Clinical History:
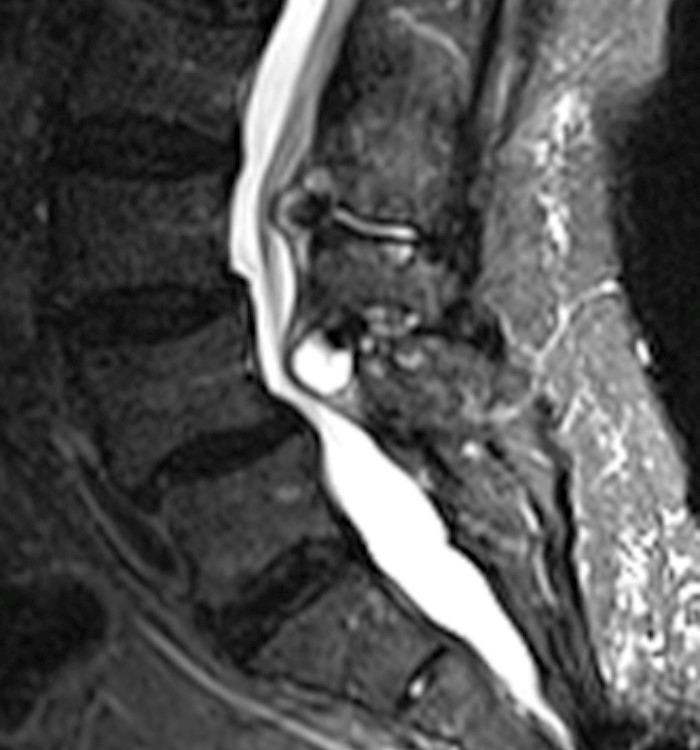
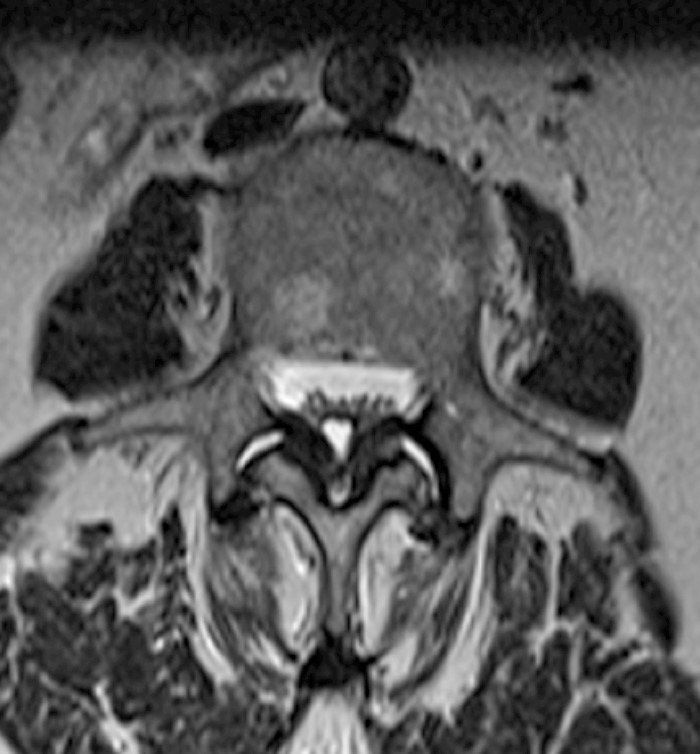
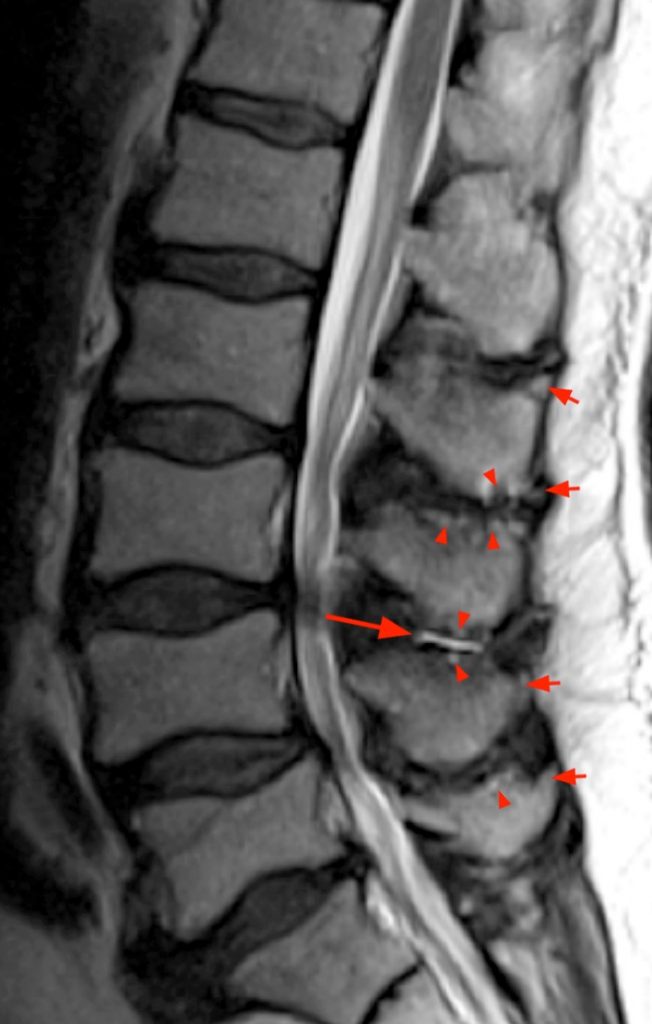
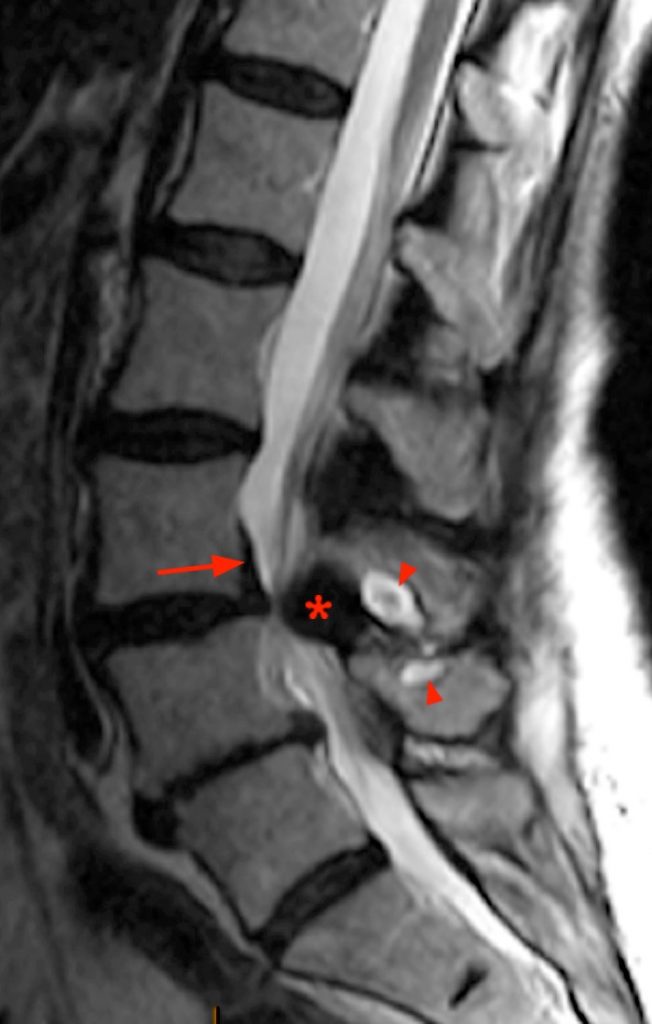
An 84 year-old female presents with low back pain, right leg pain, hip pain, numbness and weakness. STIR sagittal (1a) and T2-weighted axial (1b) MR images of the lumbar spine are provided.
What are the findings? What is your diagnosis?
Findings
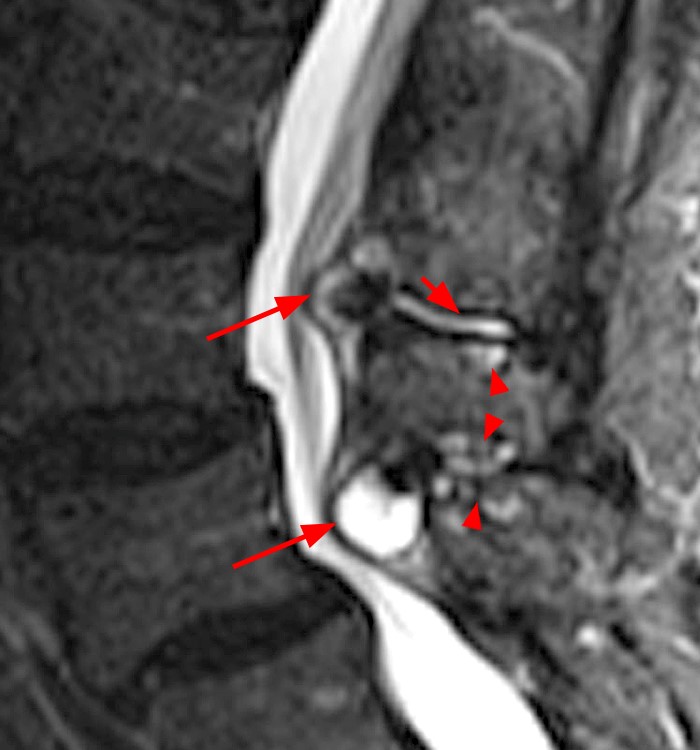
Figure 2:
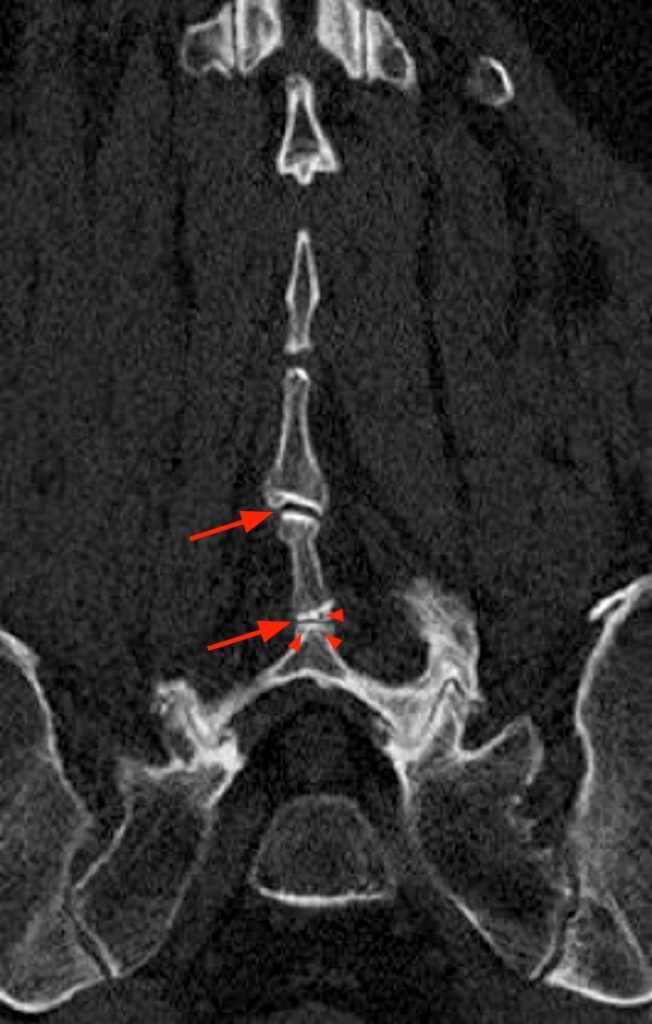
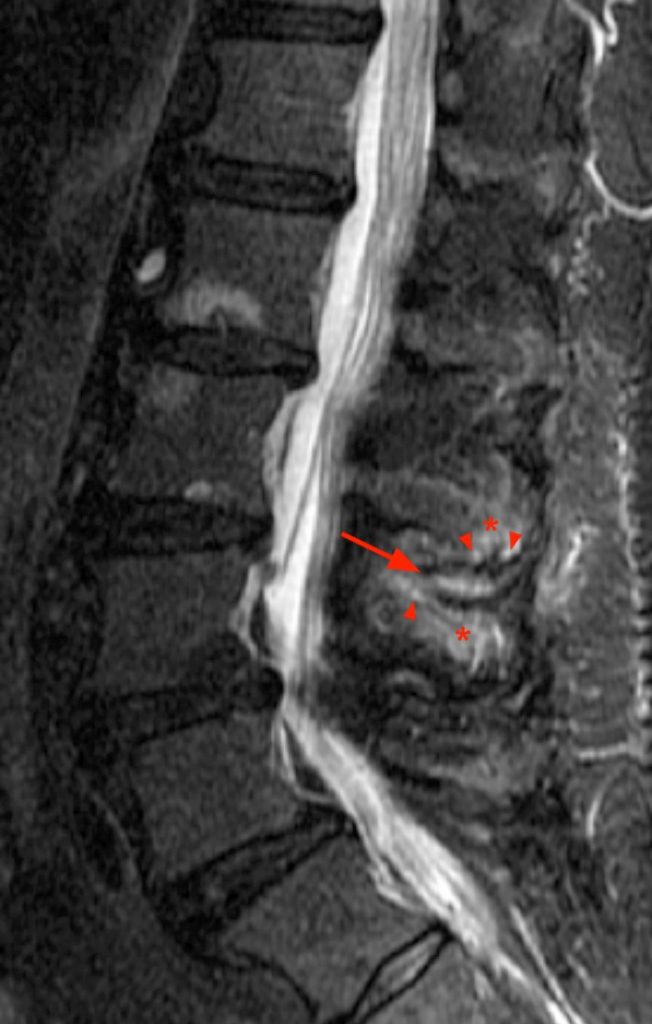
(2a) The sagittal STIR image, demonstrates abnormalities at the L2-3 and L3-4 levels, with apposition of the spinous processes, subcortical cystic changes (arrowheads), and dorsal midline epidural cysts (arrows), which cause posterior compression of the thecal sac, abutment of the descending nerve roots of the cauda equina, and contribute to central canal stenosis at these levels. At the L2-3 level, there is interspinous bursitis (short arrow), which is in direct communication with the dorsal epidural cyst. Fibrosis is present within the dorsal epidural cysts, as well as posteriorly, along the supraspinous ligament. Mild anterolisthesis of L3 on L4 and L4 on L5 are present, related to degenerative disc disease and facet arthrosis (not shown).
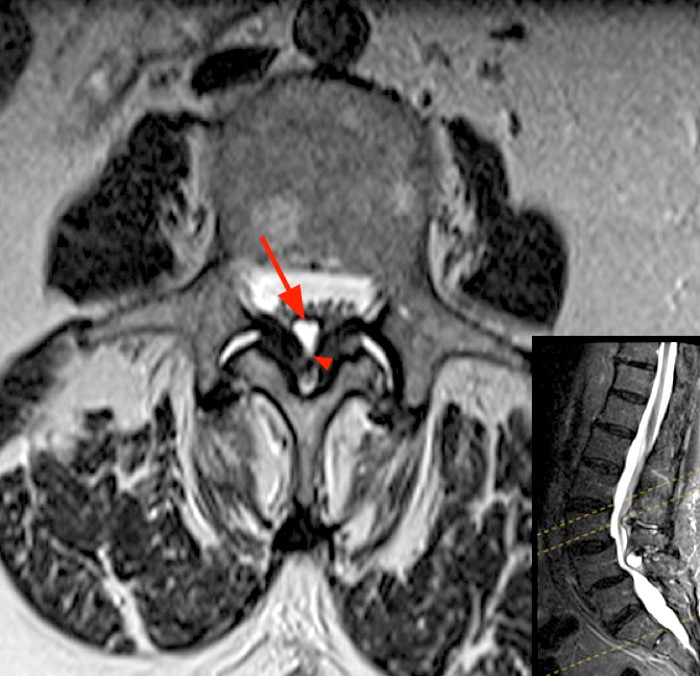
(2b) The axial FSE-weighted T2 image (with inset cross-reference sagittal STIR image) reveals a dorsal midline epidural cyst (arrow), with a neck extending into the midline cleft (arrowhead) between the thickened fibers of the ligamentum flavum.
Diagnosis
Dorsal midline intraspinal epidural cysts, associated with Baastrup’s Disease.
Introduction
Low back pain is extremely common, with a lifetime individual prevalence between 49% and 90%1,2,3,4,5, and it is a top 5 chief complaint in emergency departments in the United States and Canada.6,7 Back pain is often multifactorial, most commonly attributed to discogenic and facetogenic abnormalities. The interspinous region is an often overlooked cause of back pain. Baastrup’s disease, or kissing spinous processes, can cause pain, which is exacerbated with hyperextension or increased lordosis, and can rarely be associated with radiculopathy if there is an associated dorsal epidural cyst.
In 1933, Danish radiologist Christian Ingerslev Baastrup described pathologic changes that occur in adjacent lumbar spinous processes and the soft tissues between them, which are associated with back pain.8 Although the popular eponym is attributed to Baastrup, fluid filled cavities between overgrown lumbar spinous processes were previously reported in soldiers, by Mayer in 1825, and he called it “diarthrosis interspinosae”.9 In 1929, Brailsford described the radiologic findings of interspinous arthritis in patients who had pain in extension, that was alleviated with flexion, and called it “kissing spines”.10 The terms Baastrup’s disease, kissing spines, and interspinous bursitis have been used interchangeably by many authors.
Anatomy
The segments of the vertebral column are connected together by ligaments, which can be divided into five sets: those connecting the vertebral bodies, the laminae, the articular processes, the spinous processes, and the transverse processes. Each set can be subdivided, but for the purposes of this discussion we will concentrate on the ligaments of the laminae and spinous processes.
The ligamenta subflava connect the laminae and extend from the axis to the sacrum. Each consists of two lateral portions, which start at the roots of the articular processes and extend dorsally to the region where the laminae converge to form the spinous process. At this point they contact each other and are somewhat united, but contain natural central clefts that allow the passage of small vessels. It is through these natural clefts that posterior epidural cysts can extend into the central canal, from interspinous bursitis.
The ligaments of the spinous process are subdivided into the supraspinous and interspinous ligaments. The supraspinous ligament is a dense collagenous cord that attaches to the apices of each spinous process, starting at C7 and extending to the sacrum. It continues cephalad, from the C7 spinous process to the external occipital protuberance, as the ligamentum nuchae, where it is much thinner. The interspinous ligaments are thin membranous collagenous bands that extend from the root to the summit of each spinous process, interconnecting adjacent levels, extending ventrally to the ligamenta subflava, and dorsally to the supra-spinous ligament.
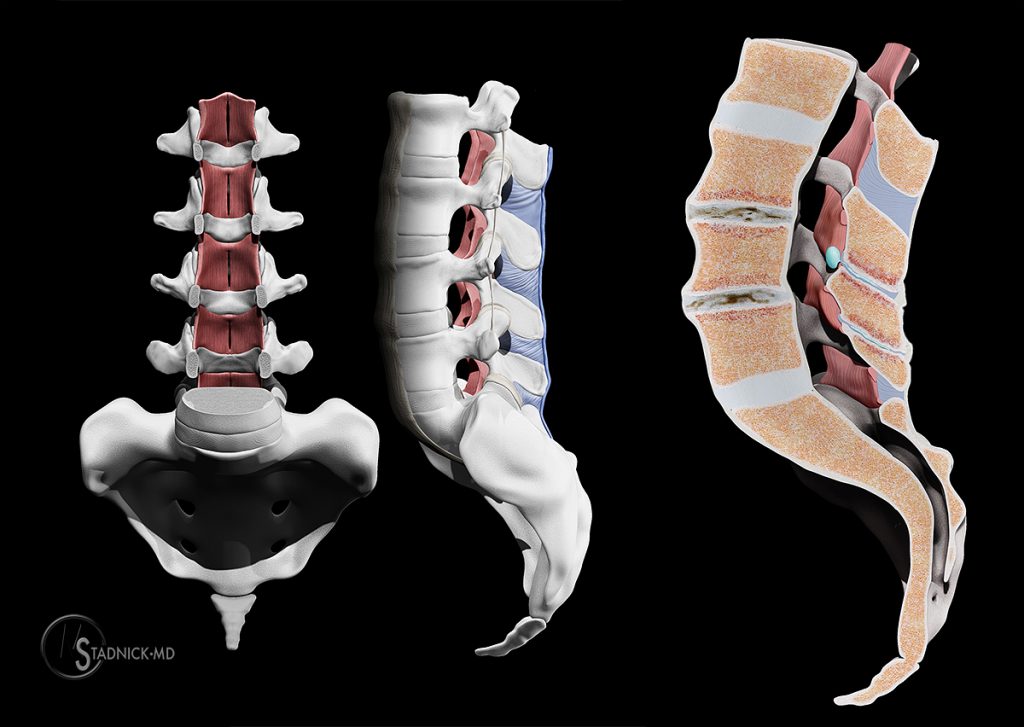
Figure 3:
The AP rendering of the lumbar spine with the vertebral bodies removed (left) demonstrates the normal ligamenta subflava (red) connecting the laminae. The normal supraspinous and interspinous ligaments (blue) are better seen on the lateral view of the spine (middle). The changes that can occur with Baastrup’s disease are illustrated on the right including close approximation of the spinous processes with bony hypertrophy and degenerative change, interspinal bursitis, and midline epidural cysts. Hyperlordosis, vertebral disc degeneration with narrowing, and spondylolisthesis are typically seen.
Discussion
Clinically, patients with Baastrup’s disease typically have midline pain, which radiates cephalad and caudad, that is increased with extension and alleviated with flexion.11 Pain can be reproduced with direct palpation of the pathologic interspinous ligament on physical exam.12 Patients can rarely present with neurogenic claudication.13
Interspinous bursitis has been described in the setting of calcium pyrophosphate dehydrate disease, hydroxyapatite crystal deposition disease, juvenile chronic arthritis, adult-onset rheumatoid arthritis and polymyalgia rheumatica.14,15 Occasionally, Baastrup’s disease can be seen in isolation.12 Frequency increases with age, as does the number of affected levels, with the peak incidence above 80 years old.16 The most commonly affected level is L4-5.16
Histologically, Baastrup’s disease is characterized by close approximation and abutment of spinous processes, interspinal bursitis, interspinous ligament degeneration/tears, subcortical cysts/erosions, edema, chondroid metaplasia, enchondral ossification involving apposing spinous processes, creation of synovial articulations, and occasionally the development of epidural cysts or epidural fibrotic masses.11, 12, 13, 16, 17
Radiologically, Baastrup’s disease is associated with hyperlordosis, loss of intervertebral disc height, disc bulges, facet arthrosis, spondylolisthesis, spondylosis and central canal stenosis.12, 16 Radiographs, CT scans and MRI demonstrate apposition of spinous processes, subcortical cysts, subcortical sclerosis and bone spurs (Figures 4-8). MRI also illustrates subcortical edema, interspinous bursitis, and if present the associated epidural cysts which can cause radiculopathy. Fluoroscopic injection of interspinous bursitis can show contrast communication with Baastrup’s associated epidural cysts, the facet joints, as well as pars interarticularis defects.17 When Baastrup’s interspinous bursitis communicates with both facet joints on fluoroscopic injection, it has the classic “butterfly” appearance.17 Nuclear medicine studies can demonstrate increased tracer uptake in the spinous processes on bone scan, and mild to moderate activity on PET/CT.18,19
Symptomatic Baastrup’s disease has been treated with oral analgesics, NSAID’s, steroids, localized injection and surgery.
Figure 4:
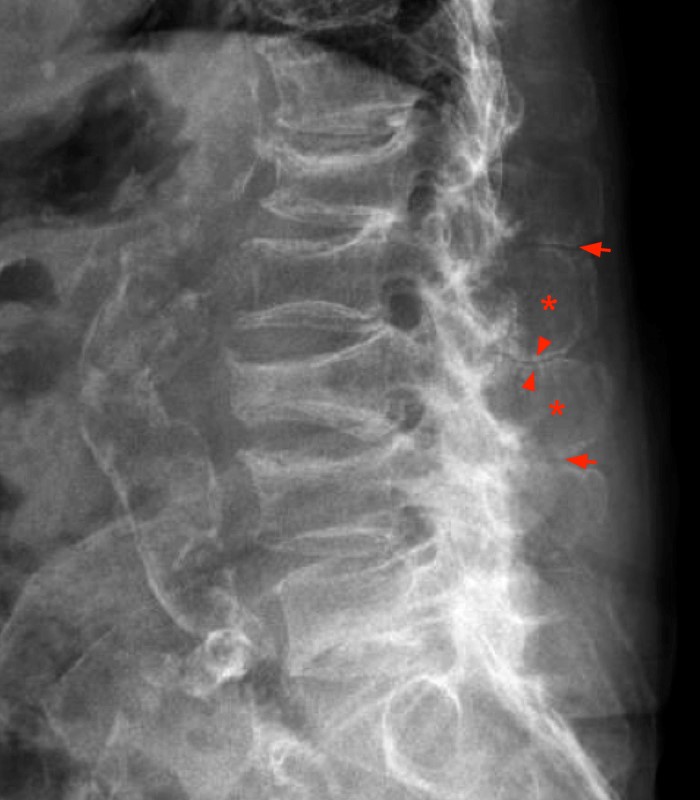
(4) Lateral lumbar spine radiograph of an 80 year old female patient, in attempted flexion, with a history of lumbar spondylosis illustrating enlargement of the L2 and L3 spinous processes (asterisks), with contact, subcortical sclerosis and flattening at the neoarticulation (arrowheads). Spinous process apposition with subcortical sclerosis is also present at L1-2 and L3-4 (short arrows). There is straightening of the normal lumbar lordosis in this erect patient imaged in flexion. Note is also made of multiple osteoporotic compression fractures, multi-level degenerative disc disease, facet arthrosis, and atherosclerotic calcification of a small abdominal aortic aneurysm.
Figure 5:
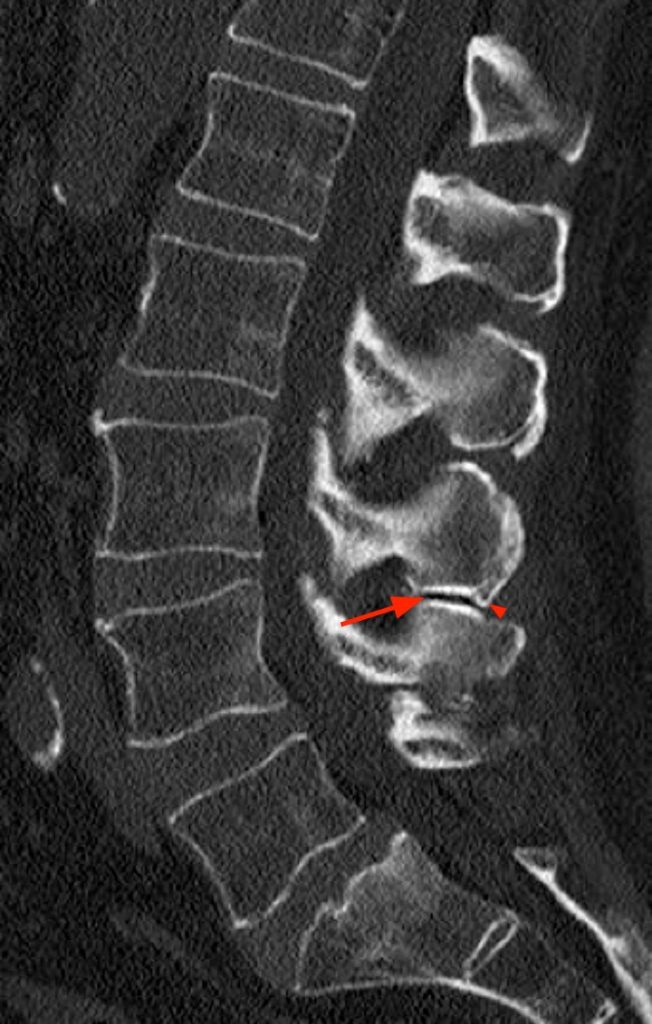
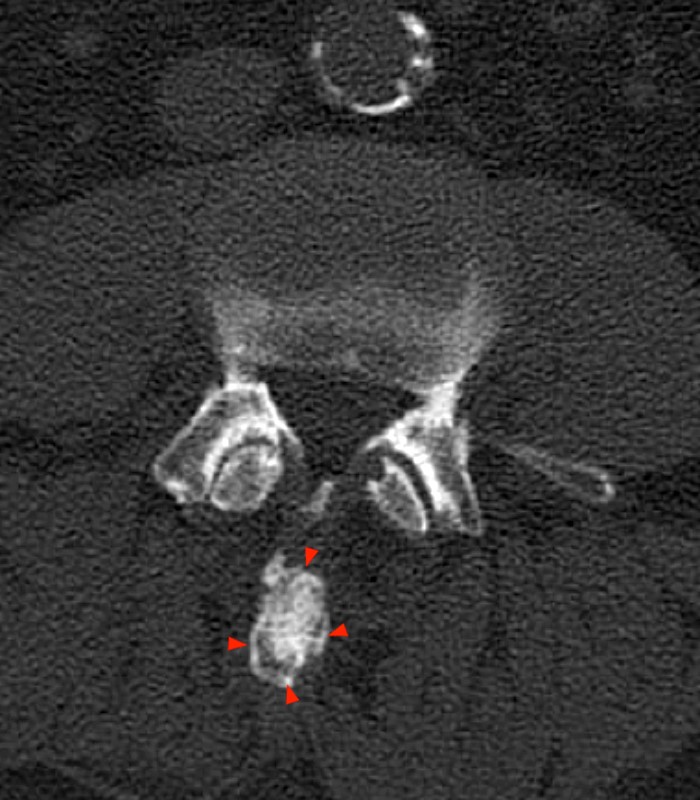
Computed Tomography (CT) images from a 69 year-old male patient with low back and right lower extremity pain for 15 years. (5a) Sagittal reconstructed CT image shows apposition of the L3-4 spinous processes, with subcortical sclerosis (arrow) and a small osteophyte (arrowhead). (5b) Axial CT image in the same patient demonstrates nodular enlargement of the spinous process (arrowheads). (5c) Coronal reconstructed CT image illustrates apposition and flattening of the L3-4 and L4-5 spinous processes (arrows), with tiny subcortical cysts and sclerosis at L4-5 (arrowheads).
Figure 6:
A sagittal T2-weighted MR image in a 75 year-old male with chronic low back pain demonstrates interspinous bursitis (arrow) at L3-4, apposition of the L2-5 spinous processes with small spurs (short arrows), subcortical cysts (arrowheads) and sclerosis, in a patient with congenitally short pedicles and degenerative disc disease that contribute to multi-level central canal stenosis.
Figure 7:
Sagittal T2-weighted MR image in an 81 year-old female with low back pain radiating into the hips and legs, demonstrates large subcortical cysts in the L3-4 spinous processes (arrowheads). There is severe L2-3 spinal stenosis related to a central disc extrusion (arrow) and severe thickening of the ligamentum flavum (asterisk).
Figure 8:
Sagittal STIR MR image in a 69 year-old male with low back pain radiating into bilateral buttocks with numbness and tingling, shows interspinous bursitis (arrow), with subcortical cysts (arrowheads) and edema (asterisks). There is also multi-level spondylolisthesis related to multi-level degenerative disc disease, small extrusions, and facet arthrosis (not shown) with multi-level central canal stenosis.
Conclusion
Back pain is excessively prevalent, often multifactorial in nature, but most frequently discogenic or facetogenic in origin. The interspinous region is an often overlooked cause of back pain. Baastrup’s disease, or kissing spinous processes can cause pain, which is exacerbated with hyperextension or increased lordosis, and can rarely be associated with radiculopathy if there is an associated dorsal epidural cyst.
Radiologic findings of Baastrup’s disease include apposition of spinous processes, subcortical cysts, subcortical sclerosis, subcortical edema, osteophytes, interspinous bursitis, and occasionally epidural cysts. Baastrup’s disease is also associated with loss of intervertebral disc height, disc bulges, facet arthrosis, spondylolisthesis, spondylosis and central canal stenosis.
Symptoms of Baastrup’s disease are often indistinguishable from other causes of back pain. MRI is an excellent tool in the evaluation of patients with back pain with or without radiculopathy, and provides a valuable roadmap in treatment planning.
References
- Van Tulder M, Koes B, Bombardier C. Low back pain. Best Pract Res Clin Rheumatol. 2002; 16:761–75. ↩
- Margarido MS, Kowalski SC, Natour J, Ferraz MB. Acute low back pain: Diagnostic and therapeutic practices reported by Brazilian rheumatologists. 2005; 30:567–71. ↩
- Devereaux MW. Low back pain. Prim Care. 2004; 31:33–51. ↩
- Woolf AD, Pleger B. Burden of major musculoskeletal conditions. Bull World Health Organ. 2003; 81:646–56. ↩
- Nyiendo J, Haas M, Goldberg B, Sexton G. Pain, disability, and satisfaction outcomes and predictors of outcomes: A practice-based study of chronic low back pain patients attending primary care and chiropractic physicians. J Manipulative Physiol Ther. 2001; 24:433–9. ↩
- Canadian Institute for Health Information, A Snapshot of Health Care in Canada as Demonstrated by Top 10 Lists, 2011 (Ottawa, Ont.: CIHI, 2012). ↩
- Nunn M, Edwards J, Hayden JA, Kiberd J, Magee K. Prevalence & Management Practices for Patients Presenting to the Emergency Department with Low Back Pain.Buxton: Poster presented at International Back and Neck Pain Forum; 2016. ↩
- Baastrup CL. Proc spin. Vert. lumb. Und einige zwischen diesen liegenden Gelenkbildungen mit pathologischen Prozessen in dieser Refion. Fortschritte auf dem Gebiete der Rontgenstrahlen 1933; 48:430-435. ↩
- Uber zwei neuentdeckte Gelenke an de Wirbelsaule des menschlichen Korpers. Z Physiol 1825; 2:29-35. ↩
- Brailsford JF. Deformities of the lumbo-sacral regions of the spine. Br J Surg 1929; 16:562-627. ↩
- Bywaters EG, Evans S (1982) The lumbar interspinous bursae and Baastrup’s syndrome an autopsy study. Rheumatol Int 1:87-87. ↩
- Filippiadis DK, Maxioti A, Argentos S, Anselmetti G, Papakonstantinou O, Kelekis N, Kelekis A. Baastrup’s disease (Kissing spines syndrome): a pictorial review. Insights Imaging (2015) 6:123-128. ↩
- Rajasekaran S, Pithway YK. Baastrup’s Disease as a Cause of Neurogenic Claudication. Spine. 2003; 28(14):E273-275. ↩
- Bywaters EG. Rheumatoid and other diseases of the cervical interspinous bursae and changes in the spinous process. Ann Rheum Dis. 1982; 41:360-370. ↩
- Salvarani C, Barozzi L, Cantini F, Niccoli L, Boiardi L, Valentino M, Pipitone N, Bajocci G, Macchioni P, Catanoso MG, Olivieri I, Hunder GG. Ann Rheum Dis. 2008 June; 67(6):758-761. ↩
- Maes R, Morrison WB, Parker L, Schweitzer ME, Carrino JA. Lumbar interspinous bursitis (Baastrup disease) in a symptomatic population: prevalence on magnetic resonance imaging. Spine. 2008; 33(7):E211-E215. ↩
- Chen CK, Yeh LR, Resnick D, Lai PH, Liang HL, Pan HB, Yang CF. Intraspinal Posterior Epidural Cysts Associated with Baastrup’s Disease: Report of 10 Patients. American Journal of Roentgenology 2004 182:1,191-194. ↩
- Kim YS, Jun JB, Lee SH, Coi YY. An Unusual Cause of Lower Back Pain; Baastrup’s Disease. J Rheum Dis. 2011 June; 18(2):147-149. ↩
- Ho, L, Wassef H, Seto J, Henderson R. Multi-Level Lumbar Baastrup Disease on F-18 FDG Pet-CT. Clinical Nuclear Medicine. 2009; 34(12):896-897. ↩