Clinical History: A 16 year-old female presents with shoulder pain and stiffness for 2 months. The symptoms are getting worse. She reports no specific injury. The pain started when she increased her softball activities and overhead weightlifting. What are the findings? What is your diagnosis?
Findings
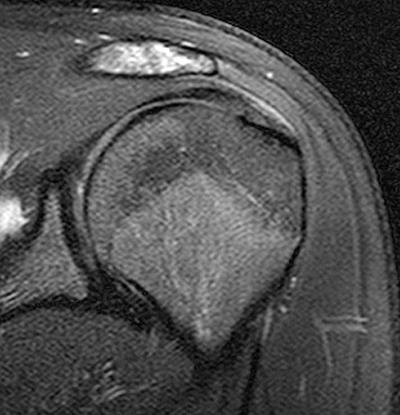
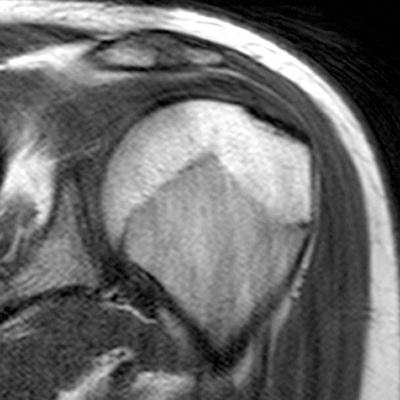
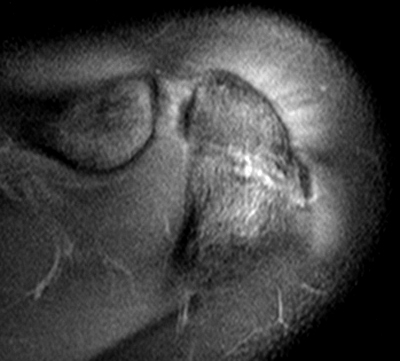
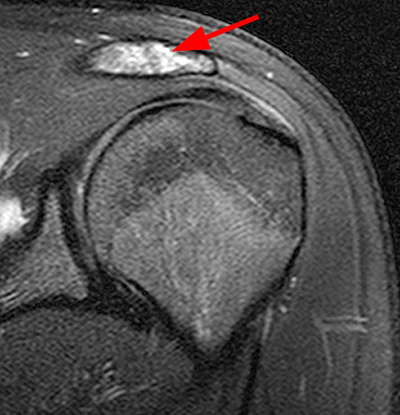
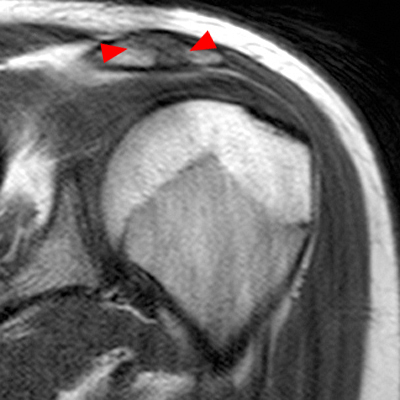
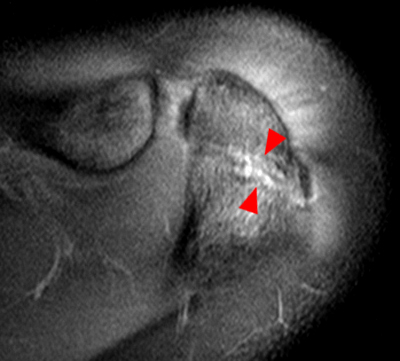
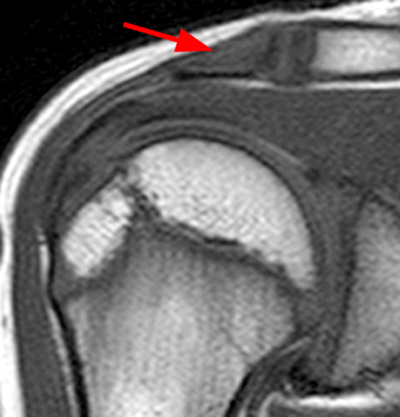
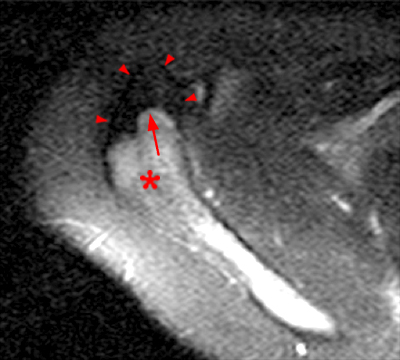
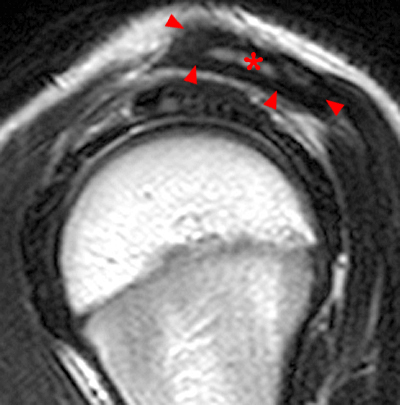
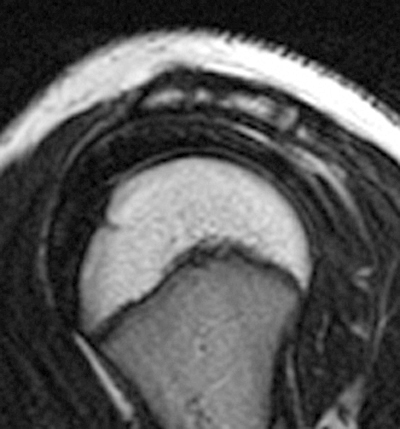
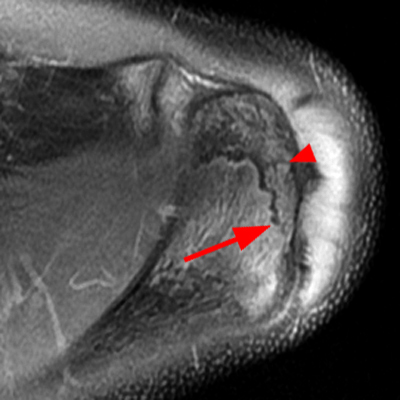
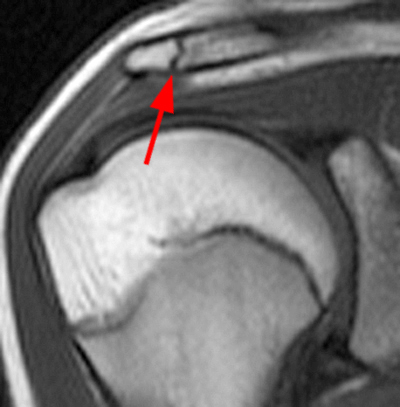
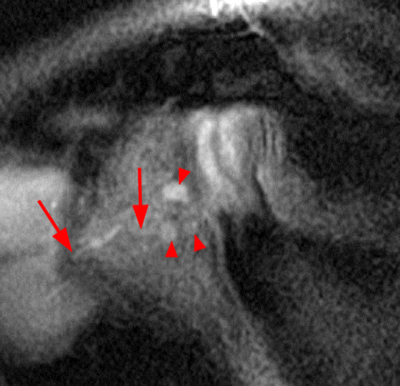
Figure 2:
2a Diffuse marrow edema is present within the acromion (arrow). 2b The margins at the growth plate of the acromion are indistinct and irregular (arrowheads). 2c Diffuse marrow edema is noted throughout the visualized portion of the acromion. The growth plate of the acromion is mildly widened and irregular (arrowheads) and has a straight, linear course from medial to lateral.
Diagnosis
Acromial apophysiolysis (os acromiale in an adolescent)
Introduction
The growth plates of the upper extremities in pitchers and other athletes are susceptible to injury and repetitive stress, such as in little leaguer’s shoulder and elbow, which may lead to deformity, chronic pain and disability. Repetitive traction forces related to pulling of the deltoid on the developing acromion may result in failure of fusion of the acromion, also known as acromial apophysiolysis, and formation of an os acromiale which may or may not be symptomatic.1 The diagnosis of an os acromiale is not commonly made in patients younger than 25 years, because it has been thought that the age range of acromial fusion is from 18 to 25 years.2 Other studies have shown that the acromion is fused in most children by the age of 16 years.3 It is therefore possible to develop an os acromiale at a younger age than what has generally been thought, which has important implications for imaging diagnosis and treatment.
Differentiation between the normal developing acromion and stress changes at the acromial growth plate on MR imaging can be challenging. This Web Clinic showcases the main differences and pitfalls in diagnosis.
Epidemiology and clinical presentation
Acromial apophysiolysis was reported in 2.6 % of patients aged 15-25 years presenting with shoulder pain in a recent study.1 In another study which included only adolescents, 8 % of the patients had similar findings.4 Risk factors include repetitive stress and especially throwing more than 100 pitches per week (baseball in male patients and softball in female patients).1 Other athletes such as competitive swimmers and football players are also at risk.5,6 The patients typically present with superior shoulder pain and/or tenderness over the acromion.1
Normal development of the acromion on MRI
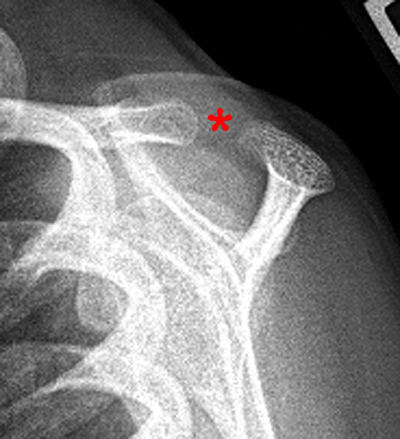
In younger children, <10 years old, the acromial process has the same shape as those of older children and adults, but has homogeneous signal similar to cartilage (Fig. 3). The relatively large portions of the acromion and distal clavicle that are not yet ossified could give the false appearance of acromioclavicular separation on radiographs (Fig. 4). The ossified portion of the acromion is often hyperintense on water sensitive MR images due to the presence of a high concentration of red marrow, which could be misinterpreted as marrow edema.7
In children aged 10-14 years, the ossification of the acromion takes place in an asymmetrical fashion with the leading anterior margin of the ossification being U-shaped on axial images (Fig 5). The chondro-osseous junction has a lobulated configuration.7
Figure 5:
An axial image of the normal acromion in an 11 year-old boy. The leading anterior margin of the ossification has an inverted U-shaped configuration (arrow). The secondary ossification centers have not yet appeared, but the normal shape of the cartilaginous precursor of the acromial process is still fairly well demonstrated. The hyperintense signal of the marrow (asterisk) in the acromion is related to normal red marrow.
The secondary ossification centers of the distal acromion vary in number, and appear between the ages of 10 and 14 years. The individual centers can be difficult to evaluate due to their small size, irregular margins, and partial volume averaging. Usually, they form in the anterior and lateral aspects of the cartilaginous acromial process and have signal similar to fat on MRI (Fig. 6,7).7 The heterogeneous signal on MRI in the region of normal ossification centers should not be mistaken for an acromial fracture, which is typically associated with marrow edema (Fig.8).
Gradually, as the centers coalesce, there are three major foci of ossification which form: the preacromion, the mesoacromion and the meta-acromion (Fig.9). Detailed analysis of the ossification and fusion of the acromion in anatomic studies and with MRI has revealed an arrangement that is somewhat different from the original theory of the side by side, parallel orientation of ossification centers.4,8 Initially, the fusion of the preacromion and the mesoacromion takes place, followed by the fusion of the meta-acromion and the basi-acromion.8
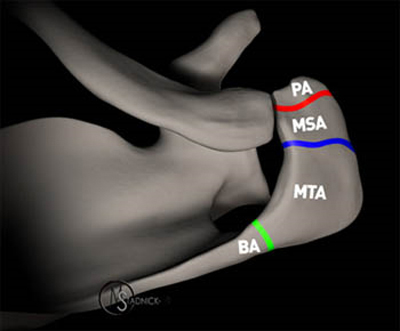
Figure 9:
A view of the scapula from above illustrates a simplified model of the three major ossification centers of the acromion: the preacromion (PA), the mesoacromion (MSA), and the meta-acromion (MTA). The adjacent basi-acromion (BA) of the lateral scapula is also depicted. Failure of fusion can occur at any of the interfaces, but is much more common in the location shown by the blue line. The ossification centers are actually secondary ossification centers which have coalesced from smaller centers, and do not typically display a parallel arrangement as shown in the model. Illustration by Michael E. Stadnick, M.D.
Complete fusion occurs by the ages of 18-25 years according to most studies; however some study reported complete fusion in most children a few years earlier. Overall, the skeletal maturation in girls is earlier than in boys.
A special region of interest is the interface where the primary and secondary ossification centers of the acromion fuse, because this is a site of potential failure of fusion and formation of an os acromiale. The normal boundary between the secondary ossification centers and the rest of the acromion is normally curved and lobulated. It typically extends obliquely and posterolaterally into the acromion towards the posterior angle (Fig. 10), because of a differential growth pattern. A thin physeal scar is sometimes present at the site of fusion and is easily differentiated from a fracture in most cases due to the absence of marrow edema (Fig. 11).
Figure 10:
The normal growth plate between the acromial ossification centers is very thin, multilobulated, and well demarcated, and has low signal (arrowhead) on a fat-suppressed proton density-weighted axial image in a 15 year-old girl. Note the curved and lobulated margin of the growth plate which extends far posterolaterally. The small ossification centers are almost completely fused in the distal acromion (arrowhead).
MRI findings of acromial apophysiolysis
The diagnosis of failure of fusion of the acromion in an adolescent can be challenging. Shoulder radiographs may be normal or show only mild contour irregularity and sclerosis of the acromion at the growth plate. MRI allows more detailed analysis, especially on axial images, regarding the orientation and margins of the growth plate, as well as the marrow signal. In apophysiolysis, the growth plate tends to be linear and transversely oriented with irregular margins (Fig. 12), whereas in the normally developing acromion the growth plate is arched and oblique, and has uniform, lobulated margins (Fig. 10).4 Marrow signal alterations in acromial apophysiolysis include diffuse marrow edema and small foci of hyperintense signal on water sensitive images adjacent to the growth plate (Fig 12, 13). Marrow edema at an unfused ossification center (os acromiale) has been shown to be more common in adults than in teenagers, which may reflect a greater degree of instability of the ossicle in adults.4 The nature of the focal regions of signal abnormality is unclear, but is thought to be related to displaced growth cartilage. The most common level of failure of fusion is between the meta-acromion and mesoacromion. A less frequently seen level of failure is at the distal acromion, between the mesoacromion and preacromion.9
Figure 12:
A T1-weighted axial image with fat suppression shows an irregular growth plate (arrows) which has a transverse orientation rather than the normal oblique orientation, consistent with acromial apophysiolysis. The small rounded foci (arrowheads) of signal abnormality next to the growth plate are probably related to displacement of physeal growth cartilage.
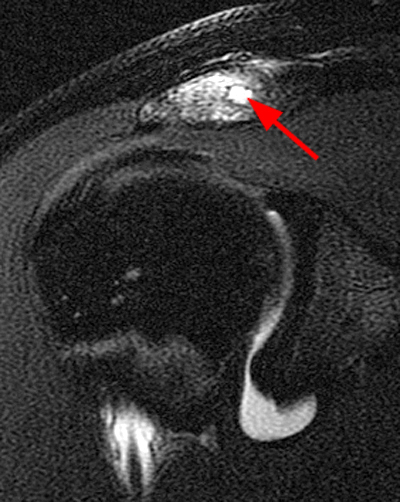
Figure 13:
17 year-old football player with shoulder pain and acromial apophysiolysis after an injury a year ago. A shoulder MR arthrogram was performed. A T2-weighted coronal image with fat suppression reveals diffuse marrow edema of the acromion. The round, well defined focus of hyperintense signal (arrow) is probably related to displacement of growth cartilage which occurred at times of physeal insult.
Complications
Follow up imaging after a minimum of 2 years in a group of patients diagnosed with acromial apophysiolysis showed development of an os acromiale in 86 %. It was not clear from the study if the ossicles were unstable.1
The subsequent risks of shoulder impingement and rotator cuff tears are discussed in the Radsource Web Clinic, August 2007.
Treatment
Treatment of adolescents with acromial apophysiolysis/os acromiale consists of conservative measures such as rest for a period of 2-3 months with cessation of pitching or other sports activity, physical therapy with ice, and oral anti-inflammatory drugs.1,5 If refractory to conservative measures, operative treatment may be considered. Open reduction and internal fixation has been performed successfully in competitive adolescent athletes with os acromiale.6,10 In addition, anterior acromial bone fragments have been excised arthroscopically with good results.11
Differential Diagnosis
Normal red marrow in the acromion in young children may be misinterpreted as marrow edema. The irregularity of individual secondary ossification centers, heterogeneous signal of coalescing ossification centers and physeal scars may present additional pitfalls.
Acute injury to the acromion resulting in acromial contusion and even fractures may resemble the imaging findings in acromial apophysiolysis/os acromiale.
Acute injury to the acromioclavicular joint in a teenager is often associated with diffuse marrow edema which may simulate the MR imaging appearance of acromial apophysiolysis in the setting of an open acromial growth plate (Fig 14 ).
Figure 14:
A 14 year-old boy who fell and injured the shoulder. An axial proton density fat suppressed image shows a small acromioclavicular joint effusion (asterisk), stripping of the acromioclavicular ligaments (arrowheads), and mild diffuse acromial edema. The growth plate of the acromion (arrow) is partially visualized and is normal.
Conclusion
The MR imaging findings of the developing acromion can be confusing due to the presence of a number of secondary ossification centers that vary in morphology and timing of fusion. Recent studies have shown normal fusion of the acromial apophysis at a younger age (16 years) than was previously considered (18-25 years), thus an acromial ossicle should not be generally ignored and called normal in adolescents. Insult to the immature acromion such as repetitive stress in a teenage athlete can result in a delay of or even complete failure of fusion with development of an unstable os acromiale, which is associated with shoulder impingement and rotator cuff tears. Knowledge of the normal stages of the acromial development and abnormalities that occur with physeal stress injury on MR imaging will aid in the prompt and accurate diagnosis, as well as treatment of these patients.
References
- Roedl JB, Morrison WB, Ciccotti MG, Zoga AC. Acromial apophysiolysis: superior shoulder pain and acromial nonfusion in the young throwing athlete. Radiology 2015;274(1): 201–209. ↩
- Scheuer L, Black S, Christie A. The pectoral girdle. In: Developmental juvenile osteology. San Diego, CA: Elsevier Academic Press, 2000; 244–271 ↩
- Flecker H. Roentgenographic observations of the times of appearance of epiphyses and their fusion with the diaphyses. J Anat 1932;67(pt 1):118–164.3. Medline ↩
- Winfeld, Matthew, et al. “Differentiating os acromiale from normally developing acromial ossification centers using magnetic resonance imaging.” Skeletal radiology 44.5 (2015): 667-672. ↩
- Frizziero, Antonio, et al. “Painful os acromiale: Conservative management in a young swimmer athlete.” Journal of sports science & medicine 11.2 (2012): 352. ↩
- Sassmannshausen, G., T. C. Wilson, and S. D. Mair. “Operative stabilization of an unstable os acromiale in an adolescent football player.” orthopaedics 26.5 (2003): 509. ↩
- Kothary, Pratik, and Zehava Sadka Rosenberg. “Skeletal developmental patterns in the acromial process and distal clavicle as observed by MRI.” Skeletal radiology 44.2 (2015): 207-215. ↩
- Macalister, Alexander. “Notes on acromion.” Journal of anatomy and physiology 27.Pt 2 (1893): 244-1. ↩
- Liberson, Frank. “Os acromiale—a contested anomaly.” The Journal of Bone & Joint Surgery 19.3 (1937): 683-689. ↩
- Demetracopoulos, Constantine A., et al. “Surgical stabilization of os acromiale in a fast-pitch softball pitcher.” The American journal of sports medicine 34.11 (2006): 1855-1859. ↩
- Pagnani, Michael J., Chad E. Mathis, and Corey G. Solman. “Painful os acromiale (or unfused acromial apophysis) in athletes.” Journal of shoulder and elbow surgery 15.4 (2006): 432-435. ↩