts of fluid to collect within the joint itself. In patients with cartilage defects at the joint, fluid typically fills the defect, creating a localized fluid collection that is often visible en face in the axial plane. This localized fluid, which we have called the “crater sign”, may be used as an indicator for the presence of a cartilage defect at the knee (7a,8a). In addition, the size and shape of the cartilage defect is often more easily determined by the “crater” than on sagittal or coronal sequences (9a,10a).
Conclusion
As methods for the treatment of cartilage disorders evolve, the ability to diagnose cartilage defects becomes increasingly important. MR’s superior contrast resolution makes it ideally suited for the evaluation of chondral disorders at the knee. Detection of cartilage abnormalities requires the combination of proper imaging technique and judicious image interpretation. Careful attention to ancillary findings such as marrow edema and the “crater sign” are helpful in maximizing sensitivity for the detection of cartilage lesions at the knee.
References
1 Gold GE, McCauley TR, Gray ML, and Disler DG. Special Focus Session: What’s New in Cartilage” Radiographics 2003; 23 (5): 1227-1242.
2 Bredella MA, Tirman PF, Peterfly CG, et al. Accuracy of T2-weighted fast spin-echo MR imaging with fat saturation in detecting cartilage defects in the knee: comparison with arthroscopy in 130 patients. AJR 1999; 172: 1073-1080.
3 Rubin DA, Harner CD, and Costello JM. Treatable Chondral Injuries in the Knee: Frequency of Associated Focal Subchondral Edema. AJR 2000; 174: 1099-1106.